Journal of Dental Problems and Solutions
Enhancing Marginal Integrity and Interproximal Papilla Stability in Posterior Teeth Using Deep Margin Elevation with Ceramic Inlays/Onlays: A Clinical Report
Department of Fixed Prosthodontics, Faculty of Dentistry, Monastir University, Tunisia
Author and article information
Cite this as
Daouahi N, et al. Enhancing Marginal Integrity and Interproximal Papilla Stability in Posterior Teeth Using Deep Margin Elevation with Ceramic Inlays/Onlays: A Clinical Report. J Dent Probl Solut. 2026; 13(1): 7-12. Available from: 10.17352/2394-8418.000135
Copyright License
© 2026 Daouahi N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Background: Defective posterior restorations with inadequate proximal morphology are commonly associated with plaque accumulation and localised periodontal inflammation. Restorative strategies that re-establish both marginal integrity and interproximal architecture are essential for maintaining periodontal health. Adhesively bonded ceramic inlays/onlays, associated with Deep margin elevation, provide a conservative option with favourable mechanical and biological outcomes.
Case presentation: A 32-year-old female patient presented with discomfort in the left posterior region, recurrent food impaction, and bleeding during oral hygiene procedures. Clinical examination revealed extensive defective restorations on teeth 36 and 37, characterised by loss of marginal ridges, deep proximal–occlusal lesions, and altered interproximal contours, contributing to plaque retention and papillary inflammation.
Management: Indirect lithium disilicate inlay/onlay restorations were planned. Deep margin elevation was performed to relocate subgingival margins coronally, facilitating adequate isolation and adhesive procedures. Restorations were designed to restore proximal contact, anatomical contours, and occlusal function, with optimal marginal adaptation.
Outcome: The definitive restorations achieved satisfactory marginal integrity and functional occlusion, with good aesthetic integration. Clinically, symptoms resolved, food impaction was eliminated, and oral hygiene improved. The interproximal papilla showed clear stabilisation, with resolution of inflammation.
Conclusion: Lithium disilicate inlays/onlays, combined with deep margin elevation and strict adhesive protocols, represent a predictable and biologically sound approach for restoring marginal integrity and interproximal tissue stability in posterior teeth with extensive structural loss.
Restoration of posterior teeth remains challenging, particularly in the interproximal region, which is highly susceptible to iatrogenic damage during operative procedures. The morphology of this area, especially the interproximal contact and embrasure width, plays a critical role in maintaining periodontal health. Evidence indicates that inadequate contact size or contour is significantly associated with increased plaque accumulation, gingival inflammation, and bleeding, as well as the development of localised alveolar bone defects [1].
Full-coverage restorations require extensive tooth reduction, increasing the risk of periodontal disease. In contrast, CAD–CAM inlays and onlays provide a conservative approach, enabling precise margin and proximal control while preserving periodontal architecture [2].
Systematic reviews and clinical series report high survival rates for inlays/onlays (well over 90% at 5 years) and reported that marginal integrity, as a critical factor for periodontal health, is more favorable in inlays/onlays than might be expected with crowns [3].
Clinical data from a prospective randomized study comparing CAD–CAD-CAM inlay onlays to full coverage crowns showed that ceramic onlays had significantly better periodontal outcomes (lower plaque index, bleeding on probing, and probing depth) over 1–2 years of follow-up. This suggests that the more conservative design of onlays, combined with supragingival or properly finished margins, may reduce periodontal inflammation and preserve the health of interdental tissues [4].
However, the long-term periodontal impact of CAD–CAM ceramic inlay/onlay restorations depends critically on multiple technical factors such as restorative material, the quality of marginal adaptation, the type and precision of the CAD–CAM system (scanner, software parameters, milling strategy), and cementation/finishing protocols [5].
Indeed, poor marginal fit, regardless of the restoration type, is widely recognized as a predisposing factor for microleakage, plaque accumulation, and subsequent periodontal irritation. According to these considerations, it is essential to explore to what extent modern CAD–CAM partial coverage restorations can maintain both structural and periodontal integrity over time [6].
This clinical report presents the rehabilitation of mandibular first and second molars using CAD–CAM ceramic partial restorations combined with deep margin elevation, highlighting a biologically driven approach to re-establish marginal integrity and optimise interproximal tissue health.
Clinical presentation
A 32-year-old patient presented to the prosthetic dentistry department with a chief complaint of pain during mastication, which is localized to the left posterior mandibular region. He also reported difficulties in maintaining hygiene in this area, frequent food impaction, recurrent bleeding when brushing, and discomfort.
