Annals of Musculoskeletal Medicine
A case study of the association between adolescent idiopathic scoliosis, weight training and shoulder dislocation
1Romanian Academy, Institute of Biology, 296 Independence Square, Bucharest, Romania
2Fellow of the Research Institute of the University of Bucharest, ICUB, Bucharest, Romania
Author and article information
Cite this as
Constantin M (2023) A case study of the association between adolescent idiopathic scoliosis, weight training and shoulder dislocation. Ann Musculoskelet Med. 2023; 7(2): 4-8. Available from: 10.17352/amm.000031
Copyright License
© 2023 Constantin M. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.This study shows a rare association between the anomalous position of the shoulder girdle, due to scoliosis, with altered shoulder kinematics, injury of joint capsule ligaments and rotator cuff tendons, and shoulder dislocation due to a traumatic event. The subject has developed adolescent idiopathic scoliosis, with convex curvatures to the right side in the lower region of the thorax (with the Cobb angle of 13 degrees) and to the left side of the upper region of the thorax (with the Cobb angle of 24-degrees), both of them with the axial rotation of vertebra and with visible gibbosities. The upper axial rotation has a 6.5-degree, which causes an unbalance between the two shoulder girdles. In normal situations, the shoulder joint is turned 30 degrees anterior to the coronal plane, but in his case, the right shoulder girdle is pulled 28 degrees anterior by the groove, and the left one is pushed 34.5 degrees anterior by the gibbosity. The major effect of shoulder girdle unbalance appears to be the maximum extension of the upper limbs when the hands can’t be aligned to the coronal plane and this is an important risk factor for the injuries of the left shoulder joint, while some weight training exercises are performed.
Scoliosis
Scoliosis is a lateral (i.e. on the frontal or coronal plane) deviation of the spinal column, consisting of developing lateral curvatures and axial rotation of vertebrae [1-4]. The development of scoliosis starts with the onset of the primary curvature, which has the tendency to persist even when the subject is supine or hanging by the arms [3]. In the superior and/or inferior position of primary curvature, sometimes there are developing compensation curvatures, giving the spine an S shape. Physiological scoliosis with angles up to 10° is common in the general population [4], due to unbalanced use of the upper limbs, but pathological scoliosis with angles greater than 10° can be developed by 2% - 3% of the growing age population [1,3], being more frequent in the girls [3,5]. In a standing or sitting position, scoliosis can be observed upon asymmetry of the shoulders and in anterior flexion of the trunk, upon the unilateral gibbosity developed in the thoracic region of the spine.
Scoliosis can develop in utero or after birth, during periods of rapid growth of the body, in infancy, or at the onset of puberty [6]. Scoliosis affects almost equally children of both sexes, but after the age of 10 (adolescent idiopathic scoliosis), the ratio changes to 6:1 for girls. It has genetic, neuromuscular, syndrome-related, dysmetabolic, and osteopathic causes or it can be associated with no known cause (idiopathic scoliosis), the latter being the most prevalent by far [1,3]. Idiopathic scoliosis is a > 10° curvature of the spine in the frontal plane, being a common spinal deformity [7] and having no obvious cause. Also, it could be associated with some spinal traumatic events in childhood, some being minor and often going unnoticed. It occurs at the thoracic level, is associated with some degree of lordosis, is often C-shaped (i.e., it is characterized by the presence of a single, long, right-convex curvature) than S-shaped, and always involves vertebral rotation (i.e., the body of the vertebrae are rotated towards the convex side of the curvature and the vertebral arches are rotated towards the concave side of the curvature) and rib deformities [8], causing a gibbosity on the convex side of the curvature. Ninety percent of all idiopathic scoliosis are reported in adolescents, affecting 2 to 5 percent of children between 10 and 16 years of age [9-11], girls being more likely to develop severe forms (i.e., the greater angle of primary curvature, with poor prognosis) than the boys (ratio of up to 10:1 for the girls). Mild scoliosis tends to affect both sexes almost equally, with a ratio of 1.5:1 for girls [5,12].
