Journal of Dental Problems and Solutions
Evaluation of Calcified Carotid Artery Atheromas Detected By Panoramic Radiograph among Patients with Type II Diabetes Mellitus
Hamdan Bin Mohamed College of Dental Medicine, MBR University of Medical & Health Sciences, UAE
Author and article information
Cite this as
Jaber MA, Shah MS, Abuzayeda M (2015) Evaluation of Calcified Carotid Artery Atheromas Detected By Panoramic Radiograph among Patients with Type II Diabetes Mellitus. J Dent Probl Solut. 2015; 2(3): 48-52. Available from: 10.17352/2394-8418.000018
Copyright License
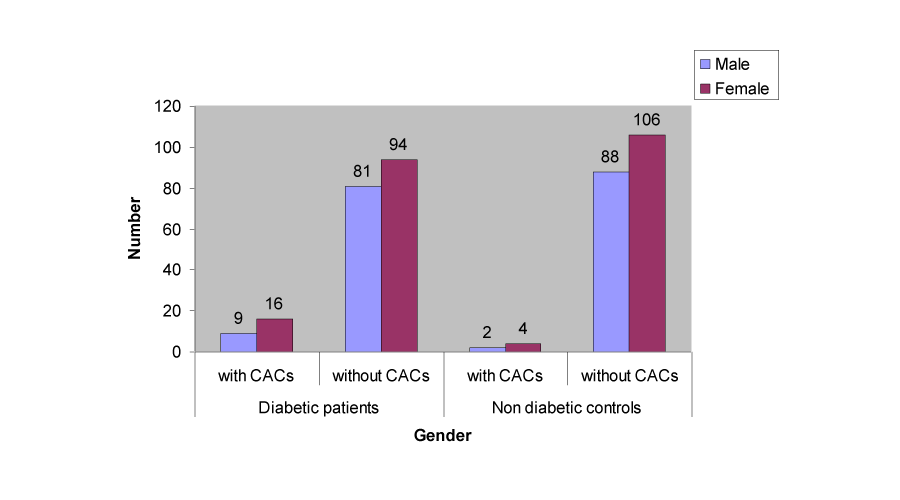
© 2015 Jaber MA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.This study was designed to determine the prevalence of Carotid artery calcifications (CACs) of diabetic patients and compare it with normal non-diabetic individuals. Panoramic radiographs of 200 adult patients with type 2 diabetes (90 male and 110 females) (age range 16-79 years; mean age 40.54 years) and 200 controls (age-match, free of systemic diseases) were examined on panoramic radiographs for any unusual radiopacity adjacent to or just below the intervertebral space between C3 and C4. Statistical analysis was carried out using chi-squared and Fisher exact tests. Carotid artery calcifications (CACs) were higher in diabetic patients compared with normal healthy control and the statistical difference between the two groups was significant (Chi-square test = 10.82, P = 0.001). Twenty-five (16 females, 9 males) diabetic patients showed CACs, Mean age of diabetic patients with calcification was 47.11 years. Further analysis of this group showed that 60% of patients with CACs were smokers, 48% had hypertension and 25% were obese. In conclusion, our study shows that in patients with diabetes mellitus CACs can be detected by panoramic radiography and the patients may benefit from a referral to physicians for further evaluation and necessary management.
Diabetes mellitus is currently the fastest growing debilitating disease in the world. The International Diabetes Federation reported that in the United Arab Emirates (UAE) the prevalence of diabetes mellitus estimated to be ~20% such that one out of five people aged 20 to 79 lives with this disease and this has been attributed to the rapid economic development coupled with ageing populations [1]. Type 2 diabetes mellitus is a disorder of abnormal metabolism of carbohydrates, fats and proteins that arises from a combination of resistance to insulin's action and insufficient secretion of additional insulin to compensate for this resistance. Diabetes mellitus associated with metabolic and vascular components that accelerate the development of atherosclerotic lesions at the bifurcation of the common carotid artery and double or triple the risk of ischemic stroke [2-5]. Type 2 diabetes typically appears after age of 40 years and often is associated with the excessive ingestion of a high-caloric diet and reduced physical activity, the combination of which results in central/abdominal obesity.