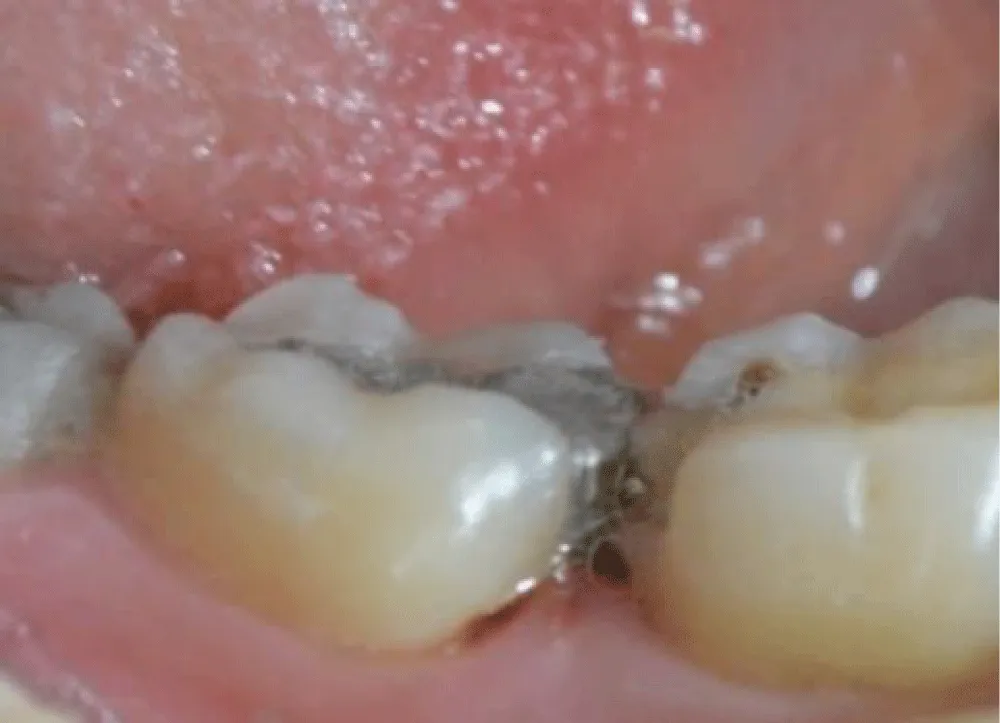
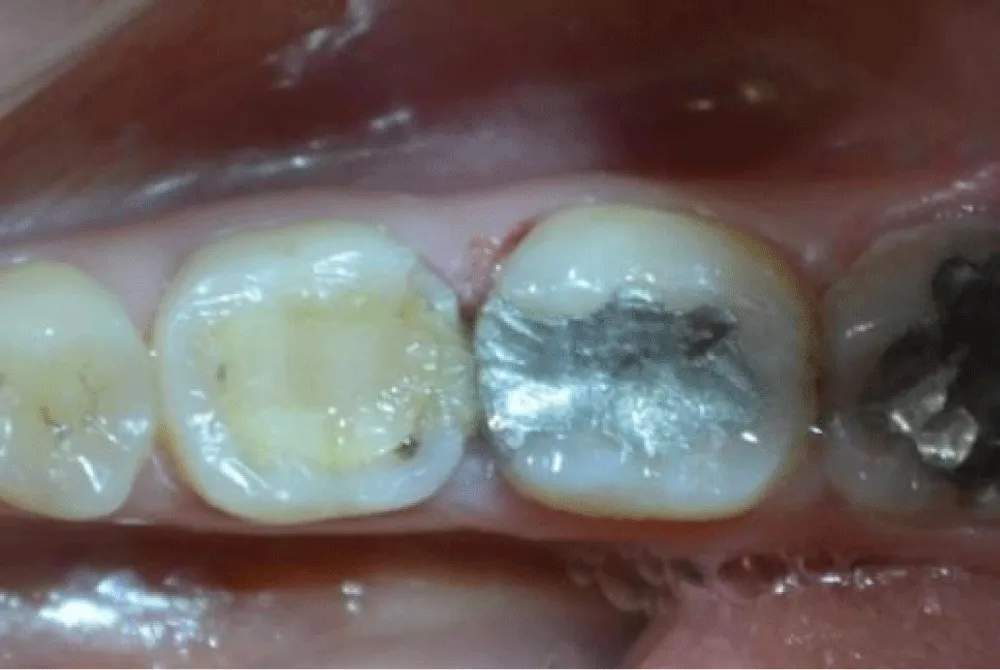
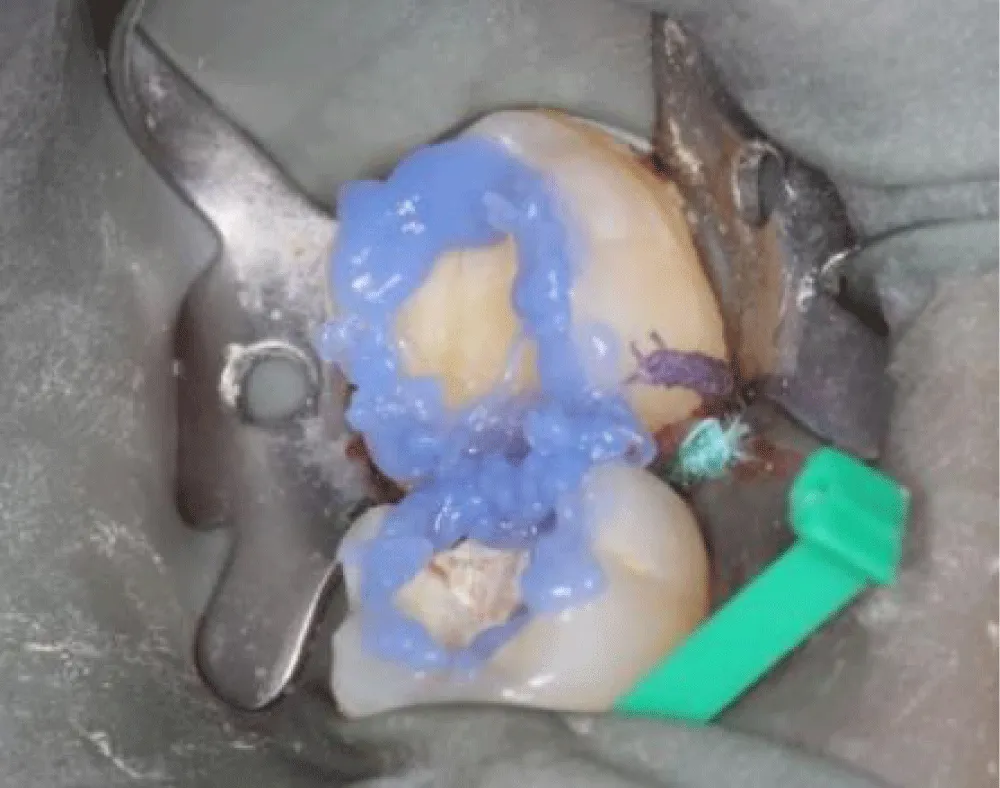
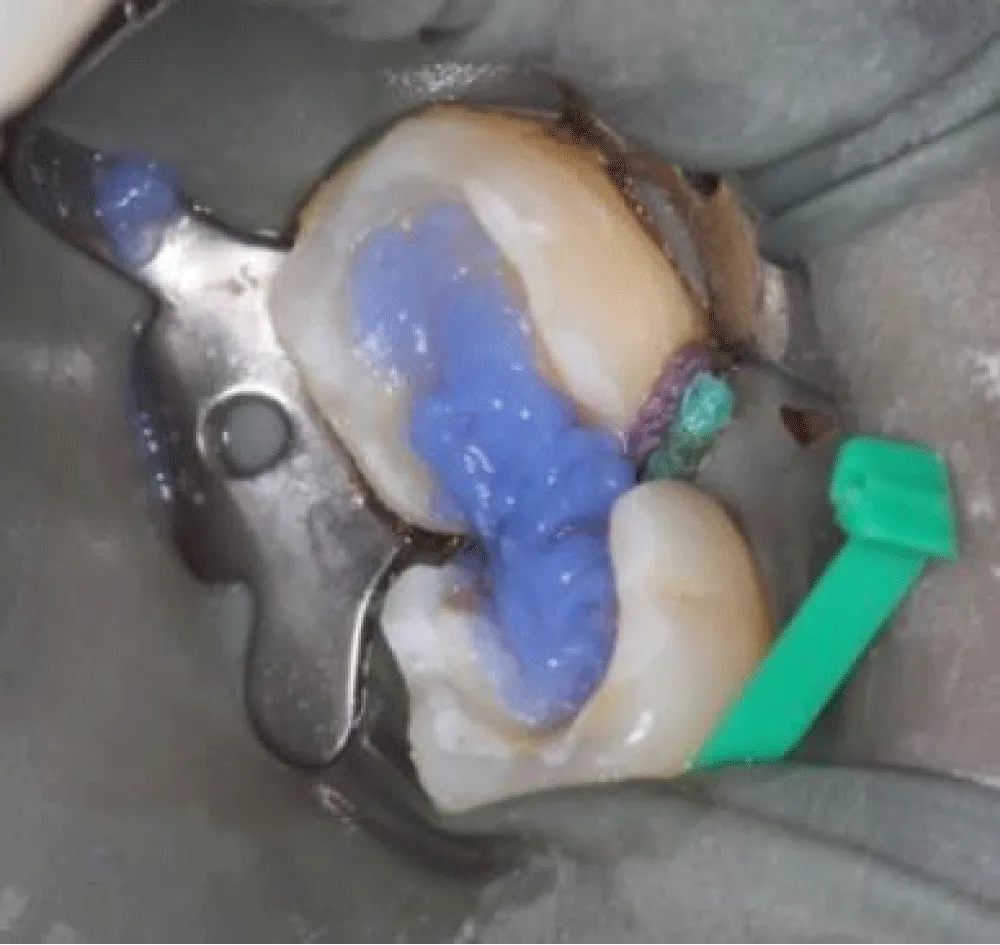
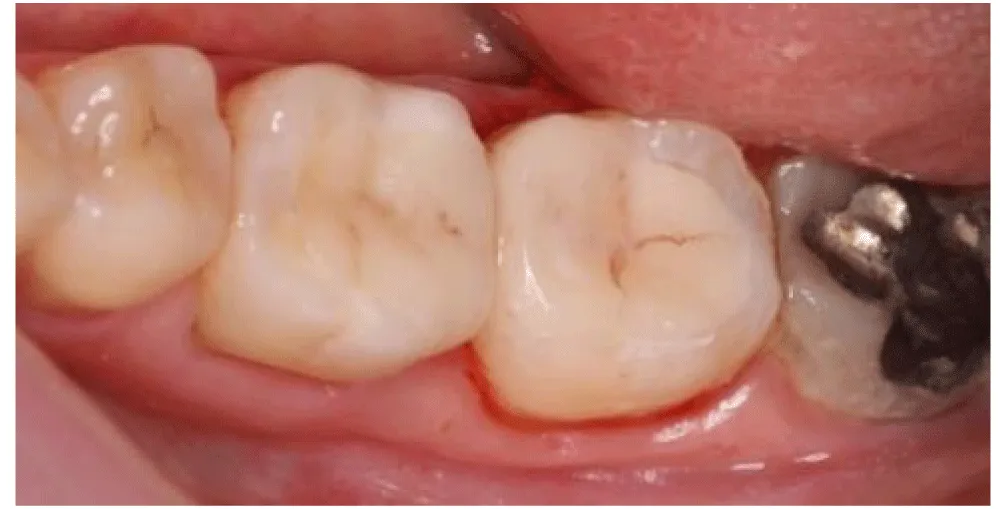
Clinical examination revealed two extensive posterior restorations affecting both tooth 36 and tooth 37, compromising the interproximal contours. Deep proximal-occlusal cavities associated with plaque accumulation in the interproximal space were detected. The probing of the interdental papilla showed localized bleeding confirming inflammatory changes in the adjacent periodontal tissues and compromised interdental architecture (Figure 1,2).
