Archives of Renal Diseases and Management
Laparoscopic resolution of Wünderlich syndrome as a primary treatment
Advanced Laparoscopic Department, Andean Clinic of Urology and Italian Hospital, Mendoza, Argentina
Author and article information
Cite this as
Fontana GL, Fontana RL, Guglielmi JM, Bellesty P, López Laur JD (2023) Laparoscopic resolution of Wünderlich syndrome as a primary treatment. Arch Renal Dis Manag. 2023; 8(1): 1-3. Available from: 10.17352/2455-5495.000043
Copyright License
© 2023 Fontana GL, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Background: Spontaneous Retroperitoneal Hemorrhage, named Wünderlich Syndrome (WS) is usually managed by emergency surgeons with a conventional laparotomy. The aim is to report a patient with WS successfully treated by a laparoscopic approach avoiding open surgery.
Methods: A 50-year-old female was diagnosed with WS hemodynamic instability and flank pain. After a normal CT scan that discarded visceral injuries and stabilized, the patient underwent a laparoscopic renal exploration.
Results: Laparoscopic approach was as standard transperitoneal renal access. Fortunately, the hematoma was within Gerota fascia meaning a non-complex surgery. Due to the high R.E.N.A.L. score, it was necessary to complete a radical nephrectomy. Surgical time was 120 minutes without perioperative complications and the renal unit was retrieved using a Pfannenstiel incision. Estimate blood loss was not quantified. Finally, the hospital stay was 24 hrs.
Conclusion: Laparoscopic approach could be performed in selected patients with WS especially when are hemodynamic stabilized with no visceral injury associated. Immediately treatment could facilitate the procedure because it avoids adherences or fibrosis due to hematoma. Experience in the laparoscopic approach is necessary.
Carl Reinhold August Wünderlich described the first case of Spontaneous Retroperitoneal Bleeding in 1856 naming it “renal capsule apoplexy” [1] for the first time, adopting prosperously the definitive denomination of Wünderlich Syndrome (WS) by Coenen in 1910 [2].
This entity is completely rare and almost self-limited in every case; however, about 20% need medical intervention due to hemodynamic decompensation and eventually death in some cases [3,4].
The most frequent etiology is renal tumors such as angiomyolipoma as the first cause in almost 30% followed by Renal Cell Carcinoma (RCC) [5,6]. It is characterized by sudden spontaneous bleeding within the retroperitoneum establishing the Lenk triad of abdominal mass, back pain, and hemodynamic alterations [7], nevertheless, it was a classic representing a quarter of patients [8]. Also, there have been described as a complication in patients with End-stage renal disease that are predisposed to bleeding diathesis in the setting of uremic platelet dysfunction and endothelial abnormalities [9].
The role of urologists depends fundamentally on the hemodynamic status because, in some circumstances, patients are unstable; therefore, general surgeons treat surgically these cases [10] performing a laparotomy and, when the renal unit is affected, radical nephrectomy finally is performed. Therefore, urologists are relegated losing the possibility of repair and even more save the renal unit.
Nevertheless, in selected cases when those patients are clinically stable, treatment options could be active surveillance or renal artery embolization. In cases not counting embolization and the patient continuous bleeding, surgery is obligatory. Currently, the most frequent approach is laparotomy or lumbotomy avoiding minimal invasive surgery that could be performed in selected cases. Infrequent cases or embolization may displace laparoscopy; therefore, the aim is to report a WS with hemodynamic instability that was solved by a laparoscopic approach as a first tool.
Clinical case
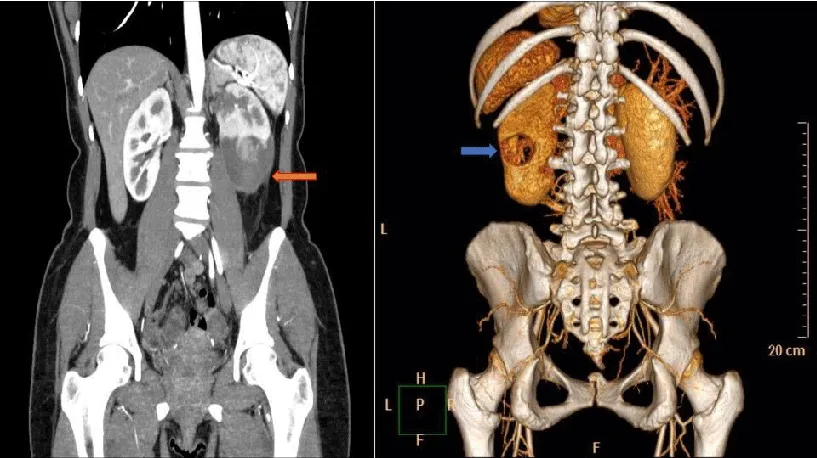
After the patient’s consent respecting her identity and ethical approval by our Institution Committee, we were allowed to report this case. It was about a healthy 50-year-old woman that attended to the emergency room with nontraumatic sudden colic flank pain without other symptomatology. The physical examination demonstrated tachycardia with normal blood pressure. Abdomen examination was painful on the left side and the blood test showed 30% hematocrit, 9.2 hemoglobin with no blood in the urinary sample. A Computer Tomography (CT) scan demonstrated active bleeding inside the Gerota Fascia associated with a 4 cm pure endophytic renal mass (Figures 1A, and 1B, Figure 2). The patient was initially treated conservatively; hence, a few hours later blood pressure decreased suddenly consequently underwent a laparoscopic exploration.