Shoulder dislocation
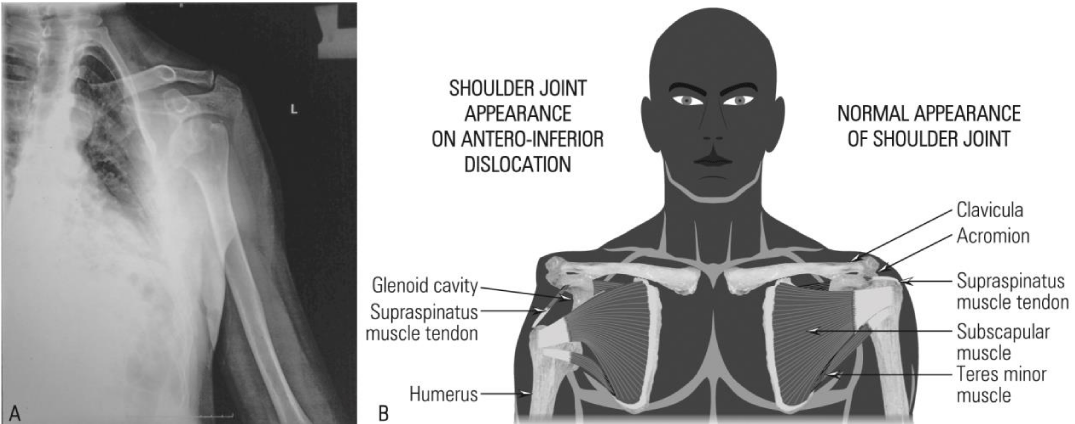
The glenohumeral joint is by far the most freely moving joint in the body, because of its conformation. The humeral head is spherical and fits only in part inside the glenoid cavity of the scapula. The surface of the glenoid cavity is deepened by the glenoid labrum, a fibrocartilage ring that borders it and gives more stability to the joint. On the upper side of the joint is located the strong coracohumeral ligament, which supports the weight of the upper limb, and in the front of the joint, there are three weak glenohumeral ligaments, whose contribution to the joint stabilization is insignificant. The main role in shoulder joint stabilization is played by muscle tendons: the biceps brachii, and the rotator cuff (the supraspinatus, the infraspinatus, the subscapular, and the teres minor) [13].
Shoulder dislocations are the most common joint injuries, accounting for 45% of all large joint dislocations [14]. Due to the weakness of the anterior and inferior reinforcements, the shoulder joint often tends to dislocate in an anterior and inferior direction [13] (Figure 1).
Case report
Three hours after suffering a trauma, a 19-year-old male student was brought consciously to the Emergency Department with his left arm kept in internal rotation by his right arm, feeling intense pain inside the left shoulder and with the inability to move his left upper limb. The injury occurred when the subject stumbled over a wire and fell down from a snow drift, bedding on his both arms. At that moment, the subject heard a crackling followed very quickly by a crack, he felt very intense pain inside his left shoulder, and, because of this, he couldn’t rise straight, but only with his trunk bowed forward.
By shoulder self-palpation, the subject found a concavity in the deltoid area, an “empty glenoid”, which appeared consequent to the humerus head detachment from its socket, which was found in the anterior and inferior position. He reported that two months prior to the shoulder dislocation, he performed front raises and pullovers, missing the warm-up stage before training. He lay on the flat bench, got the barbell in pronation with medium grip, and placed it on the upper side of his thighs. He raised the barbell and performed a 180-degree semicircular motion, until the barbell was horizontally above his head, keeping the elbows fully extended throughout the entire motion. He kept the barbell in this position for a second and after that, he started to raise it again, to go back to the initial position. While he started the positive movement (rising motion), he heard a crackling and felt very intense pain inside his left shoulder, due probably to a light form of the sprain. The difference in extension capacity between the two glenohumeral joints and the strain in the left shoulder, which was too intense for the rotator cuff to cope with, led to tendons tearing of anterior members of rotator cuff muscles (subscapular and/or teres minor). At the same time, some ligaments of the glenohumeral complex could be elongated or broken, especially those on the inferior side of the glenoid cavity.
After two weeks, while performing the same exercise in similar conditions (i.e., missing the warming-up stage), the injury took place again, probably due to a new tear in the same tendons or ligaments or to the exacerbation of the first ones.