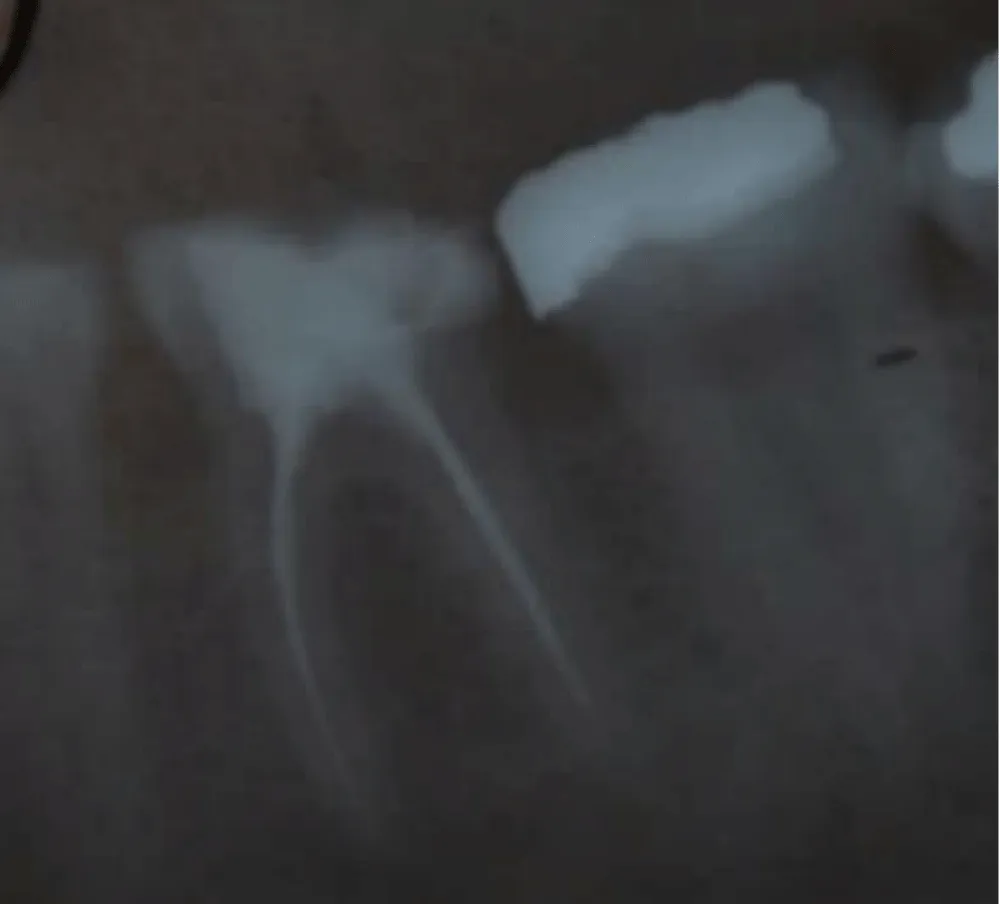
Radiographic evaluation confirmed the extent of structural loss. It demonstrated adequate endodontic treatment on the first molar, but insufficient coronal support (Figure 3). The second molar was vital. It also confirmed the lack of the natural interproximal contour, explaining the chronic irritation and pain which increases during mastication.
These findings indicated the need for indirect ceramic restorations capable of re-establishing correct contour, occlusal stability, and accurate interproximal contact to restore periodontal health.
The treatment plan included:
- Periodontal management, including scaling and debridement of the interproximal area.
- Restoration of the molars with indirect ceramic inlay/onlay (Lithium Disilicate) to re-establish an anatomical contact and correct architecture in the interproximal zone, and improve patient comfort and hygiene accessibility in the interproximal region.
The preparation provides sufficient ceramic thickness and an extensive adhesive surface. The depth of the cavity should be around ≈1.5 mm (minimum) to assure material strength. The finish lines should be a smooth, rounded shoulder (≈0.8–1.0 mm) to provide adequate marginal bulk without creating thin ceramic edges.
