Annals of Musculoskeletal Medicine
The 6-minute walk-test in type 2 diabetics predicts to some extent maximal aerobic capacity but not its training-induced improvement
U1046 INSERM, UMR9214 CNRS, Université de Montpellier, Département de Physiologie Clinique, Unité d’Explorations Métaboliques (CERAMM), Service Central de Physiologie Clinique; Hôpital Lapeyronie CHU Montpellier, France
Author and article information
Cite this as
Brun JF, Myzia J, Bui G, Grubka E, Karafiat M, et al. (2020) The 6-minute walk-test in type 2 diabetics predicts to some extent maximal aerobic capacity but not its training-induced improvement. Ann Musculoskelet Med. 2020; 4(1): 3-9. Available from: 10.17352/amm.000020
Copyright License
© 2020 Brun JF, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Objective: Six- minutes’ walk-test (6MWT) is a measure of physical fitness widely studied and validated in chronic pathologies with sedentary lifestyles. It is an aerobic fitness test, correlated with maximum oxygen consumption (VO2max) in some studies, but this correlation is not well established in diabetes. We assessed the extent to which it predicts VO2max and its training-induced changes in type 2 diabetics.
Materials and methods: Twenty-five type 2 diabetics were randomized and divided into two groups: 13 completed a physical training program (eight hospital education sessions continued at home through two weekly 30-45-minute sessions at an intensity corresponding to the first ventilatory threshold VT1) and the remaining 12 continued their usual treatment unchanged.
Results: After 1 year training maintained maximum aerobic capacity, while it decreased significantly in the untrained group (p=0.014). Voorrips’ activity score was correlated with VO2max (r= 0.44, p= 0.05) and with the distance walked at 6MWT (r=0.446, p=0.05). The distance walked during 6MWT is correlated with VO2max before (r= 0.456 p= 0.05) and after (r= 0.714 p<0.001) and on all values measured before and after (r= 0.571 p= 0.01). The change in MWT does not predict that of VO2max to which it is not correlated (r=0.318; NS), but it is weakly correlated to that of the VT1 (r= 0.435 p-0.05) while the absolute values of VT1 and 6MWT are not correlated at all. 6MWT was not correlated with HbA1c.
Conclusions: as in other sedentary populations, 6MWT is an indicator (approximate but easy and economical) of aerobic fitness. However, it does not measure training-induced changes in aerobic fitness, its variations being rather a marker of those of the first ventilatory threshold.
The six-minute walk test (6MWT) is a simple and costless measure of physical fitness which was proposed in the 80’s [1]. It has later been shown to be correlated with maximum oxygen consumption (VO2max) in healthy individuals [2,3] and also to reflect the ability to oxidize lipids at exercise [4]. Since it has been widely studied and validated in chronic pathologies associated to sedentary lifestyles [5-8], it appears to be logically more and more employed in diabetes studies [9]. However, the basis for this use was until recently poorly documented. Recently three papers evidenced relationships between 6MWT and maximal oxygen uptake (VO2max) in specific groups of diabetic patients [10-12]. All of them concluded that 6MWT is correlated to VO2max and concluded that it can be employed as a marker of aerobic capacity. However, these encouraging reports are still preliminary. They rely on quite limited samples of subjects: 54 South-Korean T2D women aged 50-70 years [10], 18 north American T2Ds included in the randomized controlled trial ACTIVE II [11] and 42 Spanish T2M with a mean age of 61.1 years [12]. Whether conclusions of these studies in selected populations can be safely extended to other populations remains to be more investigated. In addition, whether the evolution of 6MWT after training reflect a change in VO2max remains unknown, and this is a fundamental question to address before counselling the wide use of 6MWT as a reliable surrogate of aerobic working capacity measurements.
