Journal of Dental Problems and Solutions
Challenges Faced by Pediatric Dentists in the Dental Management of Children with Autism Spectrum Disorder: A Review Article
1Department for Preventive and Pediatric Dentistry, Faculty of Dental Medicine, University Ss.Cyril & Methodius, Skopje, North Macedonia
2Policlinic Cair, Health Center-Skopje, North Macedonia
Author and article information
Cite this as
Ambarkova V, et al. Challenges Faced by Pediatric Dentists in the Dental Management of Children with Autism Spectrum Disorder: A Review Article. J Dent Probl Solut. 2026; 13(1): 1-6. Available from: 10.17352/2394-8418.000134
Copyright License
© 2026 Ambarkova V, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Autism Spectrum Disorder (ASD) is a neurodevelopmental condition characterized by deficits in social communication and interaction, as well as restricted and repetitive patterns of behavior. According to the World Health Organization, the global prevalence of autism has increased in recent years. These characteristics significantly affect the provision of dental care, and dentists frequently encounter substantial behavioral and clinical challenges when treating children with ASD.
This narrative review aims to summarize the current literature regarding the major challenges faced by dental professionals and to discuss evidence-based strategies for improving dental management in children with ASD.
Children with ASD frequently present with behavioral dysregulation, communication difficulties, sensory hypersensitivity, and comorbid systemic conditions that complicate dental treatment. This review summarizes the etiology, neurobiological background, behavioral characteristics, oral manifestations, and evidence-based dental management strategies for children with ASD. Emphasis is placed on individualized care, behavioral guidance techniques, structured educational models, sensory-adapted dental environments, and preventive-focused treatment planning.
Autism Spectrum Disorder (ASD) is a neurodevelopmental condition characterized by impairments in social communication, restricted and repetitive behaviors, and sensory processing abnormalities. Autism spectrum disorder is diagnosed according to the criteria outlined in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) [1], which emphasize impairments in communication, social interaction, and sensory processing. According to the World Health Organization, the global prevalence of autism has increased in recent years [2]. The global prevalence of ASD has increased considerably in recent decades. These characteristics pose significant challenges in pediatric dental practice.
Autism spectrum disorder is a global public health concern with increasing prevalence worldwide. According to the World Health Organization, approximately 1 in 127 individuals worldwide were estimated to have autism in 2021, although prevalence varies considerably between regions due to differences in diagnostic practices, awareness, and surveillance systems [3,4].
Recent epidemiological studies also indicate that the global prevalence of ASD among children is approximately 0.77%, with notable regional variations reported across Europe, Asia, the Americas, and Africa.
Children with ASD often experience significant barriers in accessing dental care and are more likely to present with unmet dental needs [5,6]. Difficulties in maintaining oral hygiene, sensory sensitivities, and behavioral challenges further contribute to an increased risk of oral diseases [7].
The term autism originates from the Greek word “autos”, meaning “self.” Autism was first described by Hans Asperger in 1938 and later systematically characterized by Leo Kanner in 1943 as a condition marked by profound social withdrawal and insistence on sameness [8,9].
Providing dental treatment to this population requires individualized approaches and additional professional competencies [10].
Recent epidemiological estimates suggest that approximately 1 in 54 children are diagnosed with ASD, with a male-to-female ratio of approximately 4:1 [11]. The increasing prevalence underscores the importance of preparing dental professionals to manage this growing patient population [12].
Methodology
A narrative review of the literature was conducted to identify relevant studies addressing autism spectrum disorder and dental management of affected children. Electronic databases, including PubMed, Scopus, and Google Scholar, were searched for articles published between 2000 and 2024. The search strategy included combinations of the following keywords: “autism spectrum disorder,” “ASD,” “pediatric dentistry,” “oral health,” “dental treatment,” “behavior management,” and “general anesthesia.”
Articles written in English and focusing on the etiology, neurobiology, oral health status, and dental management of children with autism spectrum disorder were considered for inclusion. Review articles, clinical studies, and case reports relevant to the topic were included, while studies not related to dental care or autism spectrum disorder, non-English publications, and duplicate records were excluded. The selected articles were screened based on their relevance to the objectives of this review.