After six weeks, the subject stumbled over a wire and fell down from a snow drift, causing the shoulder dislocation. When falling down, the subject helped himself with his arms, pressing with left elbow against the snow drift. In abduction, the left shoulder joint became quickly overextended and the humerus head pushed against the acromion, to a lever movement, leading the glenohumeral complex to be elongated and some ligaments to be broken, when the subject heard the crackling. The sound of the crackling was similar to one breaking a chicken joint when eating meat. After the two injuries, the weakened joint has become more mobile and this helped to tear rotator cuff tendons at the moment of the fall. When his body lay down on the left side, due to the pain and left-arm lack of support, the humerus was suddenly pulled back by supraspinatus and infraspinatus muscle tendons towards its glenoid socket, but it was blocked by the anterior crest of the glenoid labrum, producing the crackling which the subject heard.
After the trauma, the most “comfortable” position for the subject was bending the trunk in the front, which allowed the arm to rest in anterior abduction. After one hour, the intensity of the pain decreased and he could raise his trunk almost completely only if his right hand supported the left arm.
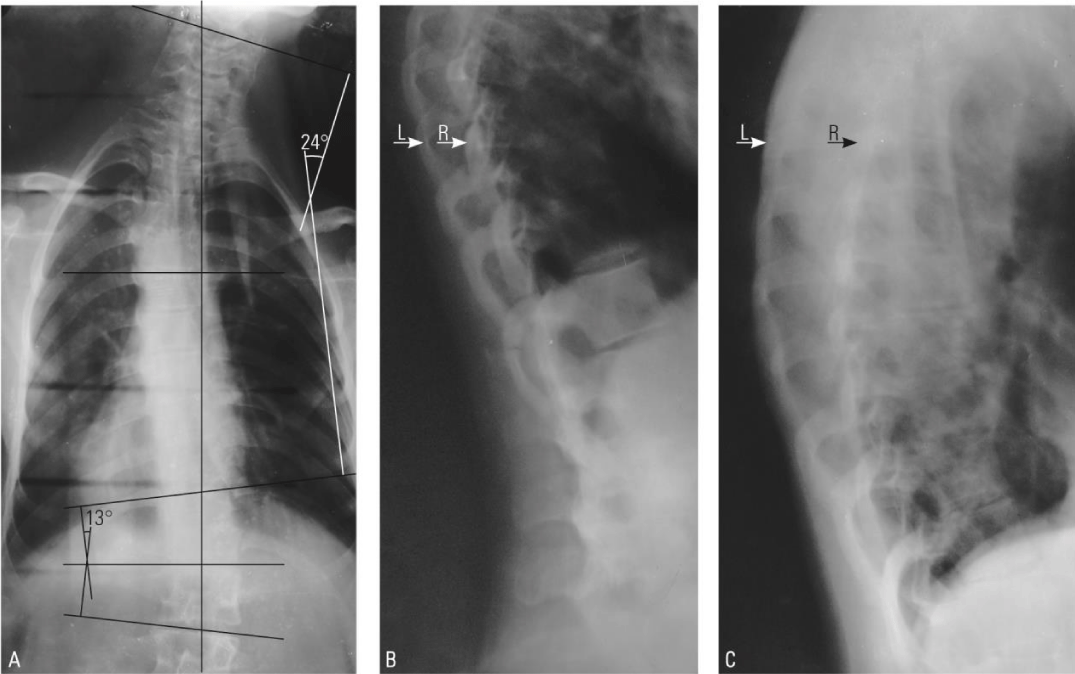
Because of the intense pain, the shoulder dislocation was reduced under general anesthesia with atropine. Meanwhile, it could be observed that the subject is affected by idiopathic S-shaped scoliosis type 3C, according to King and Moe criteria [15,16]. It has convex deviations in the left upper region (with the Cobb angle of 24°) and right lower region (with the Cobb angle of 13°) of the trunk (Figure 2), with a left-side better-developed gibbosity in the upper part of the rib cage (the difference between left and the right side is about 6.5°) and a right-side smaller gibbosity on the lower part of the rib cage (the difference between the left and right side is below 2°). On the opposite side of the humps, the rib cage has developed slight grooves. Meanwhile, he recalled that, at the age of 7 or 8, he was picked up by an older boy, lifted up, and dropped, while he blocked him with his foot so that he fell on his side. He was able to walk with difficulty for a few hours after the incident, after which he made a full recovery without any sequelae and didn’t take the incident into account. Although the diagnosis of idiopathic scoliosis was made, it is possible that this incident contributed to the onset of scoliosis.