VO2max is an important physiological parameter [13], since it is the most recognized index of cardiorespiratory fitness, whose impairment is associated with many adverse health outcomes. By contrast the measurement of VO2max requires a maximal exercise-test which cannot be performed everywhere and requires a specific and expensive material. Therefore, reliable surrogates providing an evaluation of cardiorespiratory fitness are useful for a comprehensive assessment of an individual’s health, and 6MWT is surely one of the most attractive because it is simple to realize and costless [1,5-8]. If it were also a good reflect of health improvement after treatment its interest would be even greater but this remains unknown for diabetics, since in this disease there are several factors of disability (eg, neuropathy, retinopathy). That are not directly linked with cardiorespiratory fitness.
The database of a previous study of training in diabetics [14] in order to investigate the cost-reducing effect of exercise in T2D provides us an opportunity to answer to those two important questions:
a) Is the previously reported correlation between 6MWT and VO2max confirmed in this separate sample, supporting the idea that this relationship should be expected to exist in the general population of T2D?
b) Is a change in MWT after training a reliable predictor of an improvement un working aerobic capacity in these patients?
Materials and methods
Study participants
This study is part of a wider study investigating the effects of exercise training individually targeted at the level of VT1 on healthcare costs for chronic diseases, that included 112 patients: 45 with chronic obstructive pulmonary disease (COPD), 32 with chronic heart failure, and the 25 with type 2 diabetes. The sample of 25 type 2 diabetics is presented on Table 1. More data can be found in the paper presenting all the results and investigating the main endpoint of the trial [14].
Patients routinely followed by their general practitioner were recruited into the study. Diabetes was defined according to the to the 1997 criteria of the American Diabetes Association [14]. Patients were eligible for the study if they were aged 40–85 years and if they fulfilled the following criteria:
• Treatment with oral hypoglycaemic agents or diet alone, and not with insulin therapy;
• HbA1c level between 8 and 10%;
• No change in any medication for the past three months;
• No history of ketoacidosis.
Patients with congestive heart failure, a recent episode of ischemic heart disease, peripheral vascular disease, current malignancy, chronic renal failure, severe proliferative diabetic retinopathy or any physical and mental conditions that may have an influence on the ability of the patient to participate in the intervention were excluded. The study protocol was approved by the institutional review board of the University Hospital of Montpellier. All patients gave their informed consent to participate in the study.
Body composition
The patients were measured, weighed on a Sartorius F1505-F2 balance scale and had their waist circumference measured at the umbilicus. Body composition was assessed with a four-terminal impedance plethysmograph (Dietosystem Human IM-Scan, Milan, Italy), which minimizes contact impedance and skin-electrode interactions. Measurements were taken in fasting patients after 15 minutes of rest in a supine position. A low-intensity (100–800μA) current was introduced at various frequencies (1, 5, 10, 50 and 100 kHz), and measurement of the voltage drop allowed determination of the total body impedance rate. These values are then used with specially designed software to calculate body water (intra- and extracellular), fat mass, fat-free mass and body cell mass [16].
Exercise testing
The patient’s VO2max was measured during 8–12 minutes of exercise performed on an electronically braked cycloergometer (550 ERG, Bosch, Germany). During exercise, gas exchanges were measured breath by breath, using a mass spectrometer (Marquette MGA 1100, France). The calibration of the mass spectrometer was checked before each test with standard calibration gases. A 3-L syringe was used to calibrate the volume turbine, using flow rates similar to the patient’s ventilation. Heart rate was monitored throughout the exercise test, which started with a six-minute warm-up at 20% of the theoretical maximum power output. The workload was then increased by steps of 8% of Pmax per minute until the maximum exercise level was reached, which was then evaluated in terms of maximum heart rate, Respiratory Exchange Ratio (RER) (>1.15) and O2 consumption (VO2) stability. The results of this test were used to determine the first ventilatory threshold (VT1) according to the method used by Beaver, et al. [17], and [18]. The maximum theoretical oxygen consumption (VO2max th) and, thus, the theoretical Pmax were also calculated, according to Wasserman’s equations [19]. Criteria for defining VO2max and VT1 were taken from the standardization consensus guidelines of the French Society of Sports and Exercise Medicine [18,20].
