Archives of Pulmonology and Respiratory Care
Lung cavitation-a rare complication in COVID-19 patients: A case report
1Department of Radiology, Saraswati Hospital, Ahmedabad (380058), Gujarat, India
2Department of Internal Medicine, Saraswati Hospital, Ahmedabad (380058), Gujarat, India
Author and article information
Cite this as
Angirish B, Parmar K (2020) Lung cavitation-a rare complication in COVID-19 patients: A case report. Arch Pulmonol Respir Care. 2020; 6(1): 78-80. Available from: 10.17352/aprc.000061
Copyright License
© 2020 Angirish B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Background: Usually, in clinically cured patients with viral pneumonia, the pulmonary lesions gradually resolve and show complete remission. In very few severe patients, there are residual lesions and fibrosis. Since SARS-CoV-2 is a new disease, the healing process of infected pulmonary lesions is not well known and is variable.
Case presentation: This is a case report of a 51 year old COVID-19 infection patient, who initially presented with ground glass opacities and consolidation but eventually developed large pulmonary cavity and fibrosis in the involved lobes during the course of disease.
Conclusion: Most of the patients infected with SARS-CoV-2 show near complete resolution of the lesions with mild residual opacities, however few patients develop complications in the course of disease.
SARS-CoV-2: Severe Acute Respiratory Syndrome Coronavirus 2; COVID-19: Corona Virus Disease – 2019; RT-PCR: Reverse Transcription-Polymerase Chain Reaction
Background
Coronavirus Disease 2019 (COVID-19) is a pneumonia caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). The outbreak began in Wuhan, China, and spread rapidly, and has been continuing for more than 6 months now [1]. Usually, in clinically cured patients with viral pneumonia, the pulmonary lesions gradually resolve and show complete remission. In very few severe patients, there are residual lesions and fibrosis [2]. Since SARS-CoV-2 is a new coronavirus, the repairative process of SARS-CoV-2 infected pulmonary lesions is not well known. This is a case report of a COVID-19 pneumonia patient, who developed large pulmonary cavity in the course of recovery.
Case presentation
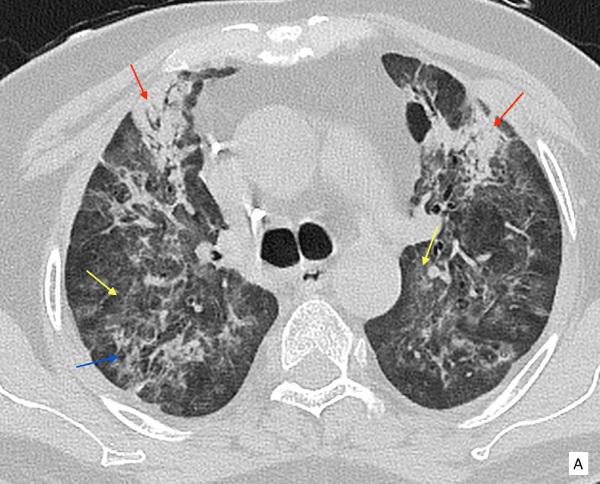
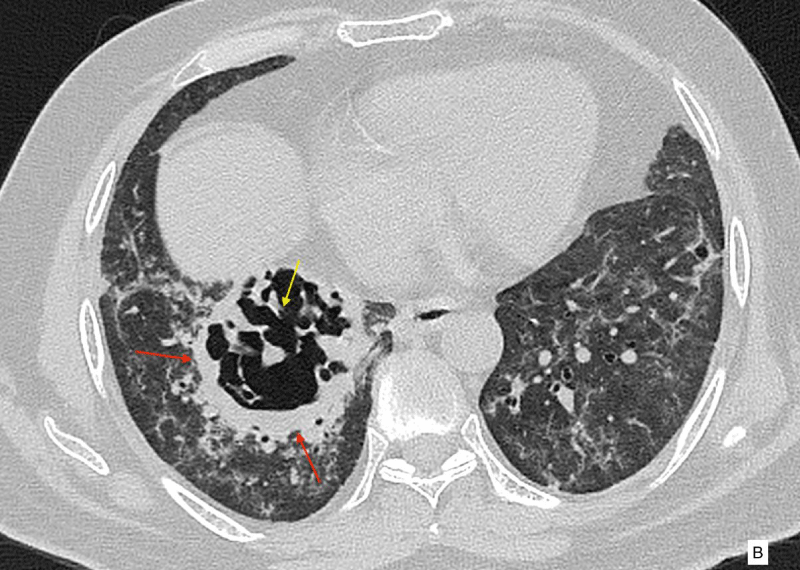
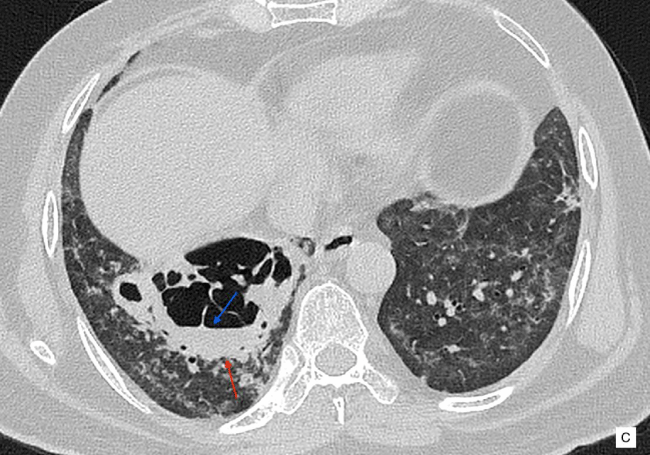