The treatment of shoulder dislocation
The arm was internally rotated and the shoulder was immobilized in a chest-arm gypsum bandage, which was changed with a chest-arm simple bandage, 4 days after the trauma, due to the discomfort felt by the subject. After 21 days, the bandages were taken off and the joint was fully recovered, regaining its full range of motion.
After a break of seven months, the subject started to train again and realized that he was not able to bring down the barbell over the shoulders, and behind the neck, when performing standing/sitting barbell presses behind the neck. He reported weakness in his left shoulder that was felt on the lower stage of the motion. Since he replaced this exercise with another one, he had no other difficulty in performing his weight training, and at his last review at 7 years post-trauma, his shoulder was still asymptomatic; the subject did not investigate further the shoulder joint weakness.
Discussion
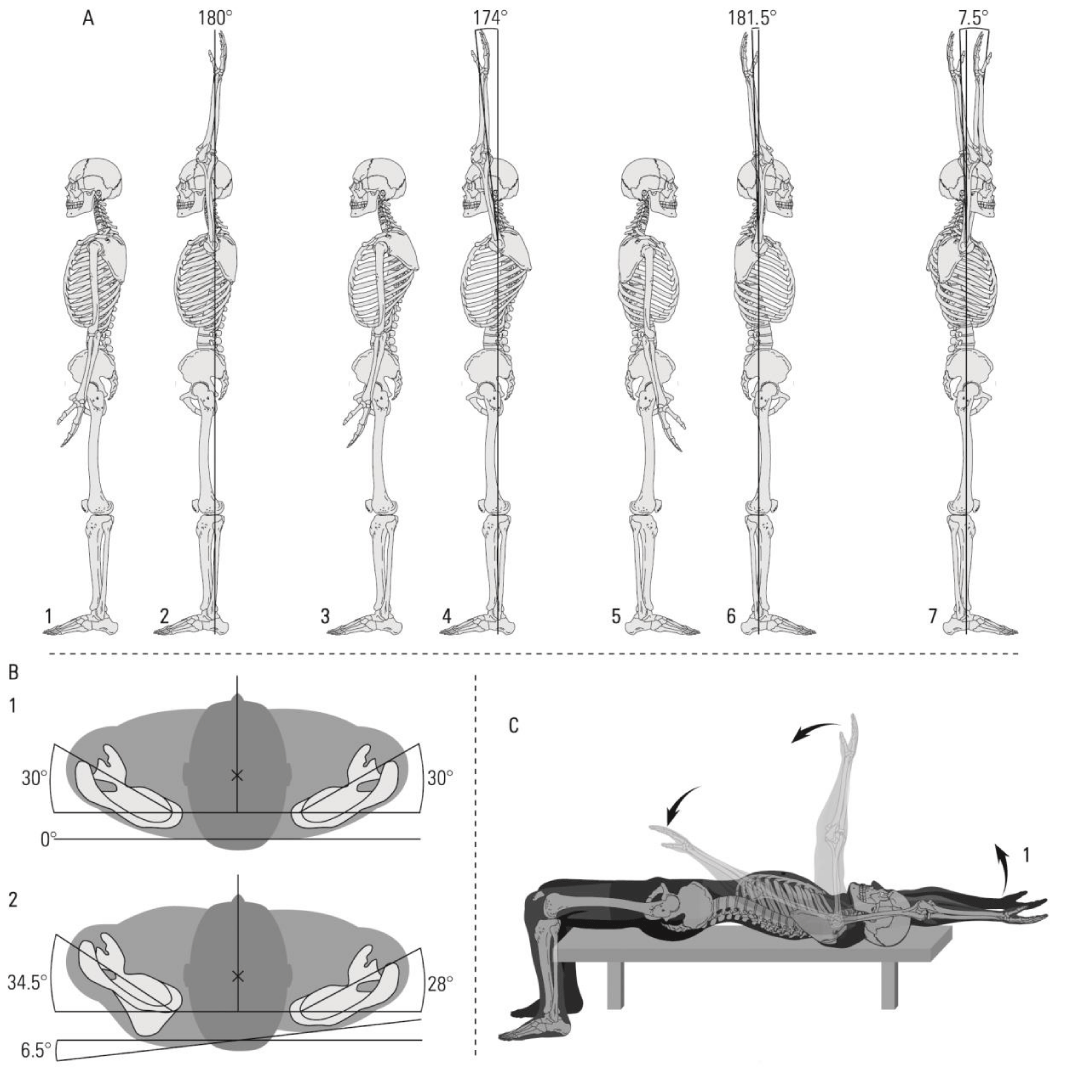
Although taken separately, scoliosis and scapulohumeral dislocation are not very rare events, the latter being somewhat more common (45% of all joint dislocations), their association is less common. In the literature, the occurrence of glenohumeral joint dysfunction and increased risk of subacromial impingement syndrome and rotator cuff pathology in idiopathic scoliosis are cited [17], with no association between scoliosis and shoulder dislocation, probably due to pain and marked limitation of joint mobility. The case presented here shows a rare association between scoliosis and shoulder dislocation. The spinal column of the subject has a left-side convex deviation in the upper part of the trunk (Figure 2A), leading to the asymmetry of the rib cage (Figure 2B,C) with upper left gibbosity and right depression, and imbalance of the pectoral arches. The position of the right scapula tends to be almost normal, with the medial border and inferior angle slightly pulled inward and the superior-lateral angle pushed only a little bit backward, allowing the right arm to go a little bit further in extension than is possible in the normal case (Figure 3A5-6, A7). On the other hand, the inferior angle of the left scapula is pushed outward by the hump, forcing its superior-lateral angle to fit in a position of protraction and internal rotation. Unfortunately, this situation limits somewhat the extension movements of the left arm, allowing the achievement of its maximum range a few degrees earlier than is possible in the normal case (Figure 3A3-4, A7, 3B2). For most people who do not practice any sustained physical activity, this limitation can be a source of back and shoulder pain, dysfunction, and altered kinematics of the shoulder joint [17-19], but for those who practice bodybuilding, where full movement extension is required, it can lead to accidents, as shown here.
