International Journal of Oral and Craniofacial Science
Coronectomy of mandibular third molars with computer-assisted navigated system: A case report
Unit of Oral Surgery, Department of Biomedical and Neuromotor Science (DIBINEM), Alma Mater Studiorum - University of Bologna, Bologna, Italy
Author and article information
Cite this as
Gerardo P, Claudia A, Vignudelli E, Agnese F, Pietro F, et al. (2024) Coronectomy of mandibular third molars with computer-assisted navigated system: A case report. Int J Oral Craniofac Sci. 2024; 10(1): 1-5. Available from: 10.17352/2455-4634.000062
Copyright License
© 2024 Gerardo P, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.The present case report describes a successful surgical case of coronectomy of a fully impacted lower third molar in close relationship with the Inferior Alveolar Nerve (IAN) that was trapped in the furcation roots of the lower third molar. It was associated with a dentigerous cyst. Dynamic Navigation (DN) was used to minimize iatrogenic injuries to the IAN. Coronectomy and cyst removal were successfully performed. High surgical accuracy was provided thanks to the dynamic navigation system that allows the surgeon to perform the procedures without direct vision during the surgery. No neurological damage or other intraoperative complications occurred. One month later, the patient reported a dental abscess to the left mandibular second molar without wound dehiscence which required antibiotic and endodontic therapy. After 2 years, no long-term postoperative complications were reported and follow-up radiographs showed complete bone mineralization. In conclusion, technological support of DN in Coronectomy seems to avoid IAN injury and reduce postoperative complications.
Coronectomy is a surgical option for the treatment of high neurological risk third molars able to reduce iatrogenic nerve injuries [1]. The surgical protocol consists of the removal of the dental crown only, leaving the root undisturbed. This technique was tested in several randomized studies, and a systematic review concluded that coronectomy could be safely used for the treatment of third molars at high neurologic risk. Furthermore, this review suggested the need to improve surgical procedures to reduce the possibility of coronectomy failure [2].
The use of modern technology, specifically Dynamic Navigation (DN) used for implantology, could improve oral and extractive surgeries too [3] DN consists of a stereoscopic camera that detects in real-time the spatial relations of reference tools placed on the patient and on the surgical handpiece as well as software that pairs these with computed tomography images (CBCT). The stereoscopic camera therefore makes all the radiological structures appear in real time, with constant feedback with regard to 3D planning [4,5]. The application of DN in dentistry has improved thanks to the increasing availability of CBCT and the development of more manageable reference tools and software calibrated for dental purposes [6,7].
Moreover, it appears to be particularly helpful in rehabilitating atrophic jaws by avoiding graft procedures, with the insertion of zygomatic, pterygoid, or inclined implants. DN technology also seems to improve the accuracy of implant positioning, independent of the clinician’s experience [5,8]. Recently, this technology enabled a dental student to successfully perform endodontic surgery through a minimally invasive approach [9].
In oral surgery, there are only two relevant case reports [10,11]. One retrospective review [12] regarding computer-assisted dental extractions is by Emery, et al. [12], focusing only on the removal of the M3M, and cases of displaced teeth or foreign body retrieval [10,13,14] where DN has been applied. DN was shown to be manageable and versatile in all components of these procedures with minimal discomfort for the surgeon [5].
The present study reports one case of the Coronectomy of the third molar impacted and in close proximity to the mandibular canal, using the DN system to improve the accuracy of the procedure.