A 51 year old male patient presented with history of cough and fever for 5 days. The patient was a non-smoker, and had no history of tuberculosis. His initial CT scan at the time of admission showed bilateral patchy bronchocentric and subpleural ground glass opacities in both the lungs and consolidation in both lower lobes (images not available). A nasopharyngeal swab specimen was collected which confirmed to be SARS-CoV-2 positive by reverse transcription-polymerase chain reaction (RT-PCR). He was hospitalized, received antiviral, antibacterial therapy, vitamin C and was on oxygen inhalation. After 7-day treatment, the patient’s body temperature returned to normal, symptoms like dry cough and fatigue disappeared, and SpO2 remained between 95% to 99% without oxygen, so he was discharged and was suggested home isolation and treatment. He was doing well for around 3 weeks, after which he started developing mild breathlessness and cough. He visited another hospital. CT re-examination was performed, almost a month after the initial diagnosis of infection, which showed patchy and confluent reticular opacities associated with ground glass opacities and subsegmental consolidation in both the lungs, representing post-COVID-19 infection changes in the lungs with a component of fibrosis (Figure A). A large cavity with internal septations, necrotic parenchyma and internal mild fluid is seen in posterior basal segment of right lower lobe (Figure B,C). There were RT-PCR for SARS-CoV-2 were negative. Bronchoscopy was performed and bronchoalveolar lavage samples had no growth. The possible etiologies of lung cavity such as tuberculosis and fungal infection was ruled out with aggressive blood work-up. There was no history of systemic disoder, connective tissue disorder or neoplasm.
Discussion
The CT findings of COVID-19 pneumonia reflect a typical lung injury pattern seen in viral pneumonia, which is characterized by a rapid change in the imaging patterns as seen in severe acute respiratory syndrome and Middle East respiratory syndrome[1]. As known for most cured viral pneumonia, the lung lesions are gradually absorbed and dissipated, but for COVID-19 infection, the long term imaging pattern is still not known and needs further observation [2].
The typical CT imaging features of COVID-19 include ground-glass opacities, consolidation, reticular opacities, halo and reverse halo sign [3,4]. Cavitation, lymphadenopathy and pleural effusion are known to occur, but are rare presentations[3]. There are cases reported in the literature of development of pulmonary cavity after bacterial infection in the late recovery stage in SARS patients [2].