Due to the presence of gibbosity in the superior left side of the rib cage and to the pectoral arches’ asymmetry, each arm of the subject has a different maximum extension range, causing an imbalance in the upper part of the motion. When trying to align both arms in the superior position, the subject forced the left arm to perform overextension, since the right arm fulfills its entire extension potential (Figure 3A7). This difference becomes more evident when the extension is performed using an overloaded barbell, in a supine position, as it is when performing front raises and pullovers (Figure 3C).
Conclusions and perspectives
This study shows the association between the anatomical conformation of the glenohumeral joint and its capacity to perform normal movements, in the presence of scoliosis. Because scoliosis modifies the symmetry of the rib cage and the conformation of pectoral arches, it can predispose to glenohumeral joint injuries, especially in subjects who are using them very intensively (i.e. athletes). In order to reduce the risk of injuries, these individuals should ask for physician advice before start practicing weight training. Also, all the subjects who practice weight training or any kind of sports should pay very much attention to the correct warm-up before starting the training, which prepares the body for the following effort and increases the mobility of the joints, significantly reducing the risk of injuries.
Consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images.
- Białek M. Conservative treatment of idiopathic scoliosis according to FITS concept: presentation of the method and preliminary, short term radiological and clinical results based on SOSORT and SRS criteria. Scoliosis. 2011 Nov 28;6:25. doi: 10.1186/1748-7161-6-25. PMID: 22122964; PMCID: PMC3286410.
- Janicki JA, Alman B. Scoliosis: Review of diagnosis and treatment. Paediatr Child Health. 2007 Nov;12(9):771-6. doi: 10.1093/pch/12.9.771. PMID: 19030463; PMCID: PMC2532872.
- Zaharia C, Dumitrescu D, Teculescu D. Scoliosis, Clinic, therapy, recovery. Medical Publishing House 1980; 196.
- Rinsky LA, Gamble JG. Adolescent idiopathic scoliosis. West J Med. 1988 Feb;148(2):182-91. PMID: 3279708; PMCID: PMC1026057.