Previous studies reported that stroke is the second most frequent cause of death worldwide, which frequently associated with permanent disability [6,7]. It has been reported that patients with diabetes are at 1.5 to three times the risk of stroke compared with the general population [8,9], and the associated mortality and morbidity is greater than in those without this underlying condition [10,11]. This is primarily due to the increased atherogenic risk within extracranial and intracranial arteries, attributable to abnormal plasma lipid profiles, hypertension and hyperglycaemia [11].
Type 2 DM may predispose patients to an ischemic stroke, and the majority of these arise in association with the development of atherosclerotic lesions in the region of the carotid bifurcation [12,13].
Hollander et al. [14], reported that individuals diagnosed with carotid artery plaques might experience an increased risk of stroke and cerebral infarction, compared with subjects who do not have carotid plaques. Denudation of the endothelium over the fibrous plaque may lead to exposure of the sub endothelial layer which may result into thrombus formation and partial or complete occlusion of the blood flow [15].
Several researchers have demonstrated the presence of CACs on dental panoramic radiographs, which might be useful indicator to identify asymptomatic dental patients who may benefit from further examination by medical professionals [16-24]. Despite the number of publications about the presence of CACs on the panoramic radiography among various populations, there has been no detailed information about this condition in diabetic patients in UAE. Hence, we evaluated the presence of carotid artery calcifications (CACs) detected on dental panoramic radiographs among a group of diabetic patients attending dental clinics.
Materials and Methods
A total of 200 diabetic patients (type II) (90 females, 110 males) who visited college of dentistry dental clinics between February 2011 to June 2012 and underwent dental panoramic radiographs for the diagnosis of dental lesions were selected for this study. Age and gender matched healthy control subjects were identified from the hospital record department and included in the study.
The inclusion criteria include: a diagnosis of type 2 diabetes mellitus, panoramic radiograph visualizing the area 2.5 cm posterior and 2.5 cm inferior to the cortical rim of the midpoint of the mandibular angle and patient's consent for the study. And the excluding criteria included; poor quality radiographs and poor or uncontrolled DM as evidenced by a glycosylated hemoglobin A, or HbA1c. According to the generally accepted guidelines in clinical monitoring of diabetic patients, diabetes mellitus is considered to be well controlled if the HbA1c levels are below 7.5%, and moderately controlled if the HbA1c levels vary between 7.5-8.5%. Values from 6.8 to 10% indicate poor control of the disease (25).
All panoramic radiographs were obtained using a standard dental panoramic radiographic system (a Planmeca 2002 EC Proline multitomographic X-ray unit (Planmeca Co., Helsinki, Finland). Exposed panoramic radiographs were processed according to the manufacturer's recommendations. They were obtained with a constant 12mA, 80kV and 18s exposure through 2.5mm Al filtration. Regular Kodak Lanex (Eastman Kodak Co, Rochester, NY) intensifying screens (15x30 cm cassette) and Kodak T Mat G films (Eastman Kodak Co, Rochester, NY). Films were developed in an automatic film processor (Velopex, Extra-X, Medivance Instruments Ltd, London, UK) with standard solutions as recommended by the manufacturer. The total time of processing was 4 minutes at 27°C.
A panoramic radiographs were examined for the presence of unilateral or bilateral, radiopaque masses of the neck at the level of the intervertebral space between C3 and C4.
Patient's records were reviewed for factors related to both diabetes and atherosclerosis. Specifically noted were hypertension as determined by self-report of physician-diagnosed hypertension; current use of an antihypertension medication; or a systolic blood pressure of more than 150 millimeters of mercury or a diastolic blood pressure of more than 90 mm Hg or both and body mass index (BMI). BMI calculated as weight in kilograms divided by the square of the height in meters, with patients categorized as normal (BMI, 18.5–24.9), overweight (BMI, 25–30) or obese (BMI 30); and smoking history. Ethical clearance for the study was obtained from the Ethical Committee for Research of the College of Dentistry, Ajman University, UAE.
Statistical procedures were carried out using SPSS program version 11. Chi-squared or Fissure exact test were used to compare between the two groups and the results were considered significant when p < 0.05.
Results
200 diabetic patients (90 male and 110 females) age range 16-79 years; mean age (40.54 ± 3.7 years) and 200 non-diabetic healthy subjects have completed the study. The mean age of diabetic patients was not significantly different than the mean (± SD) age of 40.52 ± 2.8 years (range 17–78) for the control group.