The six-minute walking shuttle test (6 MWT) was conducted as described by Guyatt, et al. [1,21]. Using a corridor in the outpatients clinic, a 15-meter course was marked out, placing a chair at each end. The decision whether the patient was fit enough to take the 6 MWT was made by the attending cardiologist. Patients were instructed to walk at their own pace from end to end while attempting to cover as much ground as possible in the allotted six-minute time period. A physiotherapist clocked the walking and called out the time every two minutes, while also encouraging the patient on. Patients were allowed to rest, but were instructed to carry on walking as soon as they were able to do so. After six minutes, patients were instructed to stop walking, and their total distance was measured to the nearest meter. Any symptoms experienced by the patient during this test were also recorded. Blood pressure was measured before and after the test.
Physical activity level was assessed using the Voorrips questionnaire [22].
Training intervention
This was a parallel-group, randomized trial. On Day 1, patients were randomly assigned to one of two groups using a computer-generated list of random numbers. In the intervention group, patients were told to follow the training programme while, in the control group, the intervention consisted of repeated evaluation of fitness, healthcare cost assessment and metabolic parameters. Patients in both groups continued to be managed by their own primary-care physician, and there was no study interference with the physicians’ therapeutic choices. The only modification from the study was the addition of structured exercise training in the intervention group. All treatments, health events and hospitalizations were recorded by the investigators at each visit for calculation of the healthcare costs.
The structured training programme comprised of an educational period of one month, followed by training at home. The educational period involved eight two-hour sessions over four weeks, when a trained professional, during the first hour, explained to the patient the purpose of the training and how it should be performed. The second hour was devoted to actually learning the exercise that the patient had to perform - in this case, cycling at the level of the ventilatory threshold for 30–45 minutes at a time. After this learning session, the patient had to train at home twice a week at a level defined by heart rate. All participants performed, at their own convenience, brisk walking, jogging or gymnastics for 45 minutes at this target heart rate, as determined by a heart-rate monitor.
To ensure “realistic” conditions of training, the actual practice of the physical activity was recorded: everyday, patients had to keep track of all their activity in a notebook, and fill in Voorrips questionnaires on Days 120, 240 and 365.
Both study groups were followed over the course of the year by evaluations at 30, 120, 240 and 365 days to determine healthcare costs, blood pressure, spirometry, glycaemic and lipid equilibrium, 6 MWT, and exercise [16] and QOL questionnaires. A further maximum-level exercise test to determine VO2max and ventilatory threshold was performed at Day 0 and Day 365 as described above.
Statistical analyses
Data are shown as means ± S.E.M. Statistical analysis was performed with Sigmastat (https://systatsoftware.com/products/sigmastat/) and the Bland-Altman and Altman plot was done with the freeware “method validator” Philippe Marquis (https://method-validator.software.informer.com/). Correlation analyses were performed on EXCEL.
Results
On entering the study, the participants appeared to have similar values of HbA1c (8.8% ± 1.38 versus 8.77 ± 0.98%), fasting blood glucose, weight, height, BMI, waist circumference and blood pressure. As previously reported [13], after 1 year of targeted training protocol, trained subjects maintained their maximum aerobic capacity, while this capacity significantly decreased in the untrained group (p=0.014). Distance walked during the 6 MWT did not decrease in the trained group and became significantly higher in this group than in the untrained group at the end of the period of training. Voorrips’ activity score was correlated with VO2max (r=0.44, p=0.05), as well as with the distance walked during the 6MWT (r=0.446, p<0.05).