Case presentation
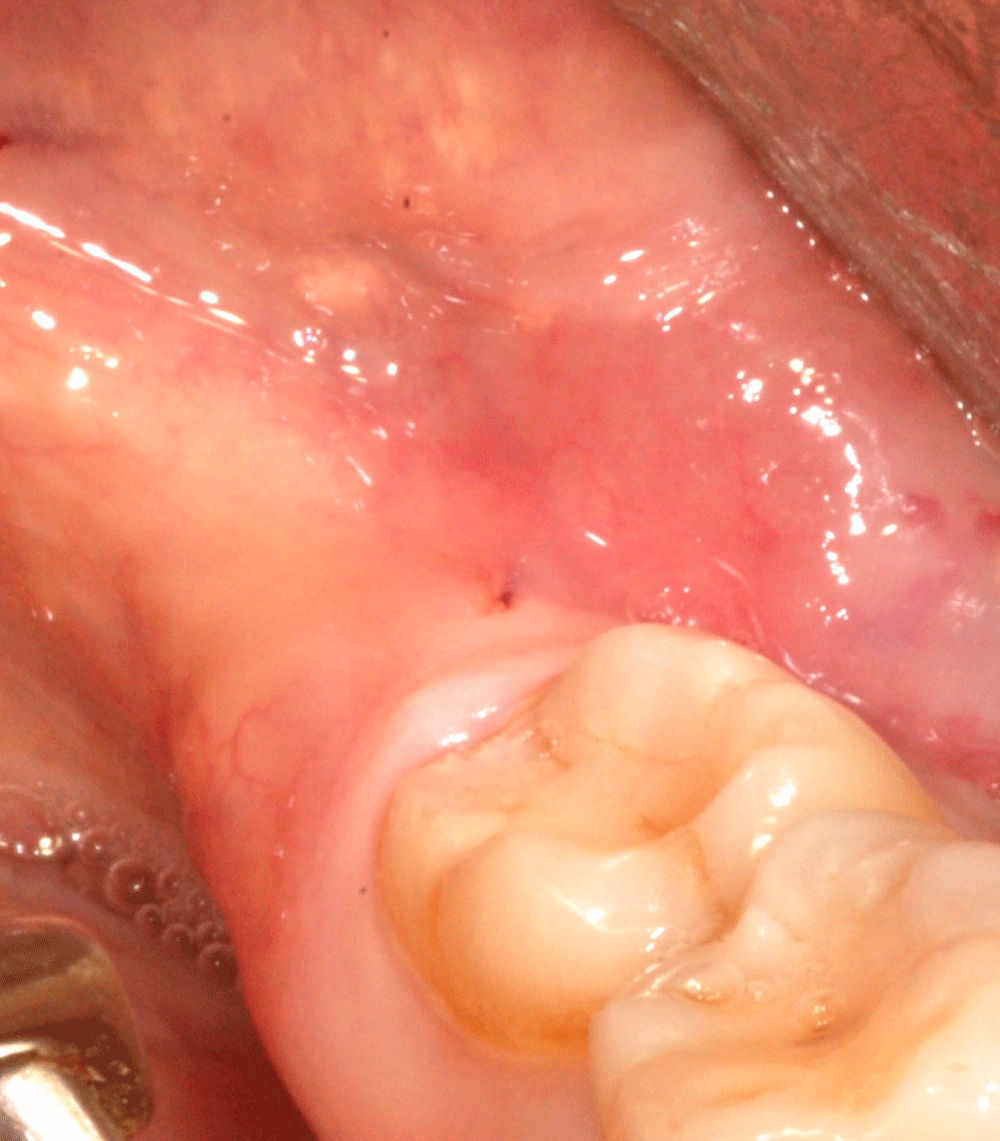
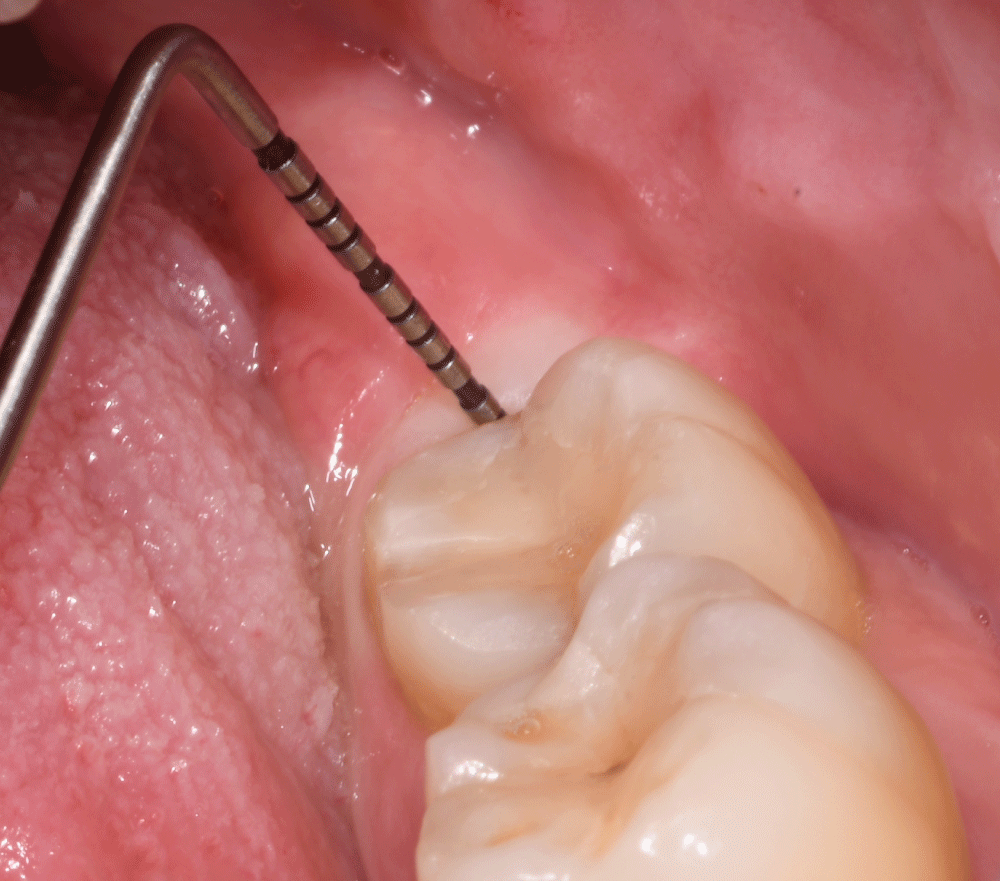
A 42-year-old woman was referred to the Unit of Oral Surgery of the Department of Biomedical and Neuromotor Sciences (DIBINEM) of the University of Bologna, Italy for the treatment of an impacted mandibular third molar. The study purpose and process were explained to patients and informed consent was obtained. The study was conducted in accordance with the Declaration of Helsinki and Strengthening the Reporting of Observational Studies in Epidemiology statement, and the study protocol was approved by the Ethics Committee Azienda Unità Sanitaria Locale Città di Bologna, Italy (Comitato Etico 12098, 2012). The patient reported recurrent pericoronitis requiring antibiotic therapy. Clinically, the third molar was deeply impacted with Pathological Probing Depth (PPD), complete with the presence of bleeding on probing (BOP) (Figure 1).
