International Journal of Oral and Craniofacial Science
Zygomatic complex fractures in a Nigerian tertiary hospital: An update on the pattern of presentation and care
1Associate Professor, Consultant, Oral and Maxillofacial Surgery, Ekiti State University Teaching Hospital, Ado-Ekiti, Nigeria
2Associate Professor/ Consultant Otorhinolaryngologist, Ekiti State University Teaching Hospital, Ado-Ekiti, Nigeria
3Consultant Oral and Maxillofacial Surgery, Federal Teaching Hospital, Ido-Ekiti, Nigeria
4Consultant Oral Medicine, Federal Teaching Hospital, Ido-Ekiti, Nigeria
5Senior Dental Officer, Ekiti State University Teaching Hospital, Ado-Ekiti, Nigeria
Author and article information
Cite this as
Obimakinde OS, Olajuyin OA, Akinbade AO, Ojo KO, Ibidun CO, et al. (2022) Zygomatic complex fractures in a Nigerian tertiary hospital: An update on the pattern of presentation and care. Int J Oral Craniofac Sci. 2022; 8(2): 36-41. Available from: 10.17352/2455-4634.000058
Copyright License
© 2022 Obimakinde OS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Aim: The Zygomatic complex [ZMC], being one of the most commonly fractured bones in the facial skeleton, is largely underreported in the literature. This study was designed to evaluate the pattern of fractures, symptomatology, and treatment modalities at our institution.
Materials and methods: Information on patients’ sociodemographics, the pattern of fractures, symptomatology, radiologic diagnosis, and treatment modalities were accessed from patients’ records on our trauma register. Data collected was analyzed with SPSS 20 and the level of significance was set at p < 0.05.
Results: A total of 105 patients aged 19-66 years had ZMC fractures during the study period. A male preponderance was observed [M: F = 3.8:1] and road traffic crashes [RTC] accounted for the majority of fractures [79.0%]. There was a statistically significant relationship between RTC and fractures among the age groups [X2 = 33.61, df = 5, p = 0.001]. Fractures at the zygomatico-frontal [ZF] and in combination with zygomaticomaxillary [ZM] sutures were the commonest finding on imaging [39.1% % 28.6% respectively]. Subconjunctival and circumorbital ecchymosis [92.4% and 91.4% respectively] were the commonest symptomatology. Eighty four patients (80 %) were managed via surgical intervention and the most commonly employed surgical modality was mini plates [1.0mm] fixation across either ZF [n = 33, 39.3%] or ZM [n = 21, 25.0%] suture lines.
Conclusion: This study revealed that RTC remains a major aetiology of ZMC fractures and mini plate ostheosynthesis was the mainstay of surgical management. Enforcement of road safety regulations on speed and the use of protective measures by road users is imperative.
The zygomatic [ZMC] complex plays a key role in the structure, function, and esthetic appearance of the facial skeleton [1]. It is responsible for the mid-facial contour and the protection of orbital contents [1-3]. The ZMC, being a major buttress of the facial skeleton is often predisposed to fracture because of its prominence [1-3]. ZMC fractures are among the most frequently encountered in the maxillofacial region and some of the aetiologies include road traffic crashes, assaults, falls, sports, and missile injuries [2-4]. Although Road Traffic Crashes [RTC] are generally regarded as the major etiological factor of maxillofacial injuries in this part of the globe, some studies, however, revealed that injuries due to assault are more prevalent in some developed countries [5-7]. The relative contribution of these etiologic factors in different studies is largely dependent on the sociocultural and geographic peculiarities of the populations studied [3,5-8].
ZMC fractures are commonly associated with a wide range of symptoms and those that have been described include diplopia, subconjunctival ecchymosis, flattening of the cheek, hooding of the globe, enophthalmous and sometimes sensory disturbance [2,7-10]. Management of ZMC fractures has received divergent opinions in the literature [3,10-12]. Some authors opined that undisplaced fractures or those with minimal displacement should be treated non-operatively, whereas fractures with functional or esthetic impairments in the form of diplopia, extraocular muscle entrapment, malocclusion, restricted mouth opening and/or depression of the malar prominence should necessitate surgical intervention [5-8,11-14].
Generally, there is a dearth of studies on ZMC fractures in sub-Saharan Africa probably due to the overriding influence of other facial injuries such as mid-face fractures of the Le Fort type and mandibular fractures. The previous efforts by Adekeye [8], Obuekwe and Owotade [3], from this environment only provided limited information mostly on the etiology and pattern of presentation. In order to scale up the existing information from these studies, the current study was therefore designed to evaluate the pattern of presentation and management modalities of ZMC fractures in our institution. We also aimed to compare our findings to similar works globally.