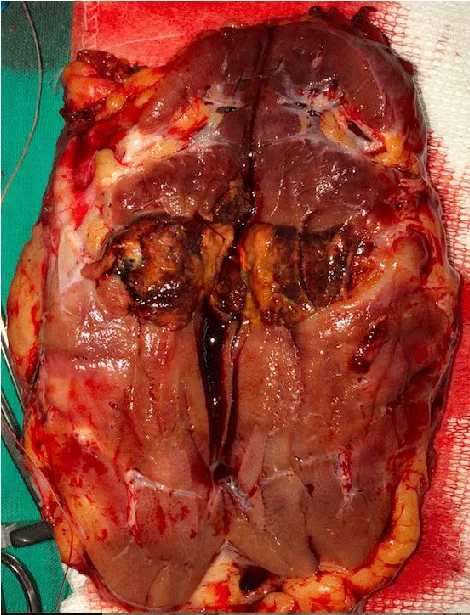
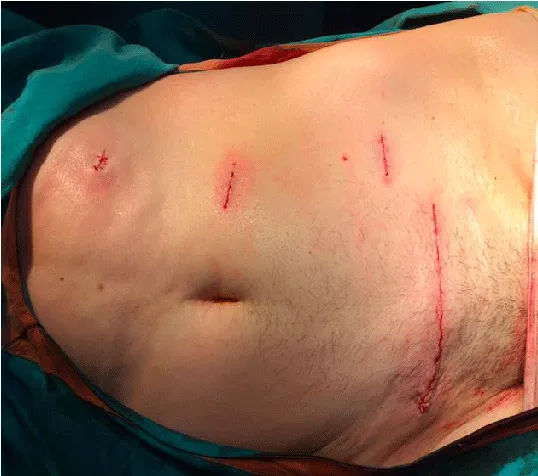
Laparoscopic access was performed as a standard transperitoneal approach. Due to the high R.E.N.A.L. score [11], it was impossible to preserve the renal unit. Fortunately, the hematoma was inside the Gerota Fascia facilitated the procedure using conventional clips de Hemolok ® (Weck Surgical Instruments, Teleflex Medical, Durham, North Carolina) to control the renal hilum. Surgical time was 120 minutes with no bleeding and the specimen retrieval was done using a Pfannenstiel incision (Figure 3). Hospital stay was 24 hs without blood transfusion and the final histopathological findings were 3.8 cm type 2 papillary RCC type.
Discussion
Wunderlich Syndrome (WS) is an interesting clinical condition characterized by the beginning of spontaneous, non-traumatic renal hemorrhage in the sub-capsular and perirenal space. Almost all cases are self-limited needing only conservative management. Nevertheless, in some cases with active bleeding, vascular embolization is highly effective. Unfortunately, urologists do not have an active role in this setting above all when the patient is hemodynamically unstable being general surgeons that treat this pathology [10].
Most approaches are performed by a middle laparotomy to explore the whole abdominal cavity; however, in selected cases when the CT scan demonstrated only renal injury urologist could consider nephron-sparring surgery in a minimally invasive approach.
Even though the laparoscopic approach is considered the standard of care for tumor renal, there are few cases reported of this access for WS probably because of the infrequent cases, hemodynamic instability, or other visceral injured as well [12,13]. Besides, embolization by hemodynamics or general surgeons is those who treat this emergency when is necessary.
Although laparoscopic access for WS is not the standard approach it could be adopted for selective cases such as those hemodynamic stable and without any visceral injured. In the setting, Peña y cols. described 4 cases of WS treated with a deferred laparoscopic approach [12]. The authors remarked the difficult surgery due to intense fibrosis and adherence was probably secondary to having deferred the treatment. In our case, no adherence was found as a conventional laparoscopic nephrectomy considering that surgery as soon as possible could be better. Escudero y Castillo described eight WS, half of them were treated laparoscopically with radical nephrectomy [6]. Recently, Bretterbauer et al. reported a laparoscopic resolution of a WS due to a 10 cm angiomyolipoma in active bleeding [13]. Finally, two cases have been publicized about laparoscopic robot-assisted being able to perform a nephron-sparring surgery in a different and acute setting; respectively [14,15].