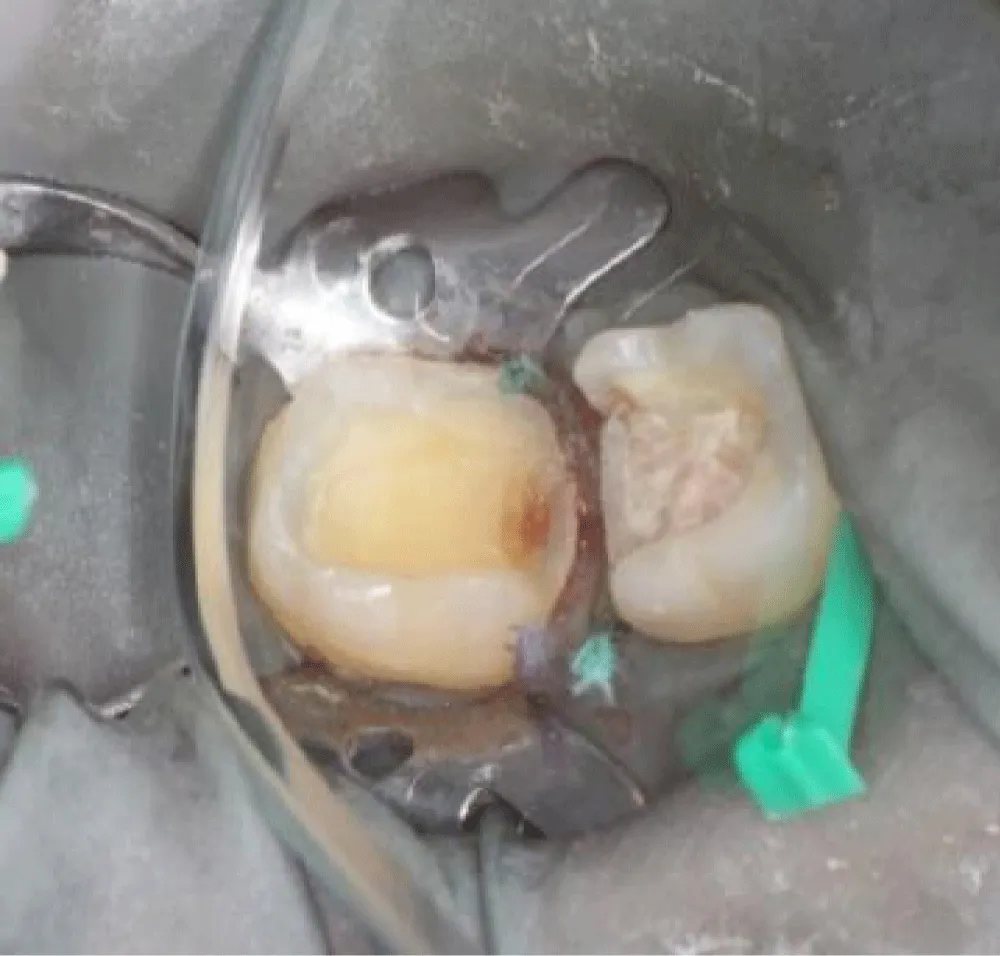
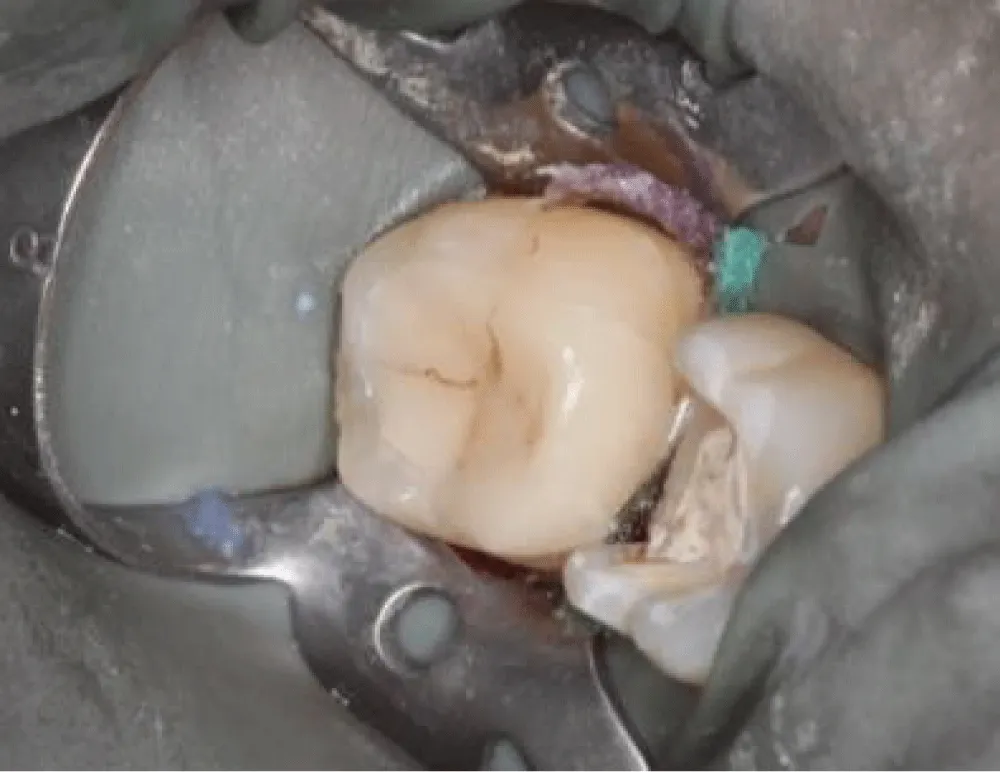
Axial walls in the cavities should be free of undercuts and have a slight divergence (clinical recommendations commonly range from about 6° up to 15° total taper, depending on the system) with rounded internal line angles to reduce stress concentrations. Sufficient tissue thickness on the cusps was maintained (Figure 4).
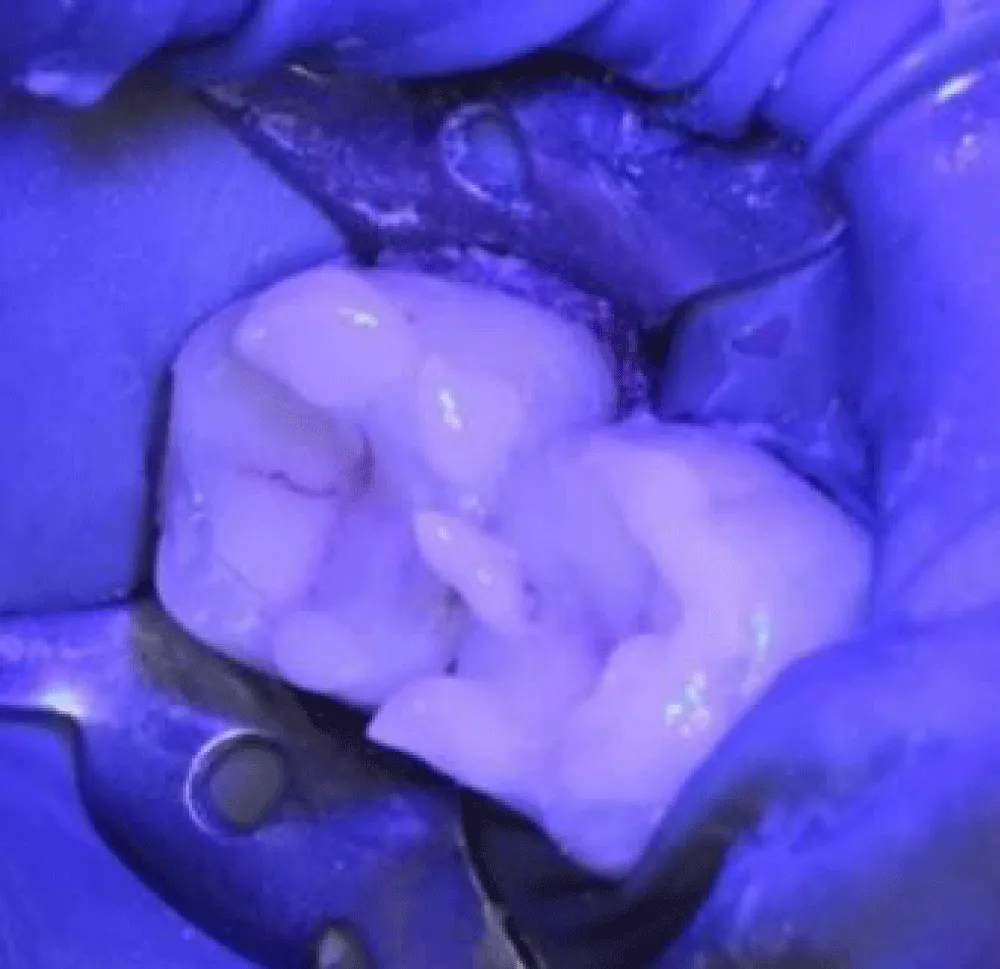
Sufficient enamel was preserved at the margins because bonded margins to enamel give superior and more durable adhesion. Deep Margin elevation was performed in the first molar. During the stage of cementation, Restorations were etched (hydrofluoric acid for ceramics) and silanized. Tooth surfaces were selectively etched, and a universal adhesive was applied. Duale Resin cement was used for bonding under controlled isolation (Figure 5-7). Restorations were finally light-cured from all aspects, and glycerin was applied in the margins to protect the marginal fit (Figure 8). At the 2-week follow-up, the patient reported complete disappearance of pain. No bleeding was observed during hygiene procedures. The interproximal area was restored, and the architecture was established with a continuous adhesive surface and optimal marginal integrity (Figure 9).