Materials and methods
Over a ten-year period [January 2010 to December 2019], the data of patients who sustained Zygomatic fractures were collected on individual proforma and added to our trauma register. Patients with other forms of maxillofacial injury without ZMC fractures were excluded from the study. The patients presented through either the Accident and emergency unit or the maxillofacial surgery clinic of our institution which is a major referral center in southwestern Nigeria. Ethical approval was obtained from our institution’s ethical review committee.
Information on patients’ sociodemographics [age, sex and occupation], aetiology, the pattern of fractures, clinical findings, and radiologic diagnosis were accessed from patients’ individual records on our trauma register. Other data documented were the associated injuries, clinical presentation, and modality of definitive treatment.
Diagnosis of Zygomatic fractures was achieved through clinical and radiologic evaluation. All patients in this series had either plain radiographs [occipitomental or submentovertex] or Computerized Tomography Scans [CT scan] for radiologic evaluation. The diagnosis was confirmed by the presence of bony discontinuity during radiologic evaluation.
Data obtained were summarized in frequency tables and analyzed using SPSS statistical software package version 20. Descriptive statistics and a Chi-square test were carried out and the level of significance was set as p < 0-05.
Result
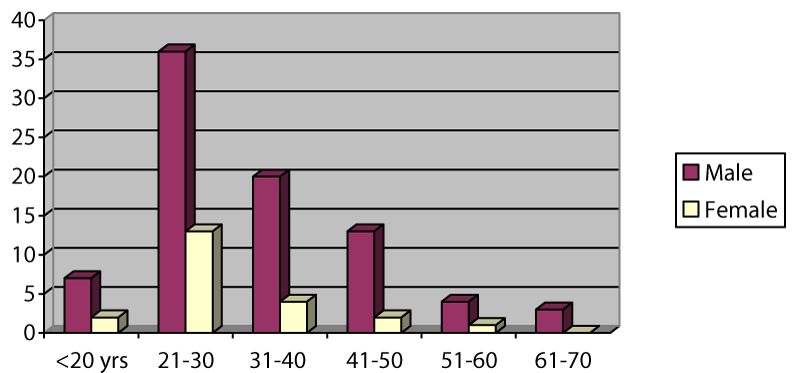
A total of 105 patients with zygomatic complex fractures were evaluated during the study period. There was a male preponderance of 83 to 22 [M: F = 3.8:1]. The age range of the subjects was 19-66 years with a mean age of 31 ± 12.6 years and those in the age group 21-30 years [46.7%] constituted the majority of the patient population (Figure 1). Regarding the aetiology of ZMC fractures (Table 1); road traffic crashes [RTC] accounted for the majority of fractures and there was a statistically significant relationship between RTC and fractures among the age groups [X2 = 33.61, df = 5, p = 0.001]. However, the patient’s gender did not have any statistically significant relationship with RTC [X2 = 3.02, df = 1, p = 0.13].
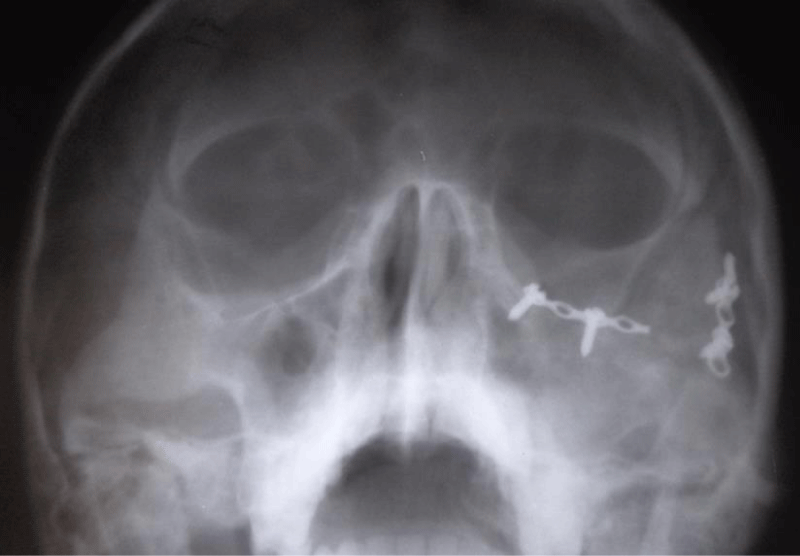
Unilateral fracture [n = 96, 91.4%] was the most common presentation and the right zygoma [n = 55, 57.3%] was the more commonly affected side (Table 2). The Pattern of zygomatic complex fractures revealed that bony discontinuity occurred mostly along the suture lines of the articulation of the zygomatic bone with the frontal, temporal and maxillary bones (Table 3). Forty-one patients [39.1%] had isolated fracture involving the zygomatico-frontal [ZF] suture while fractures involving both zygomatico-frontal [ZF] and zygomaticomaxillary [ZM] sutures simultaneously was the next most prevalent [n = 30, 28.6%]. Fractures involving only the ZM suture line were the least encountered among the patients [n = 20, 19.1%]. Two patients suffered a gross comminuted fracture of the zygomatic bone while there were two cases of fracture involving both the zygomatic bone and arch respectively.