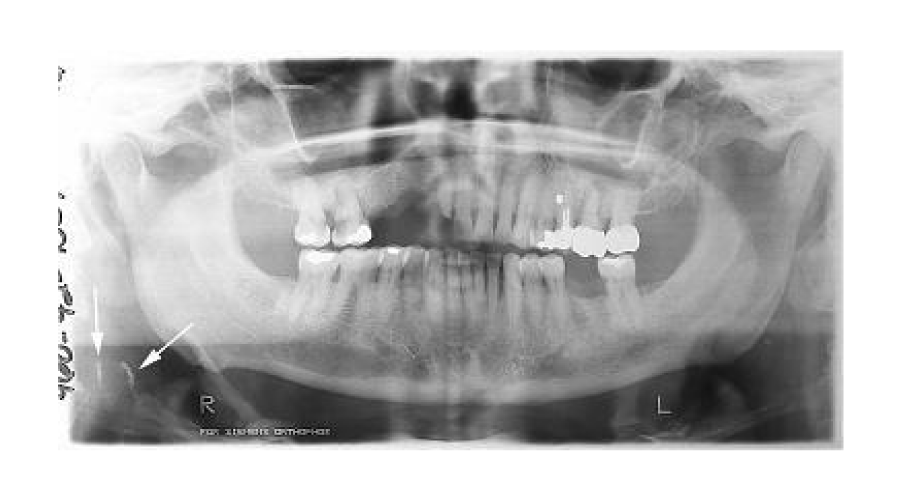
Thirty one (7.75%) CACs were detected in the panoramic radiograph of the study subjects (Figures 1,2). CACs was higher in diabetic patients 12.5% (25/200) compared with normal healthy control 3.0% (6/200) and the statistical difference between the two groups was significant (Chi-square = 10.82, P = 0.001).
Table 1 presents general comparisons between the two groups. The twenty-five diabetic patients (16 females and 9 males) had a mean (± standard deviation) age of 47.11 ± 4.7 years (range 26–65 years). Further analysis of this group showed that 60% of patients with CACs were smokers, 48% had hypertension and 25% were obese.
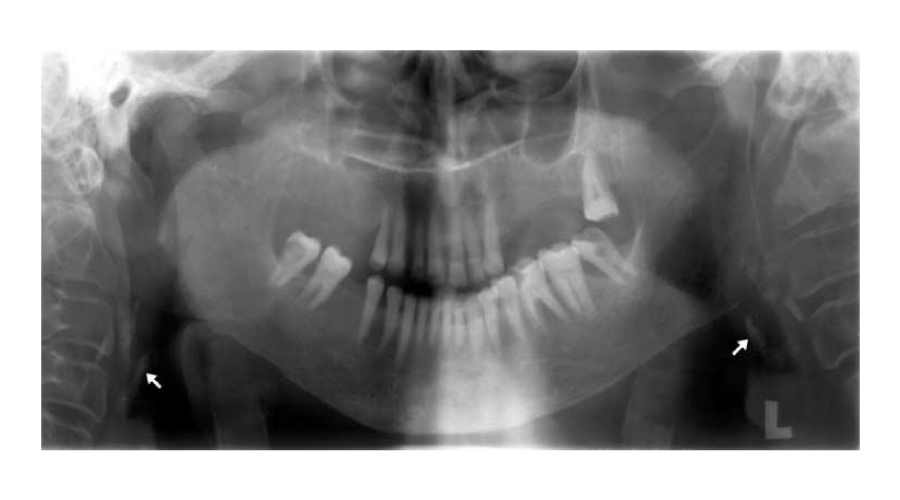
The evaluation of the CACs occurrence revealed that twenty-five (25/31 80.6%) of the CACs were unilateral (Figure 2) and six were bilateral (Figure 3) in distribution.
Discussion
Ischemic cerebrovascular disease is a leading cause of mortality in UAE and other countries. Therefore, factors associated with this disease are important to identify. In this study carotid artery calcification was higher in diabetic patients compared with non-diabetic healthy individuals, a similar findings were reported by Friedlander and Maeder [21], who reported that 20.4% of the panoramic radiographs of diabetics patients had atheromas whereas those of the control groups only 4.0% demonstrated atheromas, furthermore, previously published studies demonstrated that patients with type 2 diabetes treated with insulin had a high prevalence of CAC visible on panoramic radiographs [22,26]. And those diabetic patients controlling their type 2 diabetes with diet alone or with a hypoglycemic agent had slightly lower prevalence of CAC on their panoramic radiographs than did those treated by diet and insulin [22].