Etiology and neurobiological background
ASD is considered a multifactorial condition involving complex interactions between genetic and environmental factors. Chromosomal abnormalities, including duplication of chromosome 16p13.11-p12.3, have been reported in affected individuals [13]. Genetic predisposition plays a major role in ASD. Twin and family studies estimate heritability between 60%–90%. Key genetic mechanisms include: single-gene mutations (e.g., SHANK3, MECP2, FMR1), copy number variations (CNVs), de novo mutations, and polygenic risk involving multiple susceptibility loci [14].
ASD is frequently associated with genetic syndromes such as Fragile X syndrome, Rett syndrome, and Tuberous Sclerosis Complex. These findings suggest that disruptions in synaptic development and neuronal connectivity are central mechanisms [15].
Environmental risk factors proposed in the literature include advanced parental age, prenatal exposure to environmental toxins, perinatal hypoxia, and certain viral infections [2].
Neuroimaging studies demonstrate structural and functional brain differences in individuals with ASD, including altered amygdala and hippocampal volumes and reduced Purkinje cells in the cerebellum [16]. These neurobiological differences are associated with sensory processing abnormalities that directly influence dental care tolerance.
Behavioral characteristics relevant to dental care
Core behavioral features affecting dental treatment include impaired social interaction, communication deficits, echolalia, cognitive rigidity [16], resistance to routine changes, and hypersensitivity to sensory stimuli [1].
Sensory overload in a dental environment—bright lights, high-frequency sounds, strong smells, and tactile stimuli—may trigger distress responses or behavioral outbursts [17].
Comorbid conditions frequently associated with ASD include epilepsy, attention-deficit/hyperactivity disorder (ADHD), anxiety disorders, sleep disturbances, and intellectual disability [15].
Oral manifestations in children with ASD
Oral findings are generally nonspecific but clinically relevant. Reported manifestations are bruxism (20%–25%) [18], self-injurious behaviors (lip biting, gingival picking), traumatic oral lesions, dental erosion associated with gastroesophageal reflux, and xerostomia related to psychotropic medications [19].
Children with ASD often take medications such as methylphenidate, fluoxetine, sertraline, risperidone, olanzapine, carbamazepine, and valproate, which may reduce salivary flow and increase caries risk [18].
The literature presents inconsistent findings regarding caries prevalence. Some studies report similar or lower caries rates compared with neurotypical peers [18], while systematic reviews indicate increased periodontal disease and higher treatment needs [20,21] (Table 1).
Challenges in pediatric dental practice
Communication barriers
Limited verbal communication and reduced comprehension complicate conventional behavioral guidance techniques such as tell–show–do [18].
Sensory hypersensitivity
Sensory processing abnormalities represent a major clinical challenge. A randomized controlled pilot study demonstrated that sensory-adapted dental environments significantly reduced physiological stress indicators and improved cooperation [22].
Behavioral dysregulation
Children with ASD may exhibit crying, aggression, refusal of treatment, or self-injury during dental procedures [18].
Barriers to dental access
Children with ASD are more likely to experience barriers to dental care and unmet treatment needs [23] (Table 2).
Evidence-based behavioral and educational approaches
Applied Behavior Analysis (ABA)
Applied Behavior Analysis (ABA), pioneered by Ivar Lovaas, focuses on reinforcement, prompting, and behavioral shaping techniques [24].
Structured teaching models
The TEACCH (Treatment and Education of Autistic and Related Communication Handicapped Children) program, developed by Eric Schopler, emphasizes structured learning and visual supports. A TEACCH-based approach has been shown to improve compliance during dental examinations [25].
Sensory-adapted dental environment
Environmental modifications such as dim lighting, reduced noise, weighted blankets, and minimized staff presence significantly improve cooperation and reduce anxiety [22,26].
Visual pedagogy and social stories
Visual schedules, PECS, and video modeling enhance predictability and reduce stress [27].