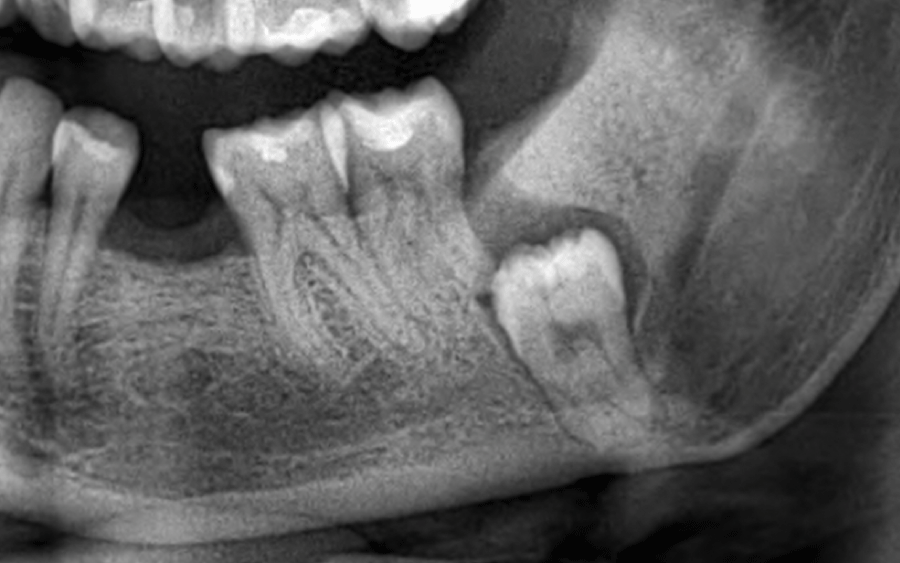
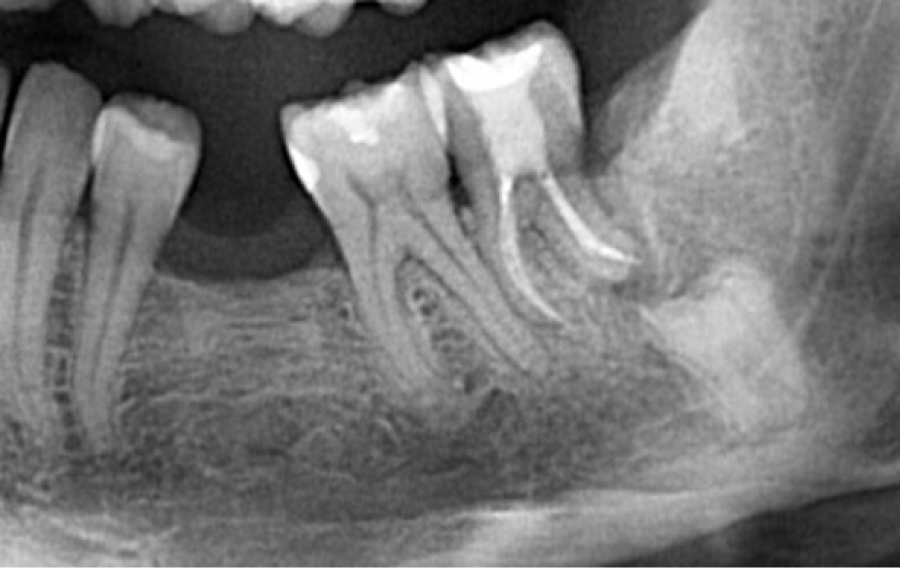
The panoramic radiograph showed a vertically impacted left lower third molar classified as IC grade according to the Pell and Gregory scale [15] (Figure 2).