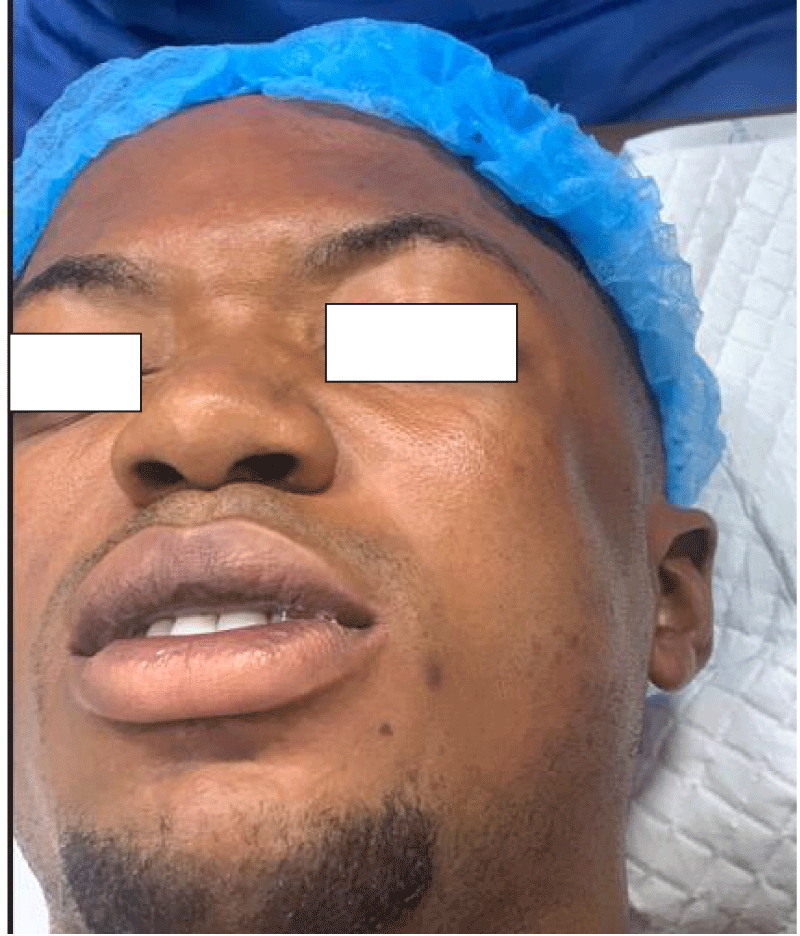
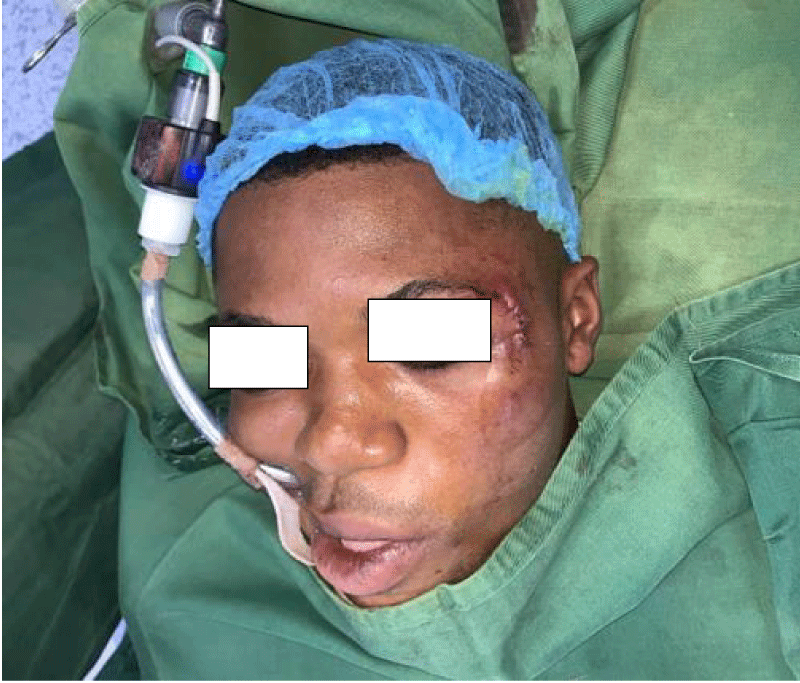
The symptomatology of zygomatic fractures was presented in Table 4 and nearly all the patients, with the exception of those who had isolated Zygomatic arch fracture, presented with subconjuctival and circumorbital ecchymosis [92.4% and 91.4% respectively]. Flattening of the cheekbone was the third commonest symptom [67.6%] while sensory disturbance involving the infraorbital nerve [17.1%] was the least encountered among the subjects.