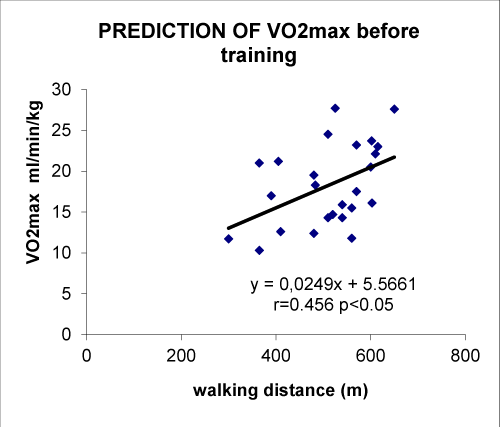
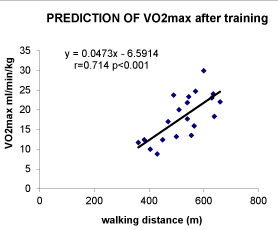
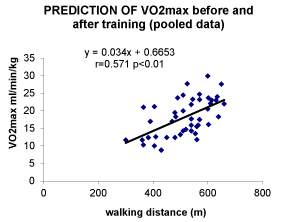
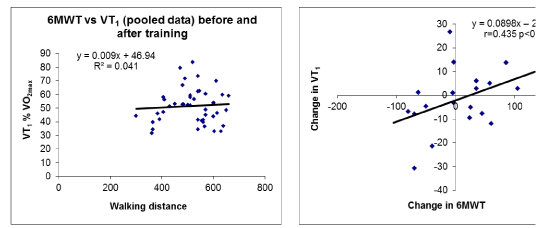
As shown on Figure 1, walking distance measured during the 6MWT is correlated with VO2 max before (r=0.456 p<0.05). This correlation is also found after training as shown on Figure 2 (r-0.714 p<0.001). When pooling values obtained before and after training there is also a highly significant correlation (r=0.571 p<0.01) as shown on Figure 3. From the latter correlation analysis we can propose a prediction of VO2 max with the equation:
VO2max = 0.034 [6MWT] + 0.6653
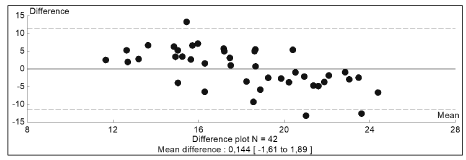
where VO2max is expressed in ml/min/kg and 6MWT in meters. On Figure 4, we show the Bland-Altman plot evaluating the agreement between actual VO2max and VO2max predicted by the abovementioned equation. It can be seen that differences between predicted and actual VO2max are well centered around the central line but that the range of differences is rather high (-12 to+12 ml/min/kg).
Since an equation predicting VO2max from 6MWT and weight was proposed in Lee’s paper [10], we tested this equation in our sample. The equation is:
VO2max = 14.986 + 0.025 [6MWT] -0.161 weight.
Actually these correlations did not reach significance. Before training we found r=0,274 (NS), after training we found r=0,339 (NS) and for values before and after pooled together we found r= 0,299 (NS). Therefore this equation proposed in a South Korean population doesn’t work in our sample.
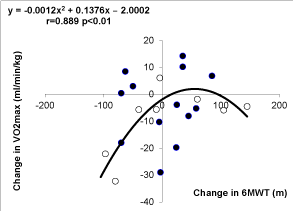
We also looked for correlations between changes in 6MWT and changes in VO2max and VT1. As shown on Figures 5,6, changes in 6MWT-derived walking distance in the patients of the study before and after 1 year of individualized training (pooled data) are not linearly correlated with changes in VO2max (r=0,317 NS) but if a nonlinear model is applied a highly significant polynomial relationship is evidenced, showing that the change in MWT may predict the decrease in VO2max but not an improvement in VO2max.
By contrast changes in MWT after 1 year are not correlated with those of VO2max despite a loose tendency (r=0.318; NS). These changes are by contrast weakly correlated to that of the Sv1 (r=0.435 p<0.05) while the crude values of SV1 and 6MWT are not correlated.
We also looked for correlations between 6MWT and HbA1c since such correlations were reported in previous papers. We found no correlation at all with r values as low as r=0.0216 before training; r=0.099 after training and r=0.037 for values before and after pooled together.
Discussion
This study shows that, as already reported other sedentary populations [5-8] and in healthy individuals [2-3], 6MWT is an index, approximative but easy to obtain and inexpensive, of aerobic working capacity. Actually, we also show that post-training changes in 6MWT are unable to reflect the training-induced changes in VO2 max and rather reflect changes in ventilatory threshold.