Atherosclerosis, a progressive inflammatory disease, may lead to stroke, coronary artery disease, or peripheral artery disease and is a frequent cause of morbidity in patients with diabetes [27]. It tends to accumulate within the bifurcation of the common, external and internal carotid arteries, and it produces symptoms as plaque forms on the irregular surface and embolises to the brain [16]. Atherosclerosis of the cervical carotid artery bifurcation is a major cause of stroke and transient ischemic attack; it provides a site at which progression of atherosclerosis can be monitored reproducibly and noninvasively [28,29]. Various risk factors were reported to contribute to its initiation and progression such as; diabetes mellitus, arterial hypertension and inadequate diet and eating habits. Other new risk factors such as periodontitis, chronic renal disease and menopause have been suggested as being favorable to its development [21]. On panoramic radiographs, these calcifications appear as heterogeneous radiopacities near the hyoid bone at the level of the C3 and C4 intervertebral space [16,21].
Atheromas composed of lipids and fibrous tissue, which are deposited on the arterial walls and become calcified, making it feasible to identify them in panoramic radiographic screening, a widely used diagnostic tool in routine dental practice [30-38]. However, The diagnosis of atheromas in panoramic radiographs may not be so simple, as various other entities may be present in the same region, therefore the dental practitioners ought to be familiar with the differential diagnosis of the images of carotid artery atheromas in panoramic radiography which includes number of anatomic structures in the cervical and adjacent regions, such as: the hyoid bone, styloid process, triticeal cartilages, thyroid cartilage, epiglottis, calcifications in the stylohyoid and stylomandibular ligaments, tonsilloliths, phlebolites, calcified lymphnodes and anterior tubercle of the atlas vertebra [39-41].
Previous reports indicated that CACs might not always be noticed on the panoramic radiograph because not all atherosclerotic lesions are calcified, thus an expert's opinion is needed for accurate radiographic interpretation [16,40]. The use of panoramic radiography to detect carotid artery calcifications could also have led to potential error. Panoramic radiography has been found in multiple studies to be helpful in the diagnosis of CAC but can lead to miscategorization of the degree of calcifications, especially if not performed and evaluated properly or if the plaques causing calcifications are not adequately calcified.
To our knowledge, the present study is the first report describing the prevalence of CACs on panoramic radiographs of patients with type 2 diabetes in UAE. We determined a higher prevalence of calcification in the area of the carotid artery of patients with diabetes than those of matched control patients (12.5% vs. 3.0%). Some studies reported that CAC were also seen in non-diabetic control group and also among general dental outpatients [37,38].
Panoramic radiography is widely used as a diagnostic tool for all health disciplines concerned with the oral and maxillofacial region. However, it has some limitations when used in screening for carotid calcification [42], thus other diagnostic modalities such as ultrasound, MRI and angiography might be required to confirm presence and extent of vascular calcification [43-46]. Randoux et al. [47], reported that Multiple Detector CT angiography is a robust technique for assessing calcification and can potentially depict and allow quantification of load in the carotid arteries in a manner similar to coronary artery scoring, while being highly accurate for measuring luminal stenosis.
In conclusion, our study shows that in patients with diabetes mellitus CACs can be detected by panoramic radiography and the patients may benefit from a referral to physicians for further evaluation and necessary management.
- Guariguata L, Whiting D, Hambleton I, Beagley J, Linnenkamp U, et al. (2014) Global estimates of diabetes prevalence for 2013 and projections for 2035. Diabetes Res Clin Pract 103: 137–149 .
- Yki-Järvinen H (2000) Management of type 2 diabetes mellitus and cardiovascular risk: lessons from intervention trials. Drugs 60: 975–983.
- Mudríková T, Szabová E, Tkac I (2000) Carotid intima-media thickness in relation to macrovascular disease in patients with type 2 diabetes mellitus. Wien Klin Wochenschr 112: 887–891 .
- Kanters SD, Banga JD, Stolk RP, Algra A (1999) Incidence and determinants of mortality and cardiovascular events in diabetes mellitus: a meta-analysis. Vascular Med 4: 67–75.
- Mogensen CE (1999) Drug treatment for hypertensive patients in special situations: diabetes and hypertension. Clin Exp Hypertens 21: 895–906 .
- Murray C, Lopez A (1997) Mortality by cause for eight regions of the world: Global Burden of Disease Study, Lancet 349:1269-1276.