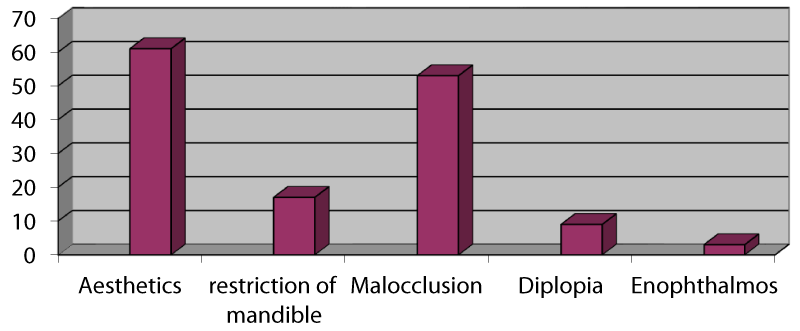
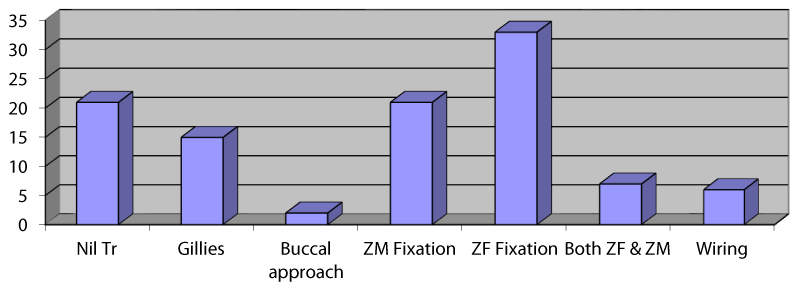
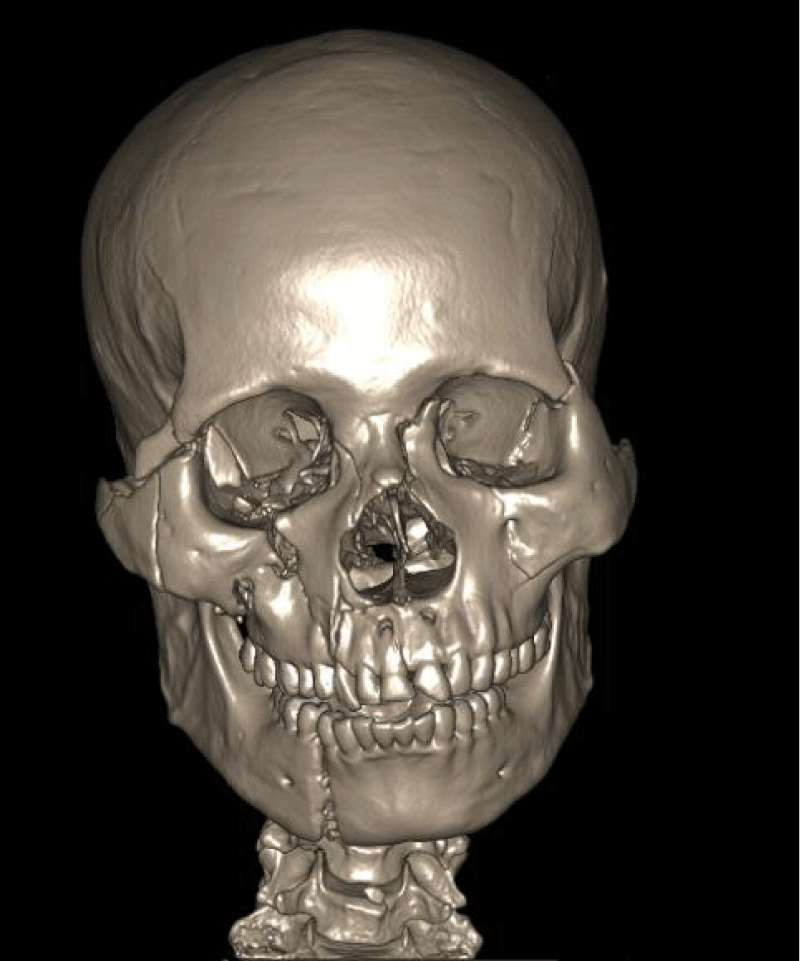
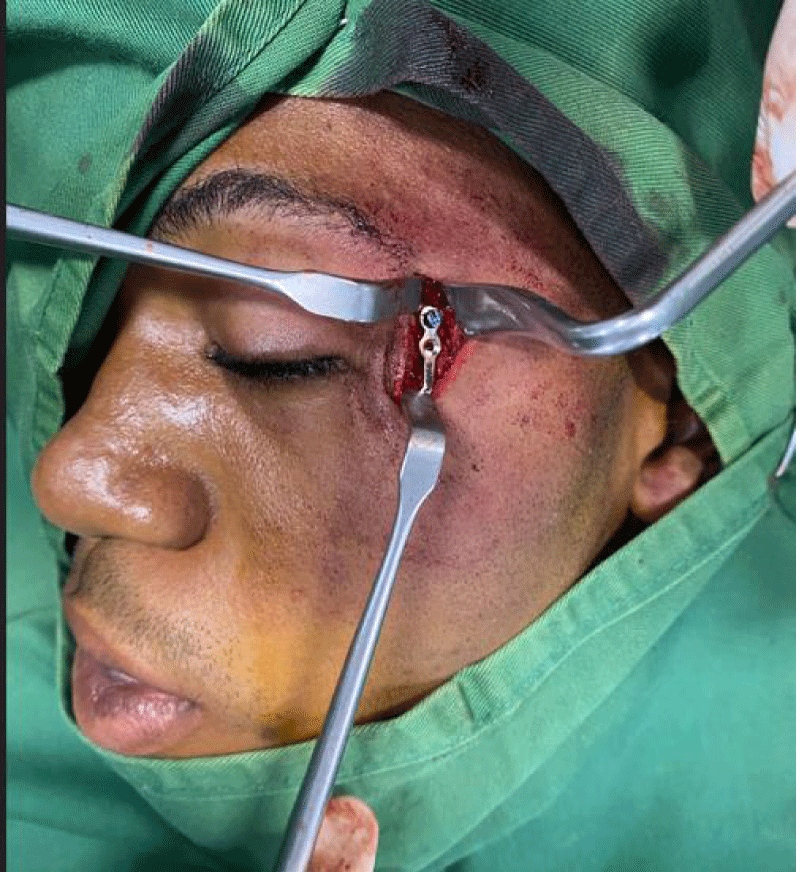
Of the 105 patients who sustained ZMC fractures in this series, the majority [n = 84, 80%] were treated actively by surgical intervention. The commonest indication for surgery was aesthetic consideration [72.6%] followed by derangement of occlusion [63.1%] and restriction of mandibular excursion [20.2%] respectively (Figure 2). Persistent diplopia and enophthalmos were the least common indicators of operative treatments. The most commonly employed surgical modality was a one-point internal fixation with 1.0 mm mini plates and screws across either ZF [n = 33, 39.3%] or ZM [n = 21, 25.0%] suture lines (Figure 3). Only 7 patients [8.3%] had two points of fixation across both ZF and ZM suture lines simultaneously. Surgical access was achieved mostly via lateral eyebrow [n = 41, 51.3%], subcilliary [n = 13, 16.3%] or a combination of both incisions [n = 7, 8.8%]. Other treatment options were Gillies temporal lift [17.9%], use of transosseous wiring with or without front mandibular suspension [7.1%], and reduction via buccal sulcus approach [2.3%]. Regarding other associated maxillofacial injuries (Table 5): mandibular fracture [41.2%] was the commonest followed by Le Fort iii fracture of the maxilla [37.2%] (Images 1-5).