Discussion
This clinical investigation evaluated the relationship between the marginal integrity of ceramic inlay–onlay restorations and the stability of the interproximal papilla. Clinically, ensuring optimal marginal adaptation in ceramic inlays and onlays is essential, as excessive marginal gaps can promote microleakage, plaque accumulation, and marginal discoloration. Such conditions may alter the local ecological environment and increase the risk of periodontal complications, ultimately compromising interproximal papilla health and stability [7].
The improved description and structuring of the FDI World Dental Federation criteria, initially introduced in 2007 and updated in 2010, have contributed to standardizing the evaluation of direct and indirect restorations. According to this consensus, key assessment parameters include material fracture, retention, marginal adaptation, proximal contact integrity, anatomical form and contour, as well as occlusal performance and wear behavior [8,9].
Marginal fit and its clinical acceptability have been widely examined in restorative dentistry literature. Numerous in vitro and clinical investigations indicate that marginal gaps of approximately 100 µm or less are generally considered clinically acceptable for ceramic inlays and onlays. Larger discrepancies are associated with increased risks of microleakage, plaque retention, and marginal discoloration, all of which may compromise both restoration longevity and periodontal health [10].
Historically, the anatomical relationship between interproximal restorations and periodontal tissues has also been explored. Matherson and Zander demonstrated (In 1963) that the morphology of the interdental col is primarily influenced by the contour and position of the proximal contact area rather than the underlying bone architecture, emphasizing the importance of precise proximal form in maintaining papillary stability [11,12].
CAD–CAM fabrication protocols and the selected restorative material present a significant influence on the marginal accuracy of indirect ceramic restorations. Scientific evidence indicates that thermomechanical stresses, including artificial aging and thermocycling, may further increase marginal discrepancies after cementation, particularly in materials with lower dimensional stability. Alterations in marginal integrity can modify the local plaque-retentive environment and compromise the seal at the tooth-restoration interface [13].
Goujat.A in systematic review reported that most investigations have reported that the marginal adaptation of CAD-CAM inlays and onlays generally present clinically acceptable limits. However, several factors influence this performance. The restorative material selected for the CAD–CAM workflow plays a decisive role in determining marginal accuracy. Non-retentive preparation designs tend to yield superior adaptation compared with retentive configurations. Many studies also indicate that thermomechanical loading can negatively affect marginal integrity, and the cementation procedure itself often leads to an increase in marginal discrepancies [14].
Comparisons between intraoral and extraoral digital impressions have shown no significant differences in marginal fit for onlay restorations. Conversely, the number of milling axes, camera technology used for image acquisition, and the specific areas assessed for measurement have demonstrated statistically significant effects on both marginal and internal adaptation [15].
In several investigations, the achieved adaptation did not match the spacer settings predefined in CAD software, suggesting limitations in reproducing digital parameters in the final restoration [16].
Further clarification is required regarding how preparation design, material type, milling instrument geometry, and material behavior during fabrication influence adaptation [17,18].
Refaey HS reported in 2025 that overlay restorations using advanced zirconia reinforced lithium disilicate CAD CAM glass ceramic demonstrated that preparation design significantly affects both marginal fit and fracture resistance, with shoulder finish designs showing the lowest marginal gaps after thermal aging [19,20].
An in vitro study comparing different CAD CAM inlay materials (ceramic, composite-based, resin-modified ceramics) was conducted by Taha AI, et al. They found that marginal gap values varied according to the material, and that thermocycling had a greater negative effect on composite-based and resin-modified ceramics than on glass ceramic inlays [20,21].
The health and presence of the interproximal papilla are primarily determined by a combination of biological and dimensional factors, which interact closely with restorative considerations. The classical “distance” rule established by Tarnow, et al. remains an indice in predicting papilla presence: when the vertical distance from the contact point to the alveolar bone crest is ≤5 mm, the papilla is present in most cases, whereas greater distances are associated with a marked reduction in papilla fill [12]. Consequently, restorative design including the position of the contact point, emergence profile, and the presence of overcontouring or under-contouring, plays a critical role in maintaining or restoring optimal papillary architecture [6,21].