Advanced management: Sedation and general anesthesia
When behavioral approaches are insufficient, conscious sedation [28-30] or general anesthesia may be necessary to complete comprehensive dental treatment [16]. General anesthesia (GA) is often an important tool when treating individuals with autism spectrum disorder (ASD), especially in medical and dental settings. GA is commonly indicated when the patient cannot tolerate treatment due to severe anxiety or sensory overload, there is a lack of cooperation despite behavioral management, extensive dental or surgical treatment is required, previous attempts under local anesthesia or conscious sedation failed, and there are safety concerns for the patient or medical staff. The use of sedation and general anesthesia may be indicated in children with Autism Spectrum Disorder who exhibit severe anxiety, behavioral dysregulation, or an inability to cooperate during dental procedures. The decision to use pharmacological behavior management should be based on established clinical guidelines such as those provided by the American Academy of Pediatric Dentistry and the American Society of Anesthesiologists. These guidelines emphasize careful patient selection, thorough medical evaluation, and detailed treatment planning before sedation or general anesthesia.
Important clinical considerations include obtaining informed consent from parents or legal guardians, adherence to recommended pre-operative fasting guidelines, and continuous intra-operative monitoring of vital parameters such as oxygen saturation, heart rate, blood pressure, and respiratory function. In addition, appropriate post-operative monitoring and recovery protocols should be followed to ensure patient safety and minimize potential complications. The implementation of these measures contributes to safer and more effective dental care for children with ASD who require advanced behavior management techniques [31].
Current evidence suggests that general anesthesia is generally safe for individuals with ASD, similar to the general population, when proper preoperative assessment is performed, it is administered by experienced anesthesiologists, and appropriate monitoring protocols are followed [32-34]. In pediatric dentistry, general anesthesia is frequently used for full-mouth rehabilitation in autistic children with severe caries or MIH. Multidisciplinary coordination is recommended when possible.
Preventive and restorative considerations
Preventive care is essential and includes 5% sodium fluoride varnish (22,600 ppm fluoride), pit and fissure sealants, and parental oral hygiene education [27,35]
For extensive caries or poor cooperation, stainless steel crowns are often preferred. Rubber dam placement and removable appliances may not be tolerated by some children with ASD [18].
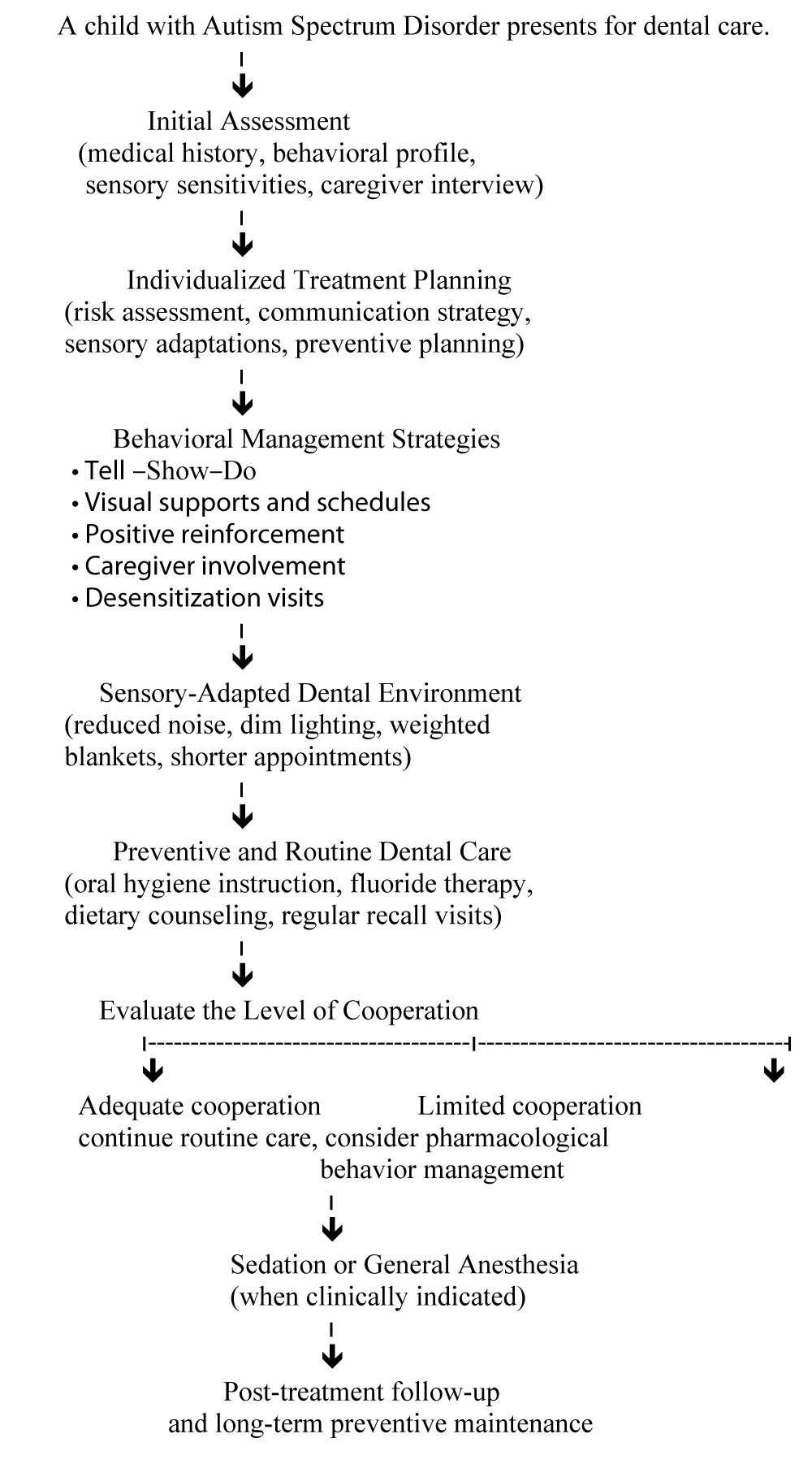
The recommended clinical approach for dental management of children with ASD is illustrated in Figure 1, highlighting the importance of individualized assessment, behavioral guidance techniques, sensory-adaptation strategies, and preventive-focused care.