Discussion
The zygoma, being one of the buttresses of the facial skeleton, plays a critical role in the maintenance of normal facial width and prominence of the cheek. These buttresses help give the zygoma an intrinsic strength such that blows to the cheek usually result in fractures of the ZMC at the suture lines, and rarely of the body of the zygomatic bone itself [3]. The observed incidence in age is similar to previous reports where the majority of the patients were in the third decade of life [1,3,5-8,16]. The third decade marked the active phase whereby individuals are more likely to indulge in injury-prone adventures such as reckless driving, violence, and the use of the automobile for commercial purposes. The observed male preponderance is also in agreement with the global trend in the literature. Also, in consonant with the studies cited, RTC was the commonest aetiology of ZMC in this study [3,7,8,16].
The pattern of fracture in this study showed that ZMC was involved in the majority of the fractures [82.9%]. Isolated fractures of the arch were quite uncommon in this series probably due to the fact that most road traffic crashes result in frontal impacts to the face, hence the zygoma is likely to be fractured at the suture lines. Zygomatic arch fractures are more likely to be caused by lateral impact which is more often associated with assault, sport, or missile injuries.
Several signs and symptoms are associated with ZMC fractures and most authors reported Circumorbital and subconjunctival ecchymosis as the most frequently encountered symptoms [2,3,8-10]. Although our findings were in agreement with this assertion, the cases of circumorbital and subconjuctival ecchymosis encountered were mostly usually self-limiting. Flattening of the cheek observed in 72.4% of our patients was the next most common symptom. This is usually seen in ZMC fractures that are most often displaced inwards to a greater extent. Diplopia observed in 30.5% of our patients is comparatively higher than figures from previous studies by Obuekwe, et al. [3] 9.7% and Al-Qurainy, et al. [17] 19.8%. Nevertheless, the presence or absence of diplopia depends largely on the inflammatory process around the extraoccular muscles and most patients seen during the acute inflammatory period, as in our series, may present with diplopia. Limitation of mandibular movement occurred in 65.7% of our patients and this is usually caused by impaction of the fractured zygomatic complex on the coronoid process of the mandible [1,10].
There are divergent opinions in the literature regarding the radiographic examination of fractures of the zygomatic complex. A survey of British oral and maxillofacial surgeons [11] revealed that the majority of surgeons [93.3%] rely on two or more radiographic views for diagnostic purposes. Similarly, Obuekwe, et al. [3] reported that 73.1% of the cases in their study required two or more radiographs for the diagnosis of ZMC fractures. On the contrary, a single 300 occipitomental radiograph was found to be sufficient for 58 [55.2%] of our patients who had plain radiographs for ZMC fracture evaluation. Our observation is in agreement with Pogrel, et al. [18] who concluded that a single 300 occipitomental radiograph (augmented with CT scans when indicated) can identify all midface fractures requiring treatment. The advent of computerized tomography scan [CT scan] has simplified the diagnosis of ZMC fractures and laid to rest the debate about the number of views of plain radiographs required to make an accurate diagnosis. However, only 47 patients [44.8%] in our series were able to afford the cost of a CT scan.
Banks and Brown [10] summarized the indications for treatment of ZMC as follows: to restore the normal contour of the face both for cosmetic reasons and to establish skeletal protection for the globe of the eye, to correct diplopia, and to remove any interference with the range of movement of the mandible. In agreement with other authors, aesthetic consideration was the commonest indicator of surgical treatment amongst our patients [3,8,17]. Malocclusion, Impairment of mandibular excursion, and persistent diplopia were other indicators of surgery that have also been reported in the literature [2,8,9,17-19].
Historically, treatment of ZMC fractures was done mostly via Gillies temporal lift, upper buccal sulcus approach, transosseous wiring, or front mandibular suspension [1-3,8,11,12,19,20]. However, the advent of ostheosynthesis has significantly reduced the use of these traditional methods. Our surgical protocol is similar to recent reports where ZMC fractures were treated with miniplate osteosynthesis. The majority of our subjects [58.1%] had open reduction and internal fixation with 1.0mm miniplates at either ZF, ZM, or both. The availability of plating technology has popularized the use of miniplates in middle and low-income countries [22-24]. Tadj and Kimble [24], and several other authors have affirmed that bone plating was the most effective fixation method in the treatment of ZMC [13,14,15,22-24]. While the use of mini plates for the fixation of ZMC fractures is not debatable in the literature, the debate has however shifted to the relative merit of the number of fixation points employed.