These findings are useful for investigators using more and more the 6MWT test in diabetic patients, because there is a tendency to consider that this test is an accurate monitoring of aerobic capacity and some recent papers could lead to think so [10-12]. Actually we demonstrate that this is not fully exact and that although the walking distance provided by the test is correlated to VO2max, changes in those two parameters after training are poorly related. An improvement in walking distance in diabetics does not closely reflect an improvement in VO2max.
This study is part of a wider study investigating the effects of exercise training at the level of VT1 and one of the findings was that VO2max declined by 16.4%, over 1 year without training while this decline was prevented by training. Although it is well accepted that diabetes is a progressive disease [23], such a rapid decline highlights the “vicious circle” of a sedentary lifestyle in chronic diseases [24], and characterized by rapid deterioration even at the stage of disease where patients are comparatively healthy. In this regard, it is noteworthy that our “realistic” lifestyle intervention, albeit not particularly aggressive, was nonetheless able to prevent such a decline.
This important finding of a preventing effect on training on the decline in VO2max in T2D is not clearly found with our 6MWT data, but a close look at the data suggests that this may become significant on a larger sample.
Nevertheless, as shown on Figure 4, 6MWT seems to be sensitive to a decrease in VO2max and thus may be helpful for detecting an impairment in aerobic capacity in this population. By contrast it is not sensitive to an increase in VO2max and cannot detect it.
In fact, it is not surprising to find some discrepancies between 6MWT and VO2max data, which by essence are not the same measurement and cannot provide exactly the same information. Correlations between VO2max and 6MWT found in the 3 previous studies [10-12] yield quite the same values of coefficients of correlation, ranging between 0.456 and 0.66. Nolen-Doerr [11] analyses this fact as reflecting that 6MWT distance alone ‘explains’ 45% of the variance of VO2max, so that 55% of this variance is not ‘explained’ by it.
Interestingly, Nolen-Doerr [11], reports a higher coefficient of correlation after training (r=0.66) compared to pre-training (r=0.57), and this is fully consistent with the current study which shows r=0.456 before training and r=0.714 after training. This may reflect an improvement in cardiovascular regulatory adaptation to exercise strengthening the agreement between the two measurements.
In contrast to other studies we were unable to evidence a correlation between diabetic control as measured by HbA1c and the 6MWT. There was absolutely no correlation between these two parameters. Such a correlation was reported by Ramírez Meléndez [12] and is logic to expect since poor glucose control drives the complications of diabetes which in turn induce disability. However, in samples of patients like those of the study, who are followed regularly, this correlation can be hidden by recent improvements in blood glucose control.
Both VO2max and 6MWT are indexes of fitness whose interest in chronic disease is obvious, because they integrate a host of factors and represent an overall evaluation of health. This was impressively demonstrated some years ago by the correlation between VO2max and insulin sensitivity [25]. Therefore, measuring a parameter of fitness that integrates cardiovascular, respiratory and metabolic health is surely important in diabetics, although this is not yet systematic. In this respect measuring 6MWT offers the advantage of easiness and low cost, and it is clear that this measurement provides an important information.
Attempts to derive from crude 6MWT data an accurate prediction of VO2max provide quite deceiving results, and it is probably better to consider that those two parameters have not exactly the same meaning and should not be considered as equivalent.
This study has strengths and limitations. One of the strengths is to present precise measurements of VO2max obtained during a maximal exercise test before and after a period of training and with an untrained control group. The randomized design of the study is also a strength. We think that the duration of one year of the study is more relevant to real life healthcare than a shorter period as often found in training studies. Clearly, training needs to be applied for long periods in patients, and short-term training studies in chronic diseases barely reflect this reality. Another strength of the study is that it was designed to represent the average population of type 2 diabetics of our country, although it is clear that T2DM occurs more and more earlier in western countries. By contrast, a limitation of the study is that it was designed for assessing training-induced changes in healthcare costs and not for comparing 6MWT and VO2max. Therefore, the number of subjects was not calculated before the study for this purpose. This may induce a risk of type-2 error, as discussed above concerning the lack of training effect on 6MWT which contrast with the training-induced prevention of a decline in VO2max which is clearly evidenced. It is likely that a greater number of subjects would allow us to evidence a training effect on 6MWT. Nevertheless, it is clear than the two parameters do not evolve in close parallelism and that they have not exactly the same meaning.