Clinical pathway for dental management of children with Autism Spectrum Disorder, illustrating the steps from initial assessment and individualized treatment planning to behavioral management strategies, preventive care, and the use of sedation or general anesthesia when indicated (Figure 1).
Conclusion
Children with ASD present complex clinical challenges in pediatric dentistry due to communication deficits, sensory hypersensitivity, and behavioral rigidity. However, structured behavioral interventions, sensory-adapted environments, preventive-focused care, and individualized treatment planning significantly improve outcomes. Ongoing professional education in special care dentistry is essential to address the growing prevalence of ASD and to ensure equitable access to quality oral healthcare.
- American Psychiatric Association. Diagnostic and statistical manual of mental disorders: DSM-5. 5th ed. Washington (DC): American Psychiatric Publishing; 2013. Available from: https://psychiatryonline.org/doi/book/10.1176/appi.books.9780890425596
- World Health Organization. Autism spectrum disorders [Internet]. Geneva: World Health Organization; 2023. Available from: https://applications.emro.who.int/docs/EMRPUB_leaflet_2019_mnh_215_en.pdf
- Institute for Health Metrics and Evaluation. 2021 Global Burden of Disease (GBD) [online database]. Seattle: Institute for Health Metrics and Evaluation; 2024. Available from: https://vizhub.healthdata.org/gbd-results/
- Issac A, Halemani K, Shetty A, Thimmappa L, Vijay VR, Koni K, Mishra P, Kapoor V, et al. The global prevalence of autism spectrum disorder in children: a systematic review and meta-analysis. Osong Public Health Res Perspect. 2025;16(1):3-27. Available from: https://doi.org/10.24171/j.phrp.2024.0286
- Lai B, Milano M, Roberts MW, Hooper SR. Unmet dental needs and barriers to dental care among children with autism spectrum disorders. J Autism Dev Disord. 2012;42(7):1294-303. Available from: https://doi.org/10.1007/s10803-011-1362-2
- McKinney CM, Nelson T, Scott JM, Heaton LJ, Vaughn MG, Lewis CW. Predictors of unmet dental need in children with autism spectrum disorder: results from a national sample. Acad Pediatr. 2014;14(6):624-31. Available from: https://doi.org/10.1016/j.acap.2014.06.023
- Ferrazzano GF, Salerno C, Bravaccio C, Ingenito A, Sangianantoni G, Cantile T. Autism spectrum disorders and oral health status: review of the literature. Eur J Paediatr Dent. 2020;21(1):9-12. Available from: https://doi.org/10.23804/ejpd.2020.21.01.02
- Hamidi A, Persaud NA, Ganti L, Keeler L. Leo Kanner: The physician and pioneer of autism. Cureus. 2024;16(11):e73859. Available from: https://doi.org/10.7759/cureus.73859
- Ostrowski J, Religioni U, Gellert B, Sytnik-Czetwertyński J, Pinkas J. Autism spectrum disorders: etiology, epidemiology, and challenges for public health. Med Sci Monit. 2024;30:e944161. Available from: https://doi.org/10.12659/msm.944161
- George SS, Elenjickal MG, Naik S, Thomas NG, Vellappally S, Varghese N, Mathew A, Narayan V, Varughese RP, Anil S, et al. Oral health status and dental treatment needs in children with autism spectrum disorder. Heliyon. 2024;10(18):e37728. Available from: https://doi.org/10.1016/j.heliyon.2024.e37728