The position and design of restorative margins represent additional key factors influencing periodontal health. While subgingival margins are sometimes required for caries management or to improve retention, they pose challenge for achieving optimal isolation, accurate cementation, and precise finishing. These technical difficulties can promote plaque accumulation and increase the risk of gingival inflammation. Evidence from clinical trials and retrospective studies indicates that, although careful exécution, including appropriate material selection, adhesive protocols, and meticulous finishing, can reduce these risks, subgingival margins may still exert a measurable impact on the periodontium [22].
Techniques such as deep margin elevation (cervical margin relocation) may offer promising strategies to preserve papilla architecture and facilitate restorative procedures. Deep Margin Elevation relocates the cervical margin coronally by building up a composite (or resin-based) foundation, thereby facilitating isolation, adhesive procedures, impression or scanning, cementation, finishing, and polishing of indirect restorations under more favorable conditions [23].
When performed with meticulous technique, DME appears to be a good strategy for restoring deep subgingival cavities or margins while preserving papilla architecture and periodontal health. However, long-term clinical studies remain necessary to validate its safety and efficacy in diverse clinical situations [24-26].
From a biomechanical perspective, deep margin elevation facilitates the relocation of subgingival margins to a more coronal position, thereby enabling optimal isolation and improving the predictability of adhesive procedures [27]. This approach enhances the quality of the resin–dentin interface by promoting more controlled hybrid layer formation and reducing the risk of marginal leakage. Furthermore, ceramic inlays/onlays contribute to favorable stress distribution across the restored tooth structure, particularly when cuspal coverage is achieved, thereby minimizing the risk of fracture [28]. The stability of the interproximal papilla is also influenced by the restoration’s emergence profile and the integrity of proximal contact points, which are critical in maintaining periodontal health and preventing food impaction. Collectively, these biomechanical and interfacial factors support the clinical rationale for combining deep margin elevation with adhesive ceramic restorations.
In summary, the marginal integrity of ceramic inlays and onlays is a key determinant of interproximal papilla stability, but it acts in concert with other critical factors. An integrated restorative approach - ensuring precise marginal adaptation, optimal proximal contacts, and respect for periodontal architecture - offers the most reliable preservation of papillary form in the aesthetic zone [27,28].
Limitations
This report describes a single case, limiting generalizability. The lack of a control group and short follow-up preclude firm conclusions on long-term outcomes. Operator-dependent and anatomical factors may also have influenced results. Further controlled studies with larger samples and longer follow-up are needed to confirm these findings.
Conclusion
Marginal integrity of ceramic inlay–onlay restorations contributes to interproximal papilla stability by influencing contact quality, plaque control, and periodontal health. Careful restorative design, appropriate contact positioning, and a harmonious emergence profile remain essential. In deep cervical margins, deep margin elevation may facilitate adhesive procedures and restorative precision while preserving the periodontal environment. This technique appears to be a promising and clinically viable approach in the presented case; however, further studies are necessary to confirm its long-term effectiveness.
Acknowledgements
The authors would like to thank the clinical and technical staff of the Department of Prosthetic Dentistry for their support.
Ethical approval and consent to participate
Ethical approval was not required for this study as it is a case report. Patient anonymity was strictly maintained, and no identifiable personal data was disclosed. A written consent was obtained from the patient.
Conflict of interest
The author declares that there are no conflicts of interest related to this study.
- Desai J, Vishnoi S, Nadig PP, Raj K, Kasundra D, Bharucha D, et al. Influence of inter-proximal dimensions on inter-dental papilla presence. Bioinformation. 2025 Jan 31;21(1):91-95. Available from: https://doi.org/10.6026/973206300210091
- Irum B, Asif M, Mumtaz B, Aslam N. Effect of dental proximal restorations on periodontal health in patients. J Ayub Med Coll Abbottabad. 2022;34 Suppl 1(4):987-990. Available from: https://doi.org/10.55519/jamc-04-s4-10454
- Vagropoulou GI, Klifopoulou GL, Vlahou SG, Hirayama H, Michalakis K. Complications and survival rates of inlays and onlays vs complete coverage restorations: a systematic review and analysis of studies. J Oral Rehabil. 2018;45(11):903-920. Available from: https://doi.org/10.1111/joor.12695
- Biswal S, Yadav BK, Nagpal A, Shetty OK, Ritwal P, Kapoor S. A comparative evaluation of prosthetic and clinical outcomes influenced by two digitally fabricated extracoronal restorations: an onlay and a full crown: a prospective, cross-arch randomized study. J Indian Prosthodont Soc. 2025;25(2):150-162. Available from: https://doi.org/10.4103/jips.jips_331_24
- Toma FR, Moleriu LC, Porojan L. Micro-CT marginal and internal fit evaluation of CAD/CAM high-performance polymer onlay restorations. Polymers (Basel). 2023;15(7):1715. Available from: https://doi.org/10.3390/polym15071715