- Trobisch P, Suess O, Schwab F. Idiopathic scoliosis. Dtsch Arztebl Int. 2010 Dec;107(49):875-83; quiz 884. doi: 10.3238/arztebl.2010.0875. Epub 2010 Dec 10. PMID: 21191550; PMCID: PMC3011182.
- Wise CA, Gao X, Shoemaker S, Gordon D, Herring JA. Understanding genetic factors in idiopathic scoliosis, a complex disease of childhood. Curr Genomics. 2008 Mar;9(1):51-9. doi: 10.2174/138920208783884874. PMID: 19424484; PMCID: PMC2674301.
- Lenz M, Oikonomidis S, Harland A, Fürnstahl P, Farshad M, Bredow J, Eysel P, Scheyerer MJ. Scoliosis and Prognosis-a systematic review regarding patient-specific and radiological predictive factors for curve progression. Eur Spine J. 2021 Jul;30(7):1813-1822. doi: 10.1007/s00586-021-06817-0. Epub 2021 Mar 26. PMID: 33772381.
- Hefti F. Pathogenesis and biomechanics of adolescent idiopathic scoliosis (AIS). J Child Orthop. 2013 Feb;7(1):17-24. doi: 10.1007/s11832-012-0460-9. Epub 2013 Jan 13. PMID: 24432054; PMCID: PMC3566249.
- Reamy BV, Slakey JB. Adolescent idiopathic scoliosis: review and current concepts. Am Fam Physician. 2001 Jul 1;64(1):111-6. PMID: 11456428.
- Marya S, Tambe AD, Millner PA, Tsirikos AI. Adolescent idiopathic scoliosis : a review of aetiological theories of a multifactorial disease. Bone Joint J. 2022 Aug;104-B(8):915-921. doi: 10.1302/0301-620X.104B8.BJJ-2021-1638.R1. PMID: 35909373.
- Mohamed M, Trivedi J, Davidson N, Munigangaiah S. Adolescent idiopathic scoliosis: a review of current concepts. Paediatrics and Child Health. 2022 Apr;32(4):119-126. doi: 10.1016/j.paed.2022.01.002.
- Konieczny MR, Senyurt H, Krauspe R. Epidemiology of adolescent idiopathic scoliosis. J Child Orthop. 2013 Feb;7(1):3-9. doi: 10.1007/s11832-012-0457-4. Epub 2012 Dec 11. PMID: 24432052; PMCID: PMC3566258.
- Marieb EN, Hoehn K. Anatomy & Physiology, 9th ed, Pearson, 2012; 1264.
- Saseendar S, Agarwal DK, Patro DK, Menon J. Unusual inferior dislocation of shoulder: reduction by two-step maneuver: a case report. J Orthop Surg Res. 2009 Nov 3;4:40. doi: 10.1186/1749-799X-4-40. PMID: 19883514; PMCID: PMC2775722.
- Ovadia D. Classification of adolescent idiopathic scoliosis (AIS). J Child Orthop. 2013 Feb;7(1):25-8. doi: 10.1007/s11832-012-0459-2. Epub 2012 Dec 25. PMID: 24432055; PMCID: PMC3566250.
- Lee GB, Priefer DT, Priefer R. Scoliosis: Causes and Treatments. Adolescents. 2022; 2:220–234. doi: 10.3390/adolescents2020018
- Rapp van Roden EA, Richardson RT, Russo SA, Rose WC, Chafetz RS, Gabos PG, Shah SA, Samdani AF, Richards JG. Shoulder Complex Mechanics in Adolescent Idiopathic Scoliosis and Their Relation to Patient-perceived Function. J Pediatr Orthop. 2018 Sep;38(8):e446-e454. doi: 10.1097/BPO.0000000000001207. PMID: 29975295.
- Lin JJ, Chen WH, Chen PQ, Tsauo JY. Alteration in shoulder kinematics and associated muscle activity in people with idiopathic scoliosis. Spine (Phila Pa 1976). 2010 May 15;35(11):1151-7. doi: 10.1097/BRS.0b013e3181cd5923. PMID: 20421854.
Article Alerts
Subscribe to our articles alerts and stay tuned.
 This work is licensed under a Creative Commons Attribution 4.0 International License.
This work is licensed under a Creative Commons Attribution 4.0 International License.


 Save to Mendeley
Save to Mendeley