Due to the contiguous anatomic relations of the zygoma with other bones of the facial skeleton, associated maxillofacial Fractures occur quite commonly with ZMC fractures. Fracture of the mandible [41.2%] was found to be the commonest in this study. Our observation was similar to figures reported by Obuekwe [3] Ellis, et al. [21] and Nam [25] These studies showed that mandibular fractures were most often associated with zygomatic complex fractures compared to the other bones of the facial skeleton.
Conclusion
Although ZMC fracture has been grossly underreported in the literature, it remains one of the commonest fractures of the facial skeleton and can be life-threatening when associated with concomitant injuries to the brain and other facial bones. It is therefore imperative to continue to educate the populace about associated morbidity and the importance of preventive measures such as restraints and the use of protective headgear/use of seatbelts while commuting in motorized transport. The advent of mini plate ostheosynthesis has revolutionized the management of ZMC fractures as the majority of the patients were treated with this modality. However, it would be inappropriate not to mention the time-honored technique of closed reduction by Gillies approach, which we employed in the management of some of our subjects with minimally displaced fractures.
- Rowe NL, Williams JL. Fractures of the zygomatic complex and orbit. In: Williams JL Rowe and Williams maxillofacial injuries, vol I, 2nd edn, Churchill Livingstone, Edinburgh. 1994;475–590.
- Yamsani B, Gaddipati R, Vura N, Ramisetti S, Yamsani R. Zygomaticomaxillary Complex Fractures: A Review of 101 Cases. J Maxillofac Oral Surg. 2016 Dec;15(4):417-424. doi: 10.1007/s12663-015-0851-9. Epub 2015 Nov 19. PMID: 27833333; PMCID: PMC5083683.
- Obuekwe O, Owotade F, Osaiyuwu O. Etiology and pattern of zygomatic complex fractures: a retrospective study. J Natl Med Assoc. 2005 Jul;97(7):992-6. PMID: 16080669; PMCID: PMC2569317.
- Hollier LH, Thornton J, Pazmino P, Stal S. The management of orbitozygomatic fractures. Plast Reconstr Surg. 2003 Jun;111(7):2386-92, quiz 2393. doi: 10.1097/01.PRS.0000061010.42215.23. PMID: 12794486.
- Oginni FO, Oladejo T, Alake DP, Oguntoba JO, Adebayo OF. Facial Bone Fractures in Ile-Ife, Nigeria: An Update on Pattern of Presentation and Care. J Maxillofac Oral Surg. 2016 Jun;15(2):184-90. doi: 10.1007/s12663-015-0826-x. Epub 2015 Aug 26. PMID: 27298542; PMCID: PMC4871832.
- Adeyemo WL, Ladeinde AL, Ogunlewe MO, James O. Trends and characteristics of oral and maxillofacial injuries in Nigeria: a review of the literature. Head Face Med. 2005 Oct 4;1:7. doi: 10.1186/1746-160X-1-7. PMID: 16270942; PMCID: PMC1277015.
- Obimakinde OS, Ogundipe KO, Rabiu TB, Okoje VN. Maxillofacial fractures in a budding teaching hospital: a study of pattern of presentation and care. Pan Afr Med J. 2017 Apr 24;26:218. doi: 10.11604/pamj.2017.26.218.11621. PMID: 28690732; PMCID: PMC5491718.
- Adekeye EO. Fractures of the zygomatic complex in Nigerian patients. J Oral Surg. 1980 Aug;38(8):596-9. PMID: 6930461.
- al-Qurainy IA, Stassen LF, Dutton GN, Moos KF, el-Attar A. The characteristics of midfacial fractures and the association with ocular injury: a prospective study. Br J Oral Maxillofac Surg. 1991 Oct;29(5):291-301. doi: 10.1016/0266-4356(91)90114-k. PMID: 1742258.
- Banks P, Brown A. Fractures of the facial skeleton. 1st ed. Oxford: Wright. 2001;40-155.
- McLoughlin P, Gilhooly M, Wood G. The management of zygomatic complex fractures--results of a survey. Br J Oral Maxillofac Surg. 1994 Oct;32(5):284-8. doi: 10.1016/0266-4356(94)90047-7. PMID: 7528055.