- Merrill TC, Mackey T, Luc R, Lung D, Naseem A, Abduo J. Effect of chairside CAD/CAM restoration type on marginal fit accuracy: a comparison of crown, inlay and onlay restorations. Eur J Prosthodont Restor Dent. 2021;29(2):119-127. Available from: https://doi.org/10.1922/ejprd_2121abduo09
- Hickel R, Mesinger S, Opdam N, Loomans B, Frankenberger R, Cadenaro M, et al. Revised FDI criteria for evaluating direct and indirect dental restorations: recommendations for clinical use, interpretation, and reporting. Clin Oral Investig. 2023;27(6):2573-2592. Available from: https://doi.org/10.1007/s00784-022-04814-1
- Hickel R, Roulet JF, Bayne S, Heintze SD, Mjör IA, Peters M, et al. Recommendations for conducting controlled clinical studies of dental restorative materials: FDI World Dental Federation study design and criteria for evaluation. J Adhes Dent. 2007;9(1):121-147. Available from: https://doi.org/10.1007/s00784-022-04814-1
- Hickel R, Peschke A, Tyas M, Mjör I, Bayne S, Peters M, et al. FDI World Dental Federation clinical criteria for the evaluation of direct and indirect restorations: update and clinical examples. J Adhes Dent. 2010;12:259-272. Available from: https://doi.org/10.3290/j.jad.a19262
- Zarrati S, Mahboub F. Marginal adaptation of indirect composite, glass-ceramic inlays and direct composite: an in vitro evaluation. J Dent (Tehran). 2010 Spring;7(2):77-83. Available from: https://pubmed.ncbi.nlm.nih.gov/21998779/
- Matherson DG. Evaluation of osseous surgery in monkeys. Int J Periodontics Restorative Dent. 1988;8(5):8-39. Available from: https://pubmed.ncbi.nlm.nih.gov/3248922/
- Tarnow DP, Magner AW, Fletcher P. The effect of the distance from the contact point to the crest of bone on the presence or absence of the interproximal dental papilla. J Periodontol. 1992;63(12):995-996. Available from: https://doi.org/10.1902/jop.1992.63.12.995
- Taha AI, Hafez ME. An in vitro study measuring marginal gaps of inlay restorations fabricated from different CAD-CAM materials after thermocycling. BMC Oral Health. 2023;23(1):974. Available from: https://doi.org/10.1186/s12903-023-03687-4
- Goujat A, Abouelleil H, Colon P, Jeannin C, Pradelle N, Seux D, et al. Marginal and internal fit of CAD-CAM inlay/onlay restorations: a systematic review of in vitro studies. J Prosthet Dent. 2019;121(4):590-597. Available from: https://doi.org/10.1016/j.prosdent.2018.06.006
- Fukazawa S, Odaira C, Kondo H. Investigation of accuracy and reproducibility of abutment position by intraoral scanners. J Prosthodont Res. 2017;61(4):450-459. Available from: https://doi.org/10.1016/j.jpor.2017.01.005
- de Paula Silveira AC, Chaves SB, Hilgert LA, Ribeiro AP. Marginal and internal fit of CAD-CAM-fabricated composite resin and ceramic crowns scanned by two intraoral cameras. J Prosthet Dent. 2017;117(3):386-392. Available from: https://doi.org/10.1016/j.prosdent.2016.07.017
- Abdel-Azim T, Rogers K, Elathamna E, Zandinejad A, Metz M, Morton D. Comparison of the marginal fit of lithium disilicate crowns fabricated with CAD/CAM technology using conventional impressions and two intraoral digital scanners. J Prosthet Dent. 2015;114:554-559. Available from: https://doi.org/10.1016/j.prosdent.2015.04.001
- Seo D, Yi Y, Roh B. The effect of preparation designs on the marginal and internal gaps in Cerec3 partial ceramic crowns. J Dent. 2009;37:374-382. Available from: https://doi.org/10.1016/j.jdent.2009.01.008
- Refaey HS, Abdelkader SH, Aly YM. Fracture resistance and marginal fit of three different overlay designs using advanced zirconia-reinforced lithium disilicate CAD/CAM material. BMC Oral Health. 2025;25(1):20. Available from: https://doi.org/10.1186/s12903-024-05315-1
- Taha AI, Hafez ME. An in vitro study measuring marginal gaps of inlay restorations fabricated from different CAD-CAM materials after thermocycling. BMC Oral Health. 2023;23(1):974. Available from: https://doi.org/10.1186/s12903-023-03687-4
- Belák Š, Žižka R, Starosta M, Zapletalová J, Šedý J, Štefanatný M. The influence of gingival phenotype on the morphology of the maxillary central papilla. BMC Oral Health. 2021;21(1):43. Available from: https://doi.org/10.1186/s12903-021-01400-x
- Muscholl C, Zamorska N, Schoilew K, Sekundo C, Meller C, Büsch C, et al. Retrospective clinical evaluation of subgingival composite resin restorations with deep-margin elevation. J Adhes Dent. 2022;24:335-344. Available from: https://doi.org/10.3290/j.jad.b3240665
- Amartzi TK, Papalexopoulos D, Ntovas P, Rahiotis C, Blatz MB. Deep margin elevation: a literature review. Dent J (Basel). 2022;10(3):48. Available from: https://doi.org/10.3390/dj10030048
- Felemban MF, Khattak O, Alsharari T, Alzahrani AH, Ganji KK, Iqbal A. Relationship between deep marginal elevation and periodontal parameters: a systematic review. Medicina (Kaunas). 2023;59(11):1948. Available from: https://doi.org/10.3390/medicina59111948
- Vargas-Corral FG, Vargas-Corral AE, Rodríguez-Valverde MA, Bravo M, Rosales-Leal JI. Clinical comparison of the marginal fit of ceramic inlays between digital and conventional impressions. J Adv Prosthodont. 2024;16(1):57-65. Available from: https://doi.org/10.4047/jap.2024.16.1.57
- Krejci I, Lutz F, Reimer M. Marginal adaptation and fit of adhesive ceramic inlays. J Dent. 1993;21(1):39-46. Available from: https://doi.org/10.1016/0300-5712(93)90048-U
- Patel M, Guni A, Nibali L, Garcia-Sanchez R. Interdental papilla reconstruction: a systematic review. Clin Oral Investig. 2024;28(1). Available from: https://doi.org/10.1007/s00784-023-05409-0
- Elmorsy AK, Ibrahim SH, El-Nahass HME, Zohairy AE. 22 months follow-up of deep marginal acquisition with thermacut bur in management of deep subgingival interproximal carious lesions: a case report. BMC Oral Health. 2025;25(1):67. Available from: https://doi.org/10.1186/s12903-024-05326-y
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