- GBD Epilepsy Collaborators. Global, regional, and national burden of epilepsy, 1990-2021: a systematic analysis for the Global Burden of Disease Study 2021. Lancet Public Health. 2025;10(3):e203-e227. Available from: https://doi.org/10.1016/s2468-2667(24)00302-5
- Weil TN, Inglehart MR. Dental education and dentists' attitudes and behavior concerning patients with autism. J Dent Educ. 2010;74(12):1294-307. Available from: https://pubmed.ncbi.nlm.nih.gov/21123497/
- Pop-Jordanova N, Zorcec T, Sukarova-Angelovska E. Duplication of chromosome 16p13.11-p12.3 with different expressions in the same family. Balkan J Med Genet. 2021;24(1):89-94. Available from: https://doi.org/10.2478/bjmg-2021-0010
- Orefice LL, Zimmerman AL, Chirila AM, Sleboda SJ, Head JP, Ginty DD. Peripheral mechanosensory neuron dysfunction underlies tactile and behavioral deficits in mouse models of ASDs. Cell. 2016;166(2):299-313. Available from: https://doi.org/10.1016/j.cell.2016.05.033
- Trajkovski V. Autism and pervasive developmental disorders. Faculty of Philosophy, Institute of Special Education; 2011. Skopje.
- Cahalan S, Mitroff SR, Subiaul F, Rosenblau G. Using the cognitive rigidity-flexibility dimension to deepen our understanding of the autism spectrum. Personal Neurosci. 2025;8:e3. Available from: https://doi.org/10.1017/pen.2025.10002
- Baizer JS. Neuroanatomy of autism: what is the role of the cerebellum? Cereb Cortex. 2024;34(13):94-103. Available from: https://doi.org/10.1093/cercor/bhae050
- Delli K, Reichart PA, Bornstein MM, Livas C. Management of children with autism spectrum disorder in the dental setting: concerns, behavioural approaches and recommendations. Med Oral Patol Oral Cir Bucal. 2013;18(6):e862-8. Available from: https://doi.org/10.4317/medoral.19084
- Loo CY, Graham RM, Hughes CV. The caries experience and behavior of dental patients with autism spectrum disorder. J Am Dent Assoc. 2008;139(11):1518-24. Available from: https://doi.org/10.14219/jada.archive.2008.0078
- Ferrazzano GF, Salerno C, Bravaccio C, Ingenito A, Sangianantoni G, Cantile T. Autism spectrum disorders and oral health status: review of the literature. Eur J Paediatr Dent. 2020;21(1):9-12. Available from: https://doi.org/10.23804/ejpd.2020.21.01.02
- Corridore D, Zumbo G, Corvino I, Guaragna M, Bossù M, Polimeni A, Vozza I. Prevalence of oral disease and treatment types proposed to children affected by autistic spectrum disorder in pediatric dentistry: a systematic review. Clin Ter. 2020;171(3):e275-e282. Available from: https://doi.org/10.7417/ct.2020.2226
- Cermak SA, Stein Duker LI, Williams ME, Dawson ME, Lane CJ, Polido JC. Sensory-adapted dental environments to enhance oral care for children with autism spectrum disorders: a randomized controlled pilot study. J Autism Dev Disord. 2015;45(9):2876-88. Available from: https://doi.org/10.1007/s10803-015-2450-5
- Du RY, Yiu CKY, King NM. Oral health behaviours of preschool children with autism spectrum disorders and their barriers to dental care. J Autism Dev Disord. 2019;49(2):453-459. Available from: https://doi.org/10.1007/s10803-018-3708-5