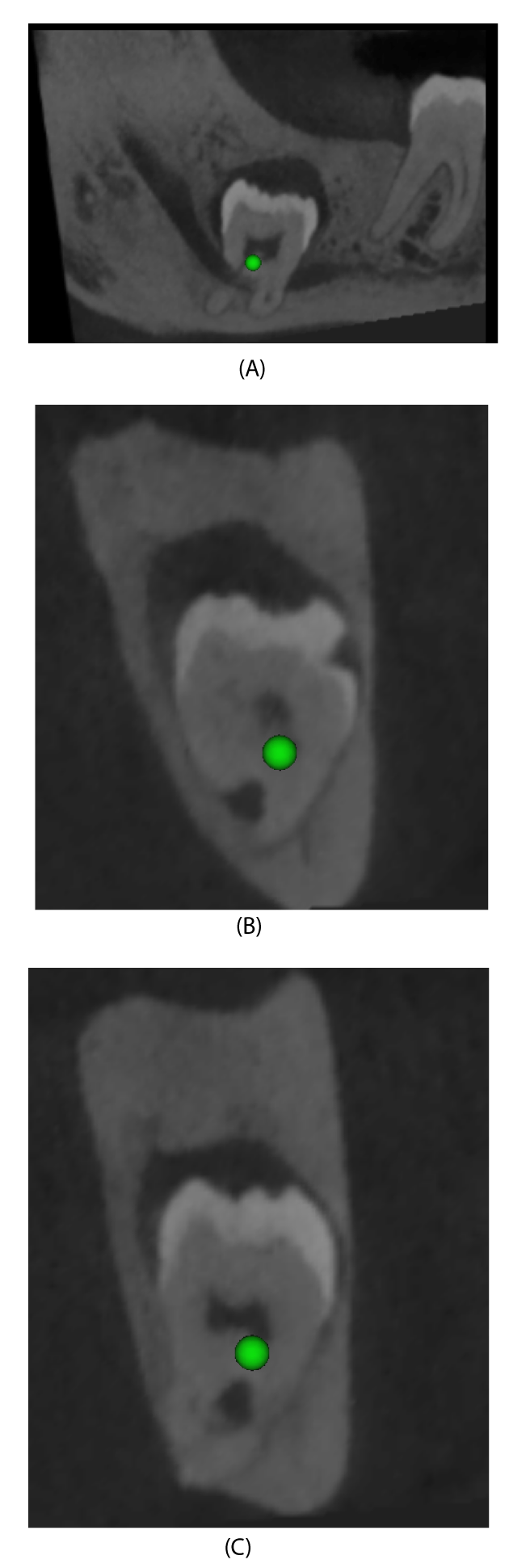
Panoramic radiographs also showed the presence of a dentigerous cyst and radiographic risk factor for alveolar nerve injuries [16,17]. CBCT examination showed the inferior alveolar nerve trapped in the furcation roots of the lower third molar. (Figure 3a-3c)
High neurological risk along with a few technical operative difficulties, and the resolute patient’s request for a semi-invasive and rapid treatment corroborated the decision to perform coronectomy with the DN technology.
The ImplaNav (BresMedical, Sydney, Australia) navigation system was used and all stages of the operating protocol were performed. Preoperative CBCT scans were taken with a reference plate placed in the oral cavity (for dentate patients) containing fiducial markers (also called a marker plate [MP]). In a similar fashion to an impression tray, this reference plate was anchored to the dental arcade with a high-density impression material Ramitec; 3M ESPE, USA). The impression involved three healthy teeth, and the zone of anchorage was chosen by previewing the spatial interference of the MP with the surgical handpiece. After the CBCT scans were taken, the reference system was removed and stored, to be positioned in situ during the surgical procedure. The DICOM files were imported into the navigation software, enabling the assessment and mapping of the dental anatomy, mandibular canal pathway, and tooth crown, and following the position of the burr.
On the day of surgery, after local anesthesia to block the IAN, the MP was again placed in situ; this time, however, the patient reference tool (RTp) was kept attached. The RTp consists of reflective spheres aligned on a support in a predefined geometric pattern in such a way that it can be localized by the firmware of an infrared digital camera [NDI], Waterloo, Canada), and segmented while in progress in the 2D images obtained from the frame. A second handle reference tool (RTh) was attached through an adaptable joint to the contra-angle handpiece and to the ultrasonic handle. This specific joint has a spherical connection that allows the surgeon to locate the camera wherever it is ergonomically comfortable, providing a direct view of the surgical field and, at the same time, the screen. In order to carry out the registration/calibration process, the operator exposed (for at least 3 s) the RTh attached to the handpiece of the camera that matched it with the RTp. Then, the fiducial markers on the MP were touched in sequence with a lancet drill (calibration tool) to enable the software to superimpose the surgical tips’ position and axis to the 3D patient radiological image.