- Mahmood S, Keith DJ, Lello GE. Current practice of British oral and maxillofacial surgeons: advice regarding length of time to refrain from contact sports after treatment of zygomatic fractures. Br J Oral Maxillofac Surg. 2002 Dec;40(6):488-90. doi: 10.1016/s0266-4356(02)00226-7. PMID: 12464206.
- Ji SY, Kim SS, Kim MH, Yang WS. Surgical Methods of Zygomaticomaxillary Complex Fracture. Arch Craniofac Surg. 2016 Dec;17(4):206-210. doi: 10.7181/acfs.2016.17.4.206. Epub 2016 Dec 23. PMID: 28913285; PMCID: PMC5556838.
- Starch-Jensen T, Linnebjerg LB, Jensen JD. Treatment of Zygomatic Complex Fractures with Surgical or Nonsurgical Intervention: A Retrospective Study. Open Dent J. 2018 May 21;12:377-387. doi: 10.2174/1874210601812010377. PMID: 30202484; PMCID: PMC6129990.
- Gandi LN, Kattimani VS, Gupta AV, Chakravarthi VS, Meka SS. Prospective blind comparative clinical study of two point fixation of zygomatic complex fracture using wire and mini plates. Head Face Med. 2012 Mar 6;8:7. doi: 10.1186/1746-160X-8-7. PMID: 22390884; PMCID: PMC3342088.
- Fasola AO, Lawoyin JO, Obiechina AE, Arotiba JT. Inner city maxillofacial fractures due to road traffic accidents. Dent Traumatol. 2003 Feb;19(1):2-5. doi: 10.1034/j.1600-9657.2003.00073.x. PMID: 12656847.
- al-Qurainy IA, Stassen LF, Dutton GN, Moos KF, el-Attar A. Diplopia following midfacial fractures. Br J Oral Maxillofac Surg. 1991 Oct;29(5):302-7. doi: 10.1016/0266-4356(91)90115-l. PMID: 1742259.
- Pogrel MA, Podlesh SW, Goldman KE. Efficacy of a single occipitomental radiograph to screen for midfacial fractures. J Oral Maxillofac Surg. 2000 Jan;58(1):24-6. doi: 10.1016/s0278-2391(00)80009-9. PMID: 10632161.
- Ogden GR. The Gillies method for fractured zygomas: an analysis of 105 cases. J Oral Maxillofac Surg. 1991 Jan;49(1):23-5; discussion 26. doi: 10.1016/0278-2391(91)90261-j. PMID: 1985179.
- Kang DH, Jung DW, Kim YH, Kim TG, Lee J, Chung KJ. Kirschner Wire Fixation for the Treatment of Comminuted Zygomatic Fractures. Arch Craniofac Surg. 2015 Dec;16(3):119-124. doi: 10.7181/acfs.2015.16.3.119. Epub 2015 Dec 9. PMID: 28913236; PMCID: PMC5556780.
- Ellis E 3rd, Kittidumkerng W. Analysis of treatment for isolated zygomaticomaxillary complex fractures. J Oral Maxillofac Surg. 1996 Apr;54(4):386-400; discussion 400-1. doi: 10.1016/s0278-2391(96)90107-x. PMID: 8600255.
- Farber SJ, Nguyen DC, Skolnick GB, Woo AS, Patel KB. Current management of zygomaticomaxillary complex fractures: A multidisciplinary survey and literature review. Craniomaxillofac Trauma Reconstr. 2016;9(4):313-22. [http://dx.doi.org/10.1055/s-0036-1592093] [PMID: 27833710].
- Balakrishnan K, Ebenezer V, Dakir A, Kumar S, Prakash D. Management of tripod fractures (zygomaticomaxillary complex) 1 point and 2 point fixations: A 5-year review. J Pharm Bioallied Sci. 2015;7(1):S242–S247. doi: [10.4103/0975-7406.155937: 10.4103/0975-7406.155937].
- Tadj A, Kimble FW. Fractured zygomas. ANZ J Surg. 2003 Jan-Feb;73(1-2):49-54. doi: 10.1046/j.1445-2197.2003.02595.x. PMID: 12534741.
- Nam IW. [Clinical studies on treatment of fractures of the zygomatic bone]. Taehan Chikkwa Uisa Hyophoe Chi. 1990 Jun;28(6):563-70. Korean. PMID: 2130135.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