Lung cavitation following pulmonary embolism and lung infarction is known previously [5,6]. However, lung cavitation due to COVID-19 infection is uncommon to occur. The predominant histopatholgical findings in lungs in most studies were capillary congestion, microthrombi and moderate intra-alveolar fibin exudation corresponding to diffuse alveolar damage [7]. In another observation by , focal hemorrhage in lung tissue, organisation of exudates in alveolar cavities and pulmonary intersitial fibrosis were observed [8]. The exact mechanism of cavitation in COVID-19 patients is unknown and may be related to diffuse alveolar damage, intra-alveolar hemorrhage and necrosis of parenchymal cells as observed in prior autopsy reports [9]. Most cases are managed conservatively, as in our case, the patient was closely monitored on re-admission.
Conclusion
The early and late complications associated with COVID-19 infection are still not completely known and it is a growing spectrum [7]. The presence of cavitary lesions in patients with COVID-19 should be appropriately investigated for superimposed infections, however lung cavitation in the course of COVID-19 infection, should be kept in mind as a spectrum of the disease.
Consent for publication
Patient’s consent was obtained keeping the identity confidental.
Contribution
Case report was written by the corresponding author and all clinical information and data contributed by other author.
Disclosure
• We hereby state that there are no potential conflict of interests (related to any commercial or financial collaboration with the industry).
• We hereby state that there were no previous publications or presentations partly or completely based on the current title/work by me.
- Wang Y, Dong C, Hu Y, Li C, Ren Q, et al. (2020) Temporal changes of CT findings in 90 patients with COVID-19 pneumonia: a longitudinal study. Radiology 296: E55-E64. Link: https://bit.ly/33TCzka
- Chen Y, Chen W, Zhou J, Sun C, Lei Y (2020) Large pulmonary cavity in COVID-19 cured patient case report. Annals of Palliative Medicine. Link: https://bit.ly/3doRGVK
- Chung M, Bernheim A, Mei X, Zhang N, Huang M, et al. (2020) CT imaging features of 2019 novel coronavirus (2019-nCoV). Radiology 295: 202-207. Link: https://bit.ly/2ItWXAa
- Carotti M, Salaffi F, Sarzi-Puttini P, Agostini A, Borgheresi A, et al. (2020) Chest CT features of coronavirus disease 2019 (COVID-19) pneumonia: key points for radiologists. Radiol Med 4: 1-11. Link: https://bit.ly/315qciW
- Teng E, Bennett L, Morelli T, Banerjee A (2018) An unusual presentation of pulmonary embolism leading to infarction, cavitation, abscess formation and bronchopleural fistulation. Case Reports 2018: bcr-2017. Link: https://bit.ly/35c2vXR
- Koroscil MT, Hauser TR (2017) Acute pulmonary embolism leading to cavitation and large pulmonary abscess: a rare complication of pulmonary infarction. Respir Med Case Rep 20: 72-74. Link: https://bit.ly/34TJlG0
- Menter T, Haslbauer JD, Nienhold R, Savic S, Hopfer H, et al. (2020) Post-Mortem examination of COVID19 patients reveals diffuse alveolar damage with severe capillary congestion and variegated findings of lungs and other organs suggesting vascular dysfunction. Histopathology 77: 198-209. Link: https://bit.ly/2Ir5YtD
- Yao XH, Li TY, He ZC, Ping YF, Liu HW, et al. (2020) A pathological report of three COVID-19 cases by minimal invasive autopsies. Zhonghua Bing Li Xue Za Zhi 49: 411-417. Link: https://bit.ly/33XmMRt
- Selvaraj V, Dapaah-Afriyie K (2020) Lung cavitation due to COVID-19 pneumonia. BMJ Case Reports 13: e237245. Link: https://bit.ly/3lITImG
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