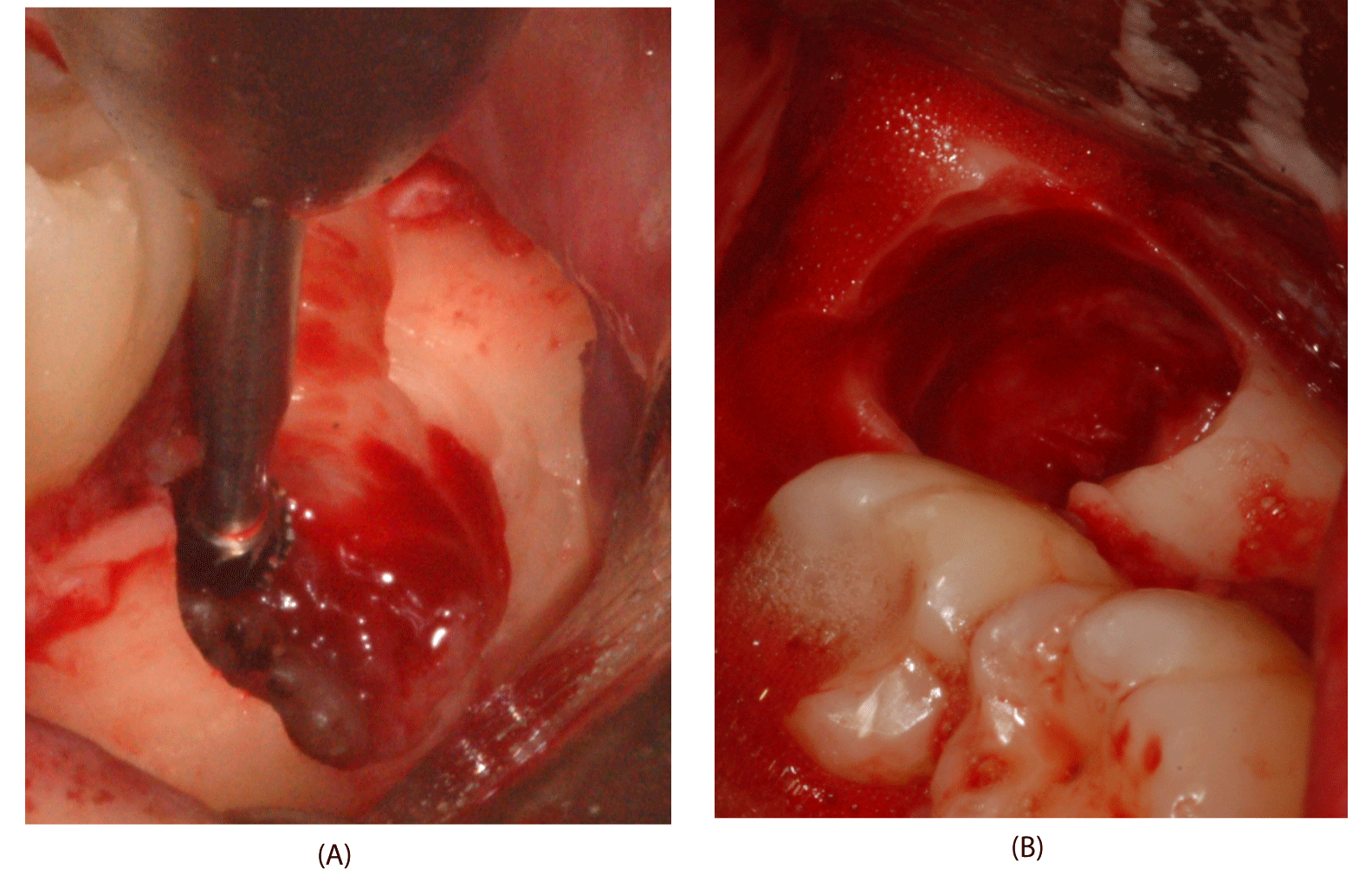
A mucoperiosteal buccal flap, with a releasing incision mesial to the second molar and a distobuccal one, was incised and raised. Then, the tracking array was placed so the surgeon could perform the planned surgical procedures for osteotomy and odontotomy with the navigation system guide (Figure 4). DN displayed the position of the rotating or ultrasonic tip on the computer monitor in real-time, overlaid with the CBCT images in the three spatial planes.