- Sacco R, Benjamin E, Broderick J (1997) American Heart Association Prevention Conference. IV. Prevention and Rehabilitation of Stroke, Risk factors. Stroke 28: 1507-1517 .
- Kissela B, Khoury J, Kleindorfer D (2005) Epidemiology of ischemic stroke in patients with diabetes: the greater Cincinnati/Northern Kentucky Stroke Study. Diabetes Care 28: 355-359 .
- Folsom A, Rasmussen M, Chambless L (199) Prospective associations of fasting insulin, body fat distribution, and diabetes with risk of ischemic stroke. The Atherosclerosis Risk in Communities (ARIC) Study Investigators. Diabetes Care 22: 1077-1083 .
- Mankovsky B, Metzger B, Molitch M, Biller J (1996) Cerebrovascular disorders in patients with diabetes mellitus. J Diabetes Complications 10: 228-242.
- Boden-Albala B, Sacco RL, Lee HS, Grahame-Clarke C, Rundek T, et al. (2008) Metabolic syndrome and ischemic stroke risk: Northern Manhattan Study. Stroke 39: 30-35.
- Chait A, Bierman EL (1994) Pathogenesis of macrovascular disease in diabetes. In: Kahn CR, Weir GC, eds. Joslin's diabetes mellitus. 13th ed. Philadelphia: Lea & Febiger 648–664 .
- Nesto R, Libby P (2001) Diabetes mellitus and the cardiovascular system. In: Braunwald E, Zipes D, Libby P, ed. Heart disease: A textbook of cardiovascular medicine. 6th ed. Philadelphia: Saunders; 2133–2146 .
- Hollander M, Bots ML, Del Sol AI, Koudstaal PJ, Witteman JC, et al. (2002) Carotid plaques increase the risk of stroke and subtypes of cerebral infarction in asymptomatic elderly: the Rotterdam study. Circulation 105: 2872–2877 .
- Boudi F (2006) Causes and treatment of atherosclerosis. Published online in eMedicine Specialties.
- Almog D, Horev T, Illig K, Gren R, Carter L (2002) Correlating carotid artery stenosis detected by panoramic radiography with clinically relevant carotid artery stenosis determined by duplex ultrasound. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 94: 768–773 .
- London G, Marty C, Marchais SJ, et al. (2004) Arterial calcifications and bone histomorphometry in end stage renal disease. J Am Soc Nephrol 15: 1943–1951 .
- Hubar J (1999) Carotid artery calcification in the Black population: a retrospective study on panoramic radiographs. Dentomaxillofac Radiol 28: 348–350 .
- Ohba T, Takata Y, Ansai T, et al. (2003) Evaluation of calcified carotid artery atheromas detected by panoramic radiograph among 80-year-olds. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 96: 647–650.
- Friedlander A, Altman L (2001) Carotid artery atheromas in postmenopausal women. Their prevalence on panoramic radiographs and their relationship to atherogenic risk factors. J Am Dent Assoc 132:1130–1136 .
- Guimarães Henriques JC1, Kreich EM, Helena Baldani M, Luciano M, Cezar de Melo Castilho J (2011) Panoramic Radiography in the Diagnosis of Carotid Artery Atheromas and the Associated Risk Factors. Open Dent J 5: 79-83 .
- Friedlander A, Garrett N, Norman D (2002) The prevalence of calcified carotid artery atheromas on the panoramic radiographs of patients with type 2 diabetes mellitus. J Am Dent Assoc 133: 1516–1523.
- Friedlander A, Friedlander I, Yueh R, Littner M (1999) The prevalence of carotid atheromas seen on panoramic radiographs of patients with obstructive sleep apnea and their relation to risk factors for atherosclerosis. J Oral Maxillofac Surg 57: 516–521.
- Friedlander A, Freymiller E (2003) Detection of radiation-accelerated atherosclerosis of the carotid artery by panoramic radiography. A new opportunity for dentists. J Am Dent Assoc 134:1361–1365.
- Suomen Diabetesliitto (1995) Nuoruustyypin diabeteksen hoitosuositus. 1: 13 .
- Friedlander A, Maeder L (2000) The prevalence of calcified carotid artery atheromas on the panoramic radiographs of patients with type 2 diabetes mellitus. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 89:420–424 .