More precisely, we can say that our study fully confirms the precedent report of some degree of correlation between 6MWT and VO2max but also points out the discrepancy between these two parameters which have not exactly the same relevance. 6MWT can provide an estimate of an individual’s fitness in chronic diseases, and it is clear that this is an interesting and useful marker of health. By contrast, changes in 6MWT may reflect other improvements than those of aerobic working capacity and are not a tool do precisely detect such improvements in diabetes.
This study was funded by a grant from the French Ministry of Health and also received financial support from LVL Medical, France.
- Guyatt GH, Sullivan MJ, Thompson PJ, Fallen EL, Pugsley SO, et al. (1985) The six-minute walk: a new measure of exercise capacity in patients with chronic heart failure. Can Med Assoc J 132: 919-923. Link: https://bit.ly/2Zf3On3
- Mänttäri A, Suni J, Sievänen H, Husu P, Vähä-Ypyä H, et al. (2018) Six-minute walk test: a tool for predicting maximal aerobic power (VO2 max) in healthy adults. Clin Physiol Funct Imaging 38: 1038-1045. Link: https://bit.ly/3eeGolK
- Hong SH, Yang HI, Kim DI, Gonzales TI, Brage S, et al. (2019) Validation of Submaximal Step Tests and the 6-Min Walk Test for Predicting Maximal Oxygen Consumption in Young and Healthy Participants. Int J Environ Res Public Health 16: 4858. Link: https://bit.ly/2Ocgapm
- Makni E, Moalla W, Trabelsi Y, Lac J, Brun JF, et al. (2012) Six-minute walking test predicts maximal fat oxidation in obese children. Int J Obes (Lond). 36: 908-913. Link: https://go.nature.com/3e9nbSJ
- Poulain M, Durand F, Palomba B, Ceugniet F, Desplan J, et al. (2003) 6-minute walk testing is more sensitive than maximal incremental cycle testing for detecting oxygen desaturation in patients with COPD. Chest 123: 1401-1407. Link: https://bit.ly/2ZKwRO4
- Donini LM, Poggiogalle E, Mosca V, Pinto A, Brunani A, et al. (2013) Disability affects the 6-minute walking distance in obese subjects (BMI>40 kg/m2). PLoS One 8: e75491. Link: https://bit.ly/3gEPMko
- Kirkham AA, Pauhl KE, Elliott RM, Scott JA, Doria SC, et al. (2015) Utility of Equations to Estimate Peak Oxygen Uptake and Work Rate From a 6-Minute Walk Test in Patients With COPD in a Clinical Setting. J Cardiopulm Rehabil Prev 35: 431-438. Link: https://bit.ly/325NHdn
- Kerti M, Balogh Z, Kelemen K, Varga JT (2018) The relationship between exercise capacity and different functional markers in pulmonary rehabilitation for COPD. Int J Chron Obstruct Pulmon Dis 13: 717-724. Link: https://bit.ly/2AGS17m
- Abraham WT, Ponikowski P, Brueckmann M, Zeller C, Macesic H, et al. (2019) EMPERIAL Investigators and National Coordinators. Rationale and design of the EMPERIAL-Preserved and EMPERIAL-Reduced trials of empagliflozin in patients with chronic heart failure. Eur J Heart Fail 21: 932-942. Link: https://bit.ly/31YHaAZ
- Lee MC (2018) Validity of the 6-minute walk test and step test for evaluation of cardio respiratory fitness in patients with type 2 diabetes mellitus. J Exerc Nutrition Biochem 22: 49-55. Link: https://bit.ly/3edlO5o
- Nolen-Doerr E, Crick K, Saha C, de Groot M, Pillay Y, et al. (2018) Six-Minute Walk Test as a Predictive Measure of Exercise Capacity in Adults with Type 2 Diabetes. Cardiopulm Phys Ther J 29: 124-129. Link: https://bit.ly/2Z9PJqN