A circumferential ostectomy of the spongiosa was performed with the straight insert on the ultrasonic handpiece (Surgysonic Moto; Esacrom, Imola, Italy) to remove buccal bone; a crown section was accomplished via a spear bur, which was constantly tracked on the DN monitor. The section is performed in a bucco-lingual and mesio-distal direction. The dentigerous cyst was raised to the bone and removed using an alveolar spoon. The crown was gently fractured using an elevator inserted between the buccal bony crest and the tooth. The crown fragments were removed using only the forceps along the straight pathway toward the occlusal plane.
After the crown’s removal, the remaining roots were reduced by at least 2 mms - 3 mms [18]. The grinding of the roots was performed using a round bur or a drill to make a smooth surface without dentinal or enamel spikes. A periapical radiograph was taken to control the crown section before suturing [19].
The post-operative migration of retained roots is a common and well-documented finding in literature [1,20,21]. The residual alveolus and roots were revised and irrigated with saline solution.
The surgery was carried out within 40 minutes, timed from the use of the first instrument to the completion of the suturing. After surgery, nonsteroidal analgesic medication was prescribed, to be taken only in case of pain and swelling. The patient was instructed to adhere to a soft diet for a few days, to maintain appropriate oral hygiene, and to rinse daily with a 0.2% chlorhexidine mouthwash. No immediate postoperative discomfort such as bleeding, swelling, or pain occurred. One month later, the patient reported a dental abscess to the left mandibular second molar without wound dehiscence which required antibiotic therapy. Root canal therapy was necessary for the left second molar. Three months later, no complications were recorded and the site completely healed. A year after the surgery, the soft tissue was completely healed, and bleeding on probing and probing depth was physiological. Two years after the surgery, a panoramic radiograph showed new bone formation distal to the second molar (Figure 5). The probing depth distal to the second molar was reported to be 3mm buccal, 3 mm medial, and 3mm distal (Figure 6).
Discussion
The objective of this study was to describe the Coronectomy of complex mandibular third molars in close relationship with IAN, using in-office dynamic computer navigation.
Removal of deeply impacted lower third molars can lead to several temporary or permanent complications. One of the most embarrassing complications is IAN injury during the procedure, which may impair nerve function for an unpredictable period, or even permanently. Impairment of the IAN ranges from 0.1% to 5.3% [22] or up to 17% and the LN from 0.1% to 22% [23].
Coronectomy is a surgical option to avoid that outcome when there is a close relationship between tooth roots and the IAN, for the protection of the IAN [1].
In the presented case, this procedure showed to be quite beneficial not only for avoiding IAN injury but also for a possible fracture of the mandible, as the tooth occupied the angle mandibular. Every year for 5 years, the residual roots are checked with Orthopantomography.
DN technology can avoid IAN injury and reduce postoperative complications due to the precise control of the surgical tools in relation to the radiologic anatomy. In the reported case, the age of the patient (42 years), tooth position, morphology, and IAN position were considered risk factors for achieving these goals, with the possibility of protracted surgery time and postoperative complications. To our knowledge, this is the first description of using dynamic navigation for the coronectomy of third molars.
The majority of office-based computer-navigated surgery is performed for the placement of dental implants using static navigation. DN technology makes it possible to reduce the learning curve in implantology after a period of proper practice. It has been reported that it takes about 10 to 20 implant placements with DN technological support to optimize the surgeon’s accuracy [12].
Thanks to the accessibility of cone beams, computed tomography has allowed oral and maxillofacial surgeons to utilize computer-assisted surgery in an office environment.
Golob Deeb, et al. [24] observed that novices obtained an implant positioning accuracy comparable to that of experienced operators within three attempts. Different studies have demonstrated better accuracy in implant positioning with a DN-supported insertion than with a freehand approach [25]. This can be helpful in general oral surgery. In a retrospective survey by Emery et al.1, covering the period between 2010 and 2014, the authors reported fewer complications after the extraction of M3Ms with DN technology. For this reason, increasing the use of this system, which is more sophisticated and manageable today, could be realistically considered. The same authors showed reduced surgical time with improved visualization of the surgical field, even though this was not scientifically demonstrated [12].
Importantly, the technology adopted by the present authors eliminated the requirement of cranial anchorage, thanks to a mini-implant placed in the premaxillary zone as the patient connection for both the reference tool and fiducial markers; this also allows the application of DN in totally edentulous patients. (Accuracy valuation using mini-implants remains to be conducted). The bearing of an extraoral fiducial MP avoids fiducial screw insertion in the jawbone, drastically reducing the invasiveness of the procedure. Optical array interferences are unavoidable drawbacks and point to the need for an observant operator and a well-trained surgical team. Another limiting factor of DN-supported extraction of third molars, as pointed out by Emery, et al. [12], is the inability to locate the tooth after it has been luxated because its position shifts from that in the presurgical CBCT. This could cause teeth to be dangerously dislocated and to lodge in inappropriate anatomical spaces.