Conclusion
Wünderlich Syndrome seems to be feasible and safely treated laparoscopically in selected patients such as no visceral injured associated, hemodynamically stable or stabilized, and, in our opinion, in an acute setting avoiding adherence and intense fibrosis. Therefore, immediate treatment should be considered.
- Wunderlich CR. Handbuch der Pathologie und Therapie, 2nd edn. Stuttgart, Ebner and Seubert. 1856.
- García Rodríguez J, Fernández Gómez JM, Rodríguez Martínez JJ, Rodríguez Faba O, Regadera Sejas J, Escaf Barmadah S. Hemorragia retroperitoneal espontánea por feocromocitoma [Spontaneous retroperitoneal hemorrhage caused by a pheochromocytoma]. Arch Esp Urol. 2002 Oct;55(8):955-8. Spanish. PMID: 12455289.
- Vesga Molina F, Albisu Tristán A, Blasco de Villalonga M, Llarena Ibarguren R, Pertusa Peña C. Hemorragia retroperitoneal espontánea [Spontaneous retroperitoneal hemorrhage]. Arch Esp Urol. 1994 Mar;47(2):129-32. Spanish. PMID: 8002668.
- Katabathina VS, Katre R, Prasad SR, Surabhi VR, Shanbhogue AK, Sunnapwar A. Wunderlich syndrome: cross-sectional imaging review. J Comput Assist Tomogr. 2011 Jul-Aug;35(4):425-33. doi: 10.1097/RCT.0b013e3182203c5e. PMID: 21765296.
- Zhang JQ, Fielding JR, Zou KH. Etiology of spontaneous perirenal hemorrhage: a meta-analysis. J Urol. 2002 Apr;167(4):1593-6. doi: 10.1097/00005392-200204000-00006. PMID: 11912370.
- Molina Escudero R, Castillo OA. Spontaneous retroperitoneal haemorrhage of renal origin (Wunderlich syndrome): analysis of 8 cases. Arch Esp Urol. 2013 Dec;66(10):925-9. English, Spanish. PMID: 24369186.
- Parmar N, Langdon J, Kaliannan K, Mathur M, Guo Y, Mahalingam S. Wunderlich Syndrome: Wonder What It Is. Curr Probl Diagn Radiol. 2022 Mar-Apr;51(2):270-281. doi: 10.1067/j.cpradiol.2020.12.002. Epub 2021 Jan 9. PMID: 33483188.
- Pode D, Meretik S, Shapiro A, Caine M. Diagnosis and management of renal angiomyolipoma. Urology. 1985 May;25(5):461-7. doi: 10.1016/0090-4295(85)90451-0. PMID: 3887727.
- Chamarthi G, Koratala A. Wunderlich syndrome. Clin Case Rep. 2018 Jul 22;6(9):1901-1902. doi: 10.1002/ccr3.1738. PMID: 30214791; PMCID: PMC6132092.
- Rankin T, Echeverria A, Green DJ, McClenathan J. Wunderlich syndrome: the role of the general surgeon. Am Surg. 2015 Mar;81(3):E113-4. PMID: 25760185.
- Kutikov A, Uzzo RG. The R.E.N.A.L. nephrometry score: a comprehensive standardized system for quantitating renal tumor size, location and depth. J Urol. 2009 Sep;182(3):844-53. doi: 10.1016/j.juro.2009.05.035. Epub 2009 Jul 17. PMID: 19616235.
- Peña JA, Serrano M, Cosentino M, Rosales A, Algaba F, Palou J, Villavicencio H. Laparoscopic management of spontaneous retroperitoneal hemorrhage. Urol Int. 2011;87(1):114-6. doi: 10.1159/000324104. Epub 2011 Apr 27. PMID: 21525714.
- Bretterbauer KM, Markić D, Colleselli D, Hruby S, Magdy A, Janetschek G, Mitterberger MJ. Laparoscopic treatment of a spontaneously ruptured kidney (wunderlich syndrome). Case Rep Urol. 2015;2015:701046. doi: 10.1155/2015/701046. Epub 2015 Feb 26. PMID: 25852958; PMCID: PMC4374331.
- Bolufer E, López-Fontana G, Castillo OA. Robot assisted partial nephrectomy (Da Vinci) in an angiomyolipoma associated to Wünderlich Syndrome. Arch Esp Urol. 2012 Nov;65(9):831-4. English, Spanish. PMID: 23154607.
- Ploumidis A, Katafigiotis I, Thanou M, Bodozoglou N, Athanasiou L, Ploumidis A. Spontaneous Retroperitoneal Hemorrhage (Wunderlich Syndrome) due to Large Upper Pole Renal Angiomyolipoma: Does Robotic-Assisted Laparoscopic Partial Nephrectomy Have a Role in Primary Treatment? Case Rep Urol. 2013;2013:498694. doi: 10.1155/2013/498694. Epub 2013 Sep 11. PMID: 24106637; PMCID: PMC3784227.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