- Gitimoghaddam M, Chichkine N, McArthur L, Sangha SS, Symington V. Applied behavior analysis in children and youth with autism spectrum disorders: a scoping review. Perspect Behav Sci. 2022;45(3):521-557. Available from: https://doi.org/10.1007/s40614-022-00338-x
- Orellana LM, Martínez-Sanchis S, Silvestre FJ. Training adults and children with an autism spectrum disorder to be compliant with a clinical dental assessment using a TEACCH-based approach. J Autism Dev Disord. 2014;44(4):776-85. Available from: https://doi.org/10.1007/s10803-013-1930-8
- Fallea A, Zuccarello R, Roccella M, Quatrosi G, Donadio S, Vetri L, Calì F, et al. Sensory-adapted dental environment for the treatment of patients with autism spectrum disorder. Children (Basel). 2022;9(3):393. Available from: https://doi.org/10.3390/children9030393
- Doichinova L, Gateva N, Hristov K. Oral hygiene education of special needs children. Part 1: Children with autism spectrum disorder. Biotechnol Biotechnol Equip. 2019;33(1):748-755. Available from: https://doi.org/10.1080/13102818.2019.1615846?urlappend=%3Futm_source%3Dresearchgate.net%26utm_medium%3Darticle
- Vallogini G, Festa P, Matarazzo G, Gentile T, Garret-Bernardin A, Zanette G, Galeotti A, et al. Conscious sedation in dentistry for the management of pediatric patients with autism: a narrative review of the literature. Children (Basel). 2022;9(4):460. Available from: https://doi.org/10.3390/children9040460
- Gao F, Wu Y. Procedural sedation in pediatric dentistry: a narrative review. Front Med (Lausanne). 2023;10:1186823. Available from: https://doi.org/10.3389/fmed.2023.1186823
- Mroczek M, Orlanska A. Nitrous oxide and oral sedation for managing dental anxiety in children: a systematic review. Cureus. 2026;18(2):e103449. Available from: https://doi.org/10.7759/cureus.103449
- Coté CJ, Wilson S. Guidelines for monitoring and management of pediatric patients before, during, and after sedation for diagnostic and therapeutic procedures. Pediatr Dent. 2019;41(4):E26–E52. Available from: https://doi.org/10.1542/peds.2019-1000
- Jaber MA. Dental caries experience, oral health status, and treatment needs of dental patients with autism. J Appl Oral Sci. 2011;19(3):212-7. Available from: https://doi.org/10.1590/s1678-77572011000300006
- Rada RE. Treatment needs and adverse events related to dental treatment under general anesthesia for individuals with autism. Intellect Dev Disabil. 2013;51(4):246-52. Available from: https://doi.org/10.1352/1934-9556-51.4.246
- Lai CC, Wu CC. Caries pattern and dental treatment features of children with autism spectrum disorder under general anesthesia. Medicine (Baltimore). 2025;104(12):e41867. Available from: https://doi.org/10.1097/md.0000000000041867
- Zerman N, Zotti F, Chirumbolo S, Zangani A, Mauro G, Zoccante L. Insights on dental care management and prevention in children with autism spectrum disorder (ASD): what is new? Front Oral Health. 2022;3:998831. Available from: https://doi.org/10.3389/froh.2022.998831
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