The shortcomings of the system reported by Emery, et al. [12] are today overcome by less bulky instrumentation, as well as the reduction of the surgical tracking volume and the stability of the patient tracking array.
As in all surgical fields, new technology requires dental surgeons to consider a multidisciplinary approach that involves teamwork and implies the sharing of medical knowledge and information, as well as professional and technical competencies. Perhaps, increased costs and certain habitual changes have to be accepted. DN technology means much more time spent on surgical planning on a screen and keyboard rather than on the patient, changing surgical situations and ergonomic positions, improving teamwork, and taking better account of the diagnostic phase.
Conclusion
The technological support of DN in Coronectomy can avoid IAN injury and reduce postoperative complications. The DN system used in the present study resulted in a more manageable and ergonomic technology, thanks to the intraoral connection of both the reference tool and the fiducial marker.
Future clinical trials are needed to confirm the real advantages of DN technology in the domain of oral surgical procedures.
- Monaco G, de Santis G, Gatto MR, Corinaldesi G, Marchetti C. Coronectomy: a surgical option for impacted third molars in close proximity to the inferior alveolar nerve. J Am Dent Assoc. 2012 Apr;143(4):363-9. doi: 10.14219/jada.archive.2012.0178. PMID: 22467696.
- Martin A, Perinetti G, Costantinides F, Maglione M. Coronectomy as a surgical approach to impacted mandibular third molars: a systematic review. Head Face Med. 2015 Apr 10;11:9. doi: 10.1186/s13005-015-0068-7. PMID: 25890111; PMCID: PMC4397866.
- Pellegrino G, Lizio G, Ferri A, Marchetti C. Flapless and bone-preserving extraction of partially impacted mandibular third molars with dynamic navigation technology. A report of three cases. Int J Comput Dent. 2021 Sep 23;24(3):253-262. PMID: 34553890.
- Siessegger M, Mischkowski RA, Schneider BT, Krug B, Klesper B, Zöller JE. Image guided surgical navigation for removal of foreign bodies in the head and neck. J Craniomaxillofac Surg. 2001 Dec;29(6):321-5. doi: 10.1054/jcms.2001.0254. PMID: 11777348.
- Pellegrino G, Taraschi V, Vercellotti T, Ben-Nissan B, Marchetti C. Three-Dimensional Implant Positioning with a Piezosurgery Implant Site Preparation Technique and an Intraoral Surgical Navigation System: Case Report. Int J Oral Maxillofac Implants. 2017 May/Jun;32(3):e163-e165. doi: 10.11607/jomi.5800. PMID: 28494042.
- Block MS, Emery RW, Lank K, Ryan J. Implant Placement Accuracy Using Dynamic Navigation. Int J Oral Maxillofac Implants. 2017 Jan/Feb;32(1):92-99. doi: 10.11607/jomi.5004. Epub 2016 Sep 19. PMID: 27643585.
- Kramer FJ, Baethge C, Swennen G, Rosahl S. Navigated vs. conventional implant insertion for maxillary single tooth replacement. Clin Oral Implants Res. 2005 Feb;16(1):60-8. doi: 10.1111/j.1600-0501.2004.01058.x. PMID: 15642032.
- Stefanelli LV, DeGroot BS, Lipton DI, Mandelaris GA. Accuracy of a Dynamic Dental Implant Navigation System in a Private Practice. Int J Oral Maxillofac Implants. 2019 January/February;34(1):205–213. doi: 10.11607/jomi.6966. Epub 2018 Dec 5. PMID: 30521660.
- Gambarini G, Galli M, Stefanelli LV, Di Nardo D, Morese A, Seracchiani M, De Angelis F, Di Carlo S, Testarelli L. Endodontic Microsurgery Using Dynamic Navigation System: A Case Report. J Endod. 2019 Nov;45(11):1397-1402.e6. doi: 10.1016/j.joen.2019.07.010. Epub 2019 Sep 10. PMID: 31515047.
- Wang J, Cui NH, Guo YJ, Zhang W. Navigation-Guided Extraction of Impacted Supernumerary Teeth: A Case Report. J Oral Maxillofac Surg. 2017 Jun;75(6):1136.e1-1136.e5. doi: 10.1016/j.joms.2017.02.001. Epub 2017 Feb 14. PMID: 28279686.