- Almog D, Tsimidis K, Moss M, Gottlieb R, Carter L (2000) Evaluation of a training program for detection of carotid artery calcifications on panoramic radiographs. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 90: 111–117 .
- Kitamura A, Iso H, Imano H, Ohira T, Okada T, et al. (2004) Carotid intima-media thickness and plaque characteristics as a risk factor for stroke in Japanese elderly men. Stroke 35: 2788–2794 .
- Hollander M, Hak AE, Koudstaal PJ, Bots ML, Grobbee DE, et al. (2003) Comparison between measures of atherosclerosis and risk of stroke: the Rotterdam Study. Stroke 34: 2367–2372 .
- Ardakani F, Ardakani M, Mohammadi Z, Sheikhha M (2007) Evaluating calcified carotid artery atheromas in panoramic radiographs of patients with type 2 diabetes mellitus. Oral Radiol 23: 6–9 .
- Friedlander A, Cohen S (2007) Panoramic radiographic atheromas portend adverse vascular events. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 103: 830–835.
- Griniatsos J, Damaskos S, Tsekouras N, Klonaris C, Georgopoulos S (2009) Correlation of calcified carotid plaques detected by panoramic radiograph with risk factors for stroke development. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 108: 600–603.
- Madden RP, Hodges JS, Salmen CW, Rindal DB, Tunio J, et al. (2007) Utility of panoramic radiographs in detecting cervical calcified carotid atheroma. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 103: 543–548.
- Manzi F, Guedes F, Duarte R (2005) Identificação de pacientes com risco de derrame na clínica odontológica por meio de radiografias panorâmicas. Rev Bras Odontol 62: 238–240 .
- Carter LC (2000) Discrimination between calcified triticeous cartilage and calcified carotid atheroma on panoramic radiography. Oral Surg Oral Med Oral Pathol Oral Radio Endod 90: 108–110.
- Ahmad M, Madden R, Perez L (2005) Triticeous cartilage: prevalence on panoramic radiographs and diagnostic criteria. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 99: 225–230.
- Ravon N, Hollender L, McDonald V, Persson G (2003) Signs of carotid calcification from dental panoramic radiographs are in agreement with Doppler sonography results. J Clin Periodontol 30:1084–1090.
- Pornprasertsuk-Damrongsri S, Virayavanich W, Thanakun S, Siriwongpairat P, Amaekchok P, et al. (2009) The prevalence of carotid artery calcifications detected on panoramic radiographs in patients with metabolic syndrome. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 108: 57–62 .
- Carter L, Haller A, Nadarajah V, Calamel A, Aguirre A (1997) Use of panoramic radiography among an ambulatory dental population to detect patients at risk of stroke. J Am Dent Assoc 128: 977–984 .
- Lewis D, Brooks S (1999) Carotid artery calcification in a general dental population: a retrospective study of panoramic radiographs. General Dent 47: 98–103 .
- Kamikawa R, Pereira M, Fernandes A, Meurer M (2006) Study of the localization of radiopacities similar to calcified carotid atheroma by means of panoramic radiography. Oral Surg Oral Med Oral Pathol Oral Radio Endod 101: 374–378 .
- Khosropanah , Shahidi S, Bronoosh P, Rasekhi A (2009) Evaluation of carotid calcification detected using panoramic radiography and carotid Doppler sonography in patients with and without coronary artery disease. Br Dent J 207: 1-4.
- Suarez-Cunqueiro M, Duker J, Liebehenschel N, Schon R, Schmelzeisen R (2002) Calcification of branches of the external carotid artery detected by panoramic radiography: A case report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 94: 636–640 .
- London GM1, Guérin AP, Marchais SJ, Métivier F, Pannier B, et al. (2003) Arterial media calcification in end-stage renal disease: impact on all cause and cardiovascular mortality. Nephrol Dial Transplant 18: 1731–1740 .
- Friedlander AH, Baker JD (1994) Panoramic radiography: an aid detecting patients at risk of cerebrovascular accident. J Am Dent Assoc 125: 1598–1603 .
- Cohen S, Friedlander A, Jolly D, Date L (2002) Carotid calcification on panoramic radiographs: An important marker for vascular risk. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 94: 510–514 .
- Randoux B1, Marro B, Koskas F, Duyme M, Sahel M, et al. (2001) Carotid artery stenosis: prospective comparison of CT, three- dimensional gadolinium-enhanced MR, and conventional angiography. Radiol 220: 179–185.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