- Ramírez Meléndez A, Arias Vázquez PI, Lucatero Lecona I, Luna Garza R (2019) Correlation between the six-minute walk test and maximal exercise test in patients with type ii diabetes mellitus. Rehabilitacion (Madr) 53: 2-7. Link: https://bit.ly/2CjpwNH
- Zeiher J, Ombrellaro KJ, Perumal N, Keil T, Mensink GBM, et al. (2019) Correlates and Determinants of Cardiorespiratory Fitness in Adults: a Systematic Review. Sports Med Open 5: 39. Link: https://bit.ly/38Mpvhh
- Brun JF, Bordenave S, Mercier J, Jaussent A, Picot MC, et al. (2008) Cost-sparing effect of twice-weekly targeted endurance training in type 2 diabetics: A one-year controlled randomized trial. Diabetes Metab 34: 258-265. Link: https://bit.ly/3f8HctM
- Report of the expert committee on the diagnosis and classification of diabetes mellitus (1997) Diabetes Care 20: 1183-1197. Link: https://bit.ly/31YjD3d
- Brun JF, Guiraudou M, Mardemootoo C, Traore A, Raingeard I, et al. (2013) Validation de la mesure segmentaire de la composition corporelle en comparaison avec la DEXA: interêt de la mesure de la masse grasse tronculaire. Sci Sports 28: 158-162. Link: https://bit.ly/2Zd2FfJ
- Beaver WL, Wasserman K, Whipp BJ (1986) A new method for detecting anaerobic threshold by gas exchange. J Appl Physiol 60 : 2020-2027. Link: https://bit.ly/3iJGyoP
- Vallier J, Bigard X, Carré F, Eclache J, Mercier J (2000) Détermination des seuils lactiques et ventilatoires. Position de la Société française de médecine du sport. Sci Sports 15: 133-140. Link: https://bit.ly/2ZPNAzD
- Wasserman K, Hansen J, Sue D, Whipp B (1987) Principles of exercise testing and interpretation. Lea & Febiger, Philadelphia.
- Lampert E (1998) Erreurs à ne pas commettre lors de la réalisation d’un exercice de détermination de la consommation maximale d’oxygène. Sci Sports 13: 193-201. Link: https://bit.ly/3e6FA2s
- Singh SJ, Puhan MA, Andrianopoulos V, Hernandes NA, Mitchell KE, et al. (2014) An official systematic review of the European Respiratory Society/American Thoracic Society: measurement properties of field walking tests in chronic respiratory disease. Eur Respir J 44: 1447-1478. Link: https://bit.ly/3gH9OL7
- Voorrips LE, Ravelli AC, Dongelmans PC, Deurenberg P, Van Staveren WA (1991) A physical activity questionnaire for the elderly. Med Sci Sports Exerc 23 : 974-979. Link: https://bit.ly/2W26Mcr
- UK prospective diabetes study 16 (1995) Overview of six years’ therapy of type II diabetes: a progressive disease. U.K. Prospective Diabetes Study Group. Diabetes 44: 1249-1258.
- Serres I, Hayot M, Prefaut C, Mercier J (1998) Skeletal muscle abnormalities in patients with COPD: contribution to exercise intolerance. Med Sci Sports Exerc 30: 1019-1027. Link: https://bit.ly/2W1QPTt
- Clausen JO, Borch-Johnsen K, Ibsen H, Bergman RN, Hougaard P, et al. (1996) Insulin sensitivity index, acute insulin response, and glucose effectiveness in a population-based sample of 380 young healthy Caucasians. Analysis of the impact of gender, body fat, physical fitness and life-style factors. J Clin Invest 98: 1195-1209. Link: https://bit.ly/320DtLi
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