- Retana A, Emery RW, Keir V. Removal of Impacted Supernumerary Teeth Using a Dynamic Surgical Navigation System: A Case Report. J Oral Maxillofac Surg. 2019 Jun;77(6):1130-1134. doi: 10.1016/j.joms.2019.01.012. Epub 2019 Jan 14. PMID: 30738066.
- Emery RW, Korj O, Agarwal R. A Review of In-Office Dynamic Image Navigation for Extraction of Complex Mandibular Third Molars. J Oral Maxillofac Surg. 2017 Aug;75(8):1591-1600. doi: 10.1016/j.joms.2017.03.031. Epub 2017 Mar 25. PMID: 28419843.
- Gerbino G, Zavattero E, Berrone M, Berrone S. Management of needle breakage using intraoperative navigation following inferior alveolar nerve block. J Oral Maxillofac Surg. 2013 Nov;71(11):1819-24. doi: 10.1016/j.joms.2013.07.023. PMID: 24135518.
- Lee TY, Zaid WS. Broken dental needle retrieval using a surgical navigation system: a case report and literature review. Oral Surg Oral Med Oral Pathol Oral Radiol. 2015 Feb;119(2):e55-9. doi: 10.1016/j.oooo.2014.08.019. Epub 2014 Sep 16. PMID: 25442246.
- Pell GJ, Gregory BT. Impacted mandibular third molars: classification and modified technique for removal. Dent Digest; 1933; 39:330–338;
- Monaco G, Montevecchi M, Bonetti GA, Gatto MR, Checchi L. Reliability of panoramic radiography in evaluating the topographic relationship between the mandibular canal and impacted third molars. J Am Dent Assoc. 2004 Mar;135(3):312-8. doi: 10.14219/jada.archive.2004.0179. PMID: 15058618.
- Jerjes W, Upile T, Kafas P, Abbas S, Rob J, McCarthy E, McCarthy P, Hopper C. Third molar surgery: the patient's and the clinician's perspective. Int Arch Med. 2009 Oct 24;2(1):32. doi: 10.1186/1755-7682-2-32. PMID: 19852848; PMCID: PMC2772836.
- Monaco G, Vignudelli E, Diazzi M, Marchetti C, Corinaldesi G. Coronectomy of mandibular third molars: A clinical protocol to avoid inferior alveolar nerve injury. J Craniomaxillofac Surg. 2015 Oct;43(8):1694-9. doi: 10.1016/j.jcms.2015.07.006. Epub 2015 Jul 29. PMID: 26321069.
- Monaco G, De Santis G, Pulpito G, Gatto MR, Vignudelli E, Marchetti C. What Are the Types and Frequencies of Complications Associated With Mandibular Third Molar Coronectomy? A Follow-Up Study. J Oral Maxillofac Surg. 2015 Jul;73(7):1246-53. doi: 10.1016/j.joms.2015.01.016. Epub 2015 Jan 29. PMID: 25914134.
- Leung YY, Cheung LK. Safety of coronectomy versus excision of wisdom teeth: a randomized controlled trial. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009 Dec;108(6):821-7. doi: 10.1016/j.tripleo.2009.07.004. Epub 2009 Sep 26. PMID: 19782621.
- Leung YY, Cheung LK. Coronectomy of the lower third molar is safe within the first 3 years. J Oral Maxillofac Surg. 2012 Jul;70(7):1515-22. doi: 10.1016/j.joms.2011.12.029. Epub 2012 Apr 10. PMID: 22494507.
- Tolstunov L, Javid B, Keyes L, Nattestad A. Pericoronal ostectomy: an alternative surgical technique for management of mandibular third molars in close proximity to the inferior alveolar nerve. J Oral Maxillofac Surg. 2011 Jul;69(7):1858-66. doi: 10.1016/j.joms.2011.03.002. Epub 2011 May 6. PMID: 21549479.
- Leung YY, Cheung LK. Risk factors of neurosensory deficits in lower third molar surgery: an literature review of prospective studies. Int J Oral Maxillofac Surg. 2011 Jan;40(1):1-10. doi: 10.1016/j.ijom.2010.09.005. Epub 2010 Oct 28. PMID: 21035310.
- Golob Deeb J, Bencharit S, Carrico CK, Lukic M, Hawkins D, Rener-Sitar K, Deeb GR. Exploring training dental implant placement using computer-guided implant navigation system for predoctoral students: A pilot study. Eur J Dent Educ. 2019 Nov;23(4):415-423. doi: 10.1111/eje.12447. Epub 2019 Jun 13. PMID: 31141291.
- Aydemir CA, Arısan V. Accuracy of dental implant placement via dynamic navigation or the freehand method: A split-mouth randomized controlled clinical trial. Clin Oral Implants Res. 2020 Mar;31(3):255-263. doi: 10.1111/clr.13563. Epub 2019 Dec 29. PMID: 31829457.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
